
- Current
- Browse
- Collections
-
For contributors
- For Authors
- Instructions to authors
- Article processing charge
- e-submission
- For Reviewers
- Instructions for reviewers
- How to become a reviewer
- Best reviewers
- For Readers
- Readership
- Subscription
- Permission guidelines
- About
- Editorial policy
Search
- Page Path
- HOME > Search
- Pathophysiology
- Relationships between Islet-Specific Autoantibody Titers and the Clinical Characteristics of Patients with Diabetes Mellitus
- Yiqian Zhang, Tong Yin, Xinlei Wang, Rongping Zhang, Jie Yuan, Yi Sun, Jing Zong, Shiwei Cui, Yunjuan Gu
- Diabetes Metab J. 2021;45(3):404-416. Published online July 21, 2020
- DOI: https://doi.org/10.4093/dmj.2019.0239
- 6,416 View
- 161 Download
- 4 Web of Science
- 4 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub Background Dysimmunity plays a key role in diabetes, especially type 1 diabetes mellitus. Islet-specific autoantibodies (ISAs) have been used as diagnostic markers for different phenotypic classifications of diabetes. This study was aimed to explore the relationships between ISA titers and the clinical characteristics of diabetic patients.
Methods A total of 509 diabetic patients admitted to Department of Endocrinology and Metabolism at the Affiliated Hospital of Nantong University were recruited. Anthropometric parameters, serum biochemical index, glycosylated hemoglobin, urinary microalbumin/creatinine ratio, ISAs, fat mass, and islet β-cell function were measured. Multiple linear regression analysis was performed to identify relationships between ISA titers and clinical characteristics.
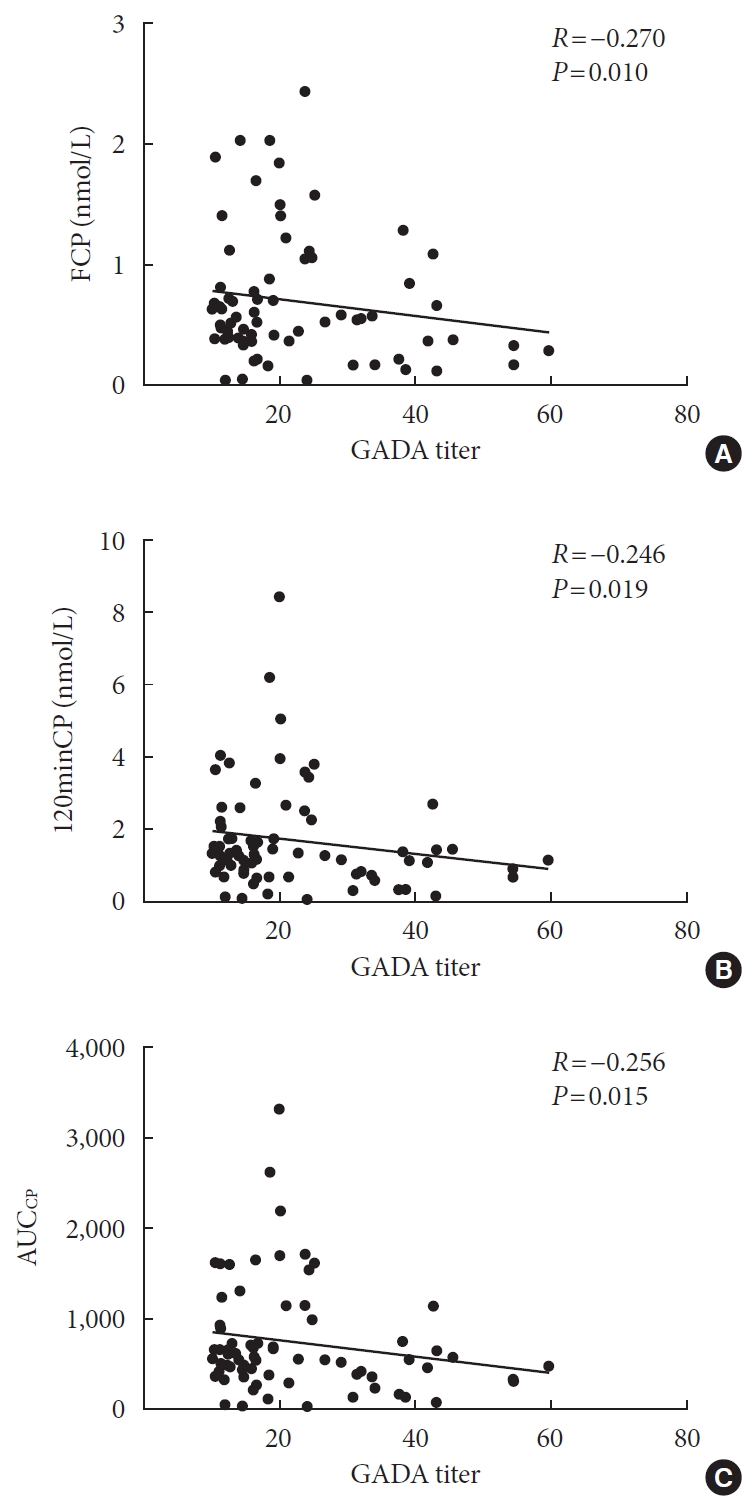
Results Compared with autoantibody negative group, blood pressure, weight, total cholesterol (TC), low density lipoprotein cholesterol (LDL-C), visceral fat mass, fasting C-peptide (FCP), 120 minutes C-peptide (120minCP) and area under C-peptide curve (AUCCP) of patients in either autoantibody positive or glutamate decarboxylase antibody (GADA) positive group were lower. Body mass index (BMI), waist circumference, triglycerides (TGs), body fat mass of patients in either autoantibody positive group were lower than autoantibody negative group. GADA titer negatively correlated with TC, LDL-C, FCP, 120minCP, and AUCCP. The islet cell antibody and insulin autoantibody titers both negatively correlated with body weight, BMI, TC, TG, and LDL-C. After adjusting confounders, multiple linear regression analysis showed that LDL-C and FCP negatively correlated with GADA titer.
Conclusion Diabetic patients with a high ISA titer, especially GADA titer, have worse islet β-cell function, but less abdominal obesity and fewer features of the metabolic syndrome.
-
Citations
Citations to this article as recorded by- Relationship between β-Cell Autoantibodies and Their Combination with Anthropometric and Metabolic Components and Microvascular Complications in Latent Autoimmune Diabetes in Adults
Tomislav Bulum, Marijana Vučić Lovrenčić, Jadranka Knežević Ćuća, Martina Tomić, Sandra Vučković-Rebrina, Lea Duvnjak
Biomedicines.2023; 11(9): 2561. CrossRef - RETRACTED ARTICLE: MiRNA-27a mediates insulin resistance in 3T3-L1 cells through the PPARγ
Yangming Zhuang, Ming Li
Molecular and Cellular Biochemistry.2022; 477(4): 1107. CrossRef - Correlation between Insulin Resistance and Microalbuminuria Creatinine Ratio in Postmenopausal Women
Han Na, Rong Wang, Hai-Long Zheng, Xiao-Pan Chen, Lin-Yang Zheng, Faustino R. Perez-Lopez
International Journal of Endocrinology.2022; 2022: 1. CrossRef - The longitudinal loss of islet autoantibody responses from diagnosis of type 1 diabetes occurs progressively over follow-up and is determined by low autoantibody titres, early-onset, and genetic variants
C L Williams, R Fareed, G L M Mortimer, R J Aitken, I V Wilson, G George, K M Gillespie, A J K Williams, Chitrabhanu Ballav, Atanu Dutta, Michelle Russell-Taylor, Rachel Besser, James Bursell, Shanthi Chandran, Sejal Patel, Anne Smith, Manohara Kenchaiah,
Clinical and Experimental Immunology.2022; 210(2): 151. CrossRef
- Relationship between β-Cell Autoantibodies and Their Combination with Anthropometric and Metabolic Components and Microvascular Complications in Latent Autoimmune Diabetes in Adults
- Technology/Device
- Glutamic Acid Decarboxylase Autoantibody Detection by Electrochemiluminescence Assay Identifies Latent Autoimmune Diabetes in Adults with Poor Islet Function
- Yuxiao Zhu, Li Qian, Qing Liu, Jing Zou, Ying Zhou, Tao Yang, Gan Huang, Zhiguang Zhou, Yu Liu
- Diabetes Metab J. 2020;44(2):260-266. Published online November 12, 2019
- DOI: https://doi.org/10.4093/dmj.2019.0007
- 5,345 View
- 128 Download
- 11 Web of Science
- 13 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background The detection of glutamic acid decarboxylase 65 (GAD65) autoantibodies is essential for the prediction and diagnosis of latent autoimmune diabetes in adults (LADA). The aim of the current study was to compare a newly developed electrochemiluminescence (ECL)-GAD65 antibody assay with the established radiobinding assay, and to explore whether the new assay could be used to define LADA more precisely.
Methods Serum samples were harvested from 141 patients with LADA, 95 with type 1 diabetes mellitus, and 99 with type 2 diabetes mellitus, and tested for GAD65 autoantibodies using both the radiobinding assay and ECL assay. A glutamic acid decarboxylase antibodies (GADA) competition assay was also performed to assess antibody affinity. Furthermore, the clinical features of these patients were compared.
Results Eighty-eight out of 141 serum samples (62.4%) from LADA patients were GAD65 antibody-positive by ECL assay. Compared with ECL-GAD65 antibody-negative patients, ECL-GAD65 antibody-positive patients were leaner (
P <0.0001), had poorer β-cell function (P <0.05), and were more likely to have other diabetes-associated autoantibodies. The β-cell function of ECL-GAD65 antibody-positive patients was similar to that of type 1 diabetes mellitus patients, whereas ECL-GAD65 antibody-negative patients were more similar to type 2 diabetes mellitus patients.Conclusion Patients with ECL-GAD65 antibody-negative share a similar phenotype with type 2 diabetes mellitus patients, whereas patients with ECL-GAD65 antibody-positive resemble those with type 1 diabetes mellitus. Thus, the detection of GADA using ECL may help to identify the subtype of LADA.
-
Citations
Citations to this article as recorded by- 2. Diagnosis and Classification of Diabetes: Standards of Care in Diabetes—2024
Nuha A. ElSayed, Grazia Aleppo, Raveendhara R. Bannuru, Dennis Bruemmer, Billy S. Collins, Laya Ekhlaspour, Jason L. Gaglia, Marisa E. Hilliard, Eric L. Johnson, Kamlesh Khunti, Ildiko Lingvay, Glenn Matfin, Rozalina G. McCoy, Mary Lou Perry, Scott J. Pil
Diabetes Care.2024; 47(Supplement): S20. CrossRef - 2. Classification and Diagnosis of Diabetes: Standards of Care in Diabetes—2023
Nuha A. ElSayed, Grazia Aleppo, Vanita R. Aroda, Raveendhara R. Bannuru, Florence M. Brown, Dennis Bruemmer, Billy S. Collins, Jason L. Gaglia, Marisa E. Hilliard, Diana Isaacs, Eric L. Johnson, Scott Kahan, Kamlesh Khunti, Jose Leon, Sarah K. Lyons, Mary
Diabetes Care.2023; 46(Supplement): S19. CrossRef - Determination of autoantibodies in type 2 diabetes: one simple way to improve classification
Johnny Ludvigsson
Diabetologia.2023; 66(5): 955. CrossRef - 2. Classification and Diagnosis of Diabetes:Standards of Medical Care in Diabetes—2022
Diabetes Care.2022; 45(Supplement): S17. CrossRef - Screening Strategy for Islet Autoantibodies in Diabetes Patients of Different Ages
Xixi Nan, Xia Li, Yufei Xiang, Xiang Yan, Houde Zhou, Xiaohan Tang, Jin Cheng, Xiaohong Niu, Jing Liu, Qiuhe Ji, Linong Ji, Gan Huang, Zhiguang Zhou
Diabetes Technology & Therapeutics.2022; 24(3): 212. CrossRef - Atypical Diabetes and Management Considerations
Shivajirao Prakash Patil
Primary Care: Clinics in Office Practice.2022; 49(2): 225. CrossRef - Latent autoimmune diabetes in adults: a focus on β-cell protection and therapy
Wenfeng Yin, Shuoming Luo, Zilin Xiao, Ziwei Zhang, Bingwen Liu, Zhiguang Zhou
Frontiers in Endocrinology.2022;[Epub] CrossRef - Analysis of detrended fluctuation function derived from continuous glucose monitoring may assist in distinguishing latent autoimmune diabetes in adults from T2DM
Liyin Zhang, Qi Tian, Keyu Guo, Jieru Wu, Jianan Ye, Zhiyi Ding, Qin Zhou, Gan Huang, Xia Li, Zhiguang Zhou, Lin Yang
Frontiers in Endocrinology.2022;[Epub] CrossRef - Prevalence of antibodies targeting ubiquitin-conjugating enzyme 2L3 and eukaryote translation elongation factor 1 α1 in Chinese Han and American Caucasian populations with type 1 diabetes
Li Qian, Yuxiao Zhu, Yan Luo, Mu Zhang, Liping Yu, Yu Liu, Tao Yang
Endocrine Connections.2022;[Epub] CrossRef - 2. Classification and Diagnosis of Diabetes:Standards of Medical Care in Diabetes—2021
Diabetes Care.2021; 44(Supplement): S15. CrossRef - High-Affinity ZnT8 Autoantibodies by Electrochemiluminescence Assay Improve Risk Prediction for Type 1 Diabetes
Xiaofan Jia, Ling He, Dongmei Miao, Kathleen Waugh, Cristy Geno Rasmussen, Fran Dong, Andrea K Steck, Marian Rewers, Liping Yu
The Journal of Clinical Endocrinology & Metabolism.2021;[Epub] CrossRef - Lada or Type 2 Diabetes Mellitus - A Challenging Diagnosis in Clinical Approach
Lucia Mihaela Custură, Oana Deteşan, Raluca Maria Tilinca, Reka Annamaria Schmiedt, Brigitta Irén Bacso, Mariana Cornelia Tilinca
Acta Medica Transilvanica.2021; 26(3): 55. CrossRef - A fluorescence enhancement assay for measurement of glutamate decarboxylase activity
Messripour Manoochehr, Mesripour Azadeh
Open Journal of Analytical and Bioanalytical Chemistry.2020; : 007. CrossRef
- 2. Diagnosis and Classification of Diabetes: Standards of Care in Diabetes—2024
- Prevalence and Clinical Characteristics of Recently Diagnosed Type 2 Diabetes Patients with Positive Anti-Glutamic Acid Decarboxylase Antibody
- Yul Hwangbo, Jin Taek Kim, Eun Ky Kim, Ah Reum Khang, Tae Jung Oh, Hak Chul Jang, Kyong Soo Park, Seong Yeon Kim, Hong Kyu Lee, Young Min Cho
- Diabetes Metab J. 2012;36(2):136-143. Published online April 17, 2012
- DOI: https://doi.org/10.4093/dmj.2012.36.2.136
- 4,576 View
- 40 Download
- 15 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background Latent autoimmune diabetes in adults (LADA) refers to a specific type of diabetes characterized by adult onset, presence of islet auto-antibodies, insulin independence at the time of diagnosis, and rapid decline in β-cell function. The prevalence of LADA among patients with type 2 diabetes varies from 2% to 20% according to the study population. Since most studies on the prevalence of LADA performed in Korea were conducted in patients who had been tested for anti-glutamic acid decarboxylase antibody (GADAb), a selection bias could not be excluded. In this study, we examined the prevalence and clinical characteristics of LADA among adult patients recently diagnosed with type 2 diabetes.
Methods We included 462 patients who were diagnosed with type 2 diabetes within 5 years from the time this study was performed. We measured GADAb, fasting insulin level, fasting C-peptide level, fasting plasma glucose level, HbA1c, and serum lipid profiles and collected data on clinical characteristics.
Results The prevalence of LADA was 4.3% (20/462) among adult patients with newly diagnosed type 2 diabetes. Compared with the GADAb-negative patients, the GADAb-positive patients had lower fasting C-peptide levels (1.2±0.8 ng/mL vs. 2.0±1.2 ng/mL,
P =0.004). Other metabolic features were not significantly different between the two groups.Conclusion The prevalence of LADA is 4.3% among Korean adult patients with recently diagnosed type 2 diabetes. The Korean LADA patients exhibited decreased insulin secretory capacity as reflected by lower C-peptide levels.
-
Citations
Citations to this article as recorded by- The worldwide prevalence of latent autoimmune diabetes of adults among adult-onset diabetic individuals: a systematic review and meta-analysis
Deepika Ramu, Selvaraj Ramaswamy, Suresh Rao, Solomon F. D. Paul
Endocrine.2023; 82(1): 28. CrossRef - Investigation of serum level relationship anti-glutamic acid decarboxylase antibody and inflammatory cytokines (IL1-β, IL-6) with vitamins D in type 2 diabetes
Vahid Pouresmaeil, Sarmad Mashayekhi, Mohammad Sarafraz Yazdi
Journal of Diabetes & Metabolic Disorders.2022; 21(1): 181. CrossRef - Recent information on test utilization and intraindividual change in anti-glutamic acid decarboxylase antibody in Korea: a retrospective study
Rihwa Choi, Wonseo Park, Gayoung Chun, Jiwon Lee, Sang Gon Lee, Eun Hee Lee
BMJ Open Diabetes Research & Care.2022; 10(3): e002739. CrossRef - Prevalence and factors associated with latent autoimmune diabetes in adults (LADA): a cross-sectional study
Anselmo M. Manisha, Aminiel R. Shangali, Sayoki G. Mfinanga, Erasto V. Mbugi
BMC Endocrine Disorders.2022;[Epub] CrossRef - Latent Autoimmune Diabetes in Adults (LADA) and its Metabolic Characteristics among Yemeni Type 2 Diabetes Mellitus Patients
Dhekra Al-Zubairi, Molham AL-Habori, Riyadh Saif-Ali
Diabetes, Metabolic Syndrome and Obesity: Targets and Therapy.2021; Volume 14: 4223. CrossRef - Therapeutic approaches for latent autoimmune diabetes in adults: One size does not fit all
Theocharis Koufakis, Niki Katsiki, Pantelis Zebekakis, George Dimitriadis, Kalliopi Kotsa
Journal of Diabetes.2020; 12(2): 110. CrossRef - Long‐term effects on glycaemic control and β‐cell preservation of early intensive treatment in patients with newly diagnosed type 2 diabetes: A multicentre randomized trial
Suk Chon, Sang Youl Rhee, Kyu Jeung Ahn, Sei Hyun Baik, Yongsoo Park, Moon Suk Nam, Kwan Woo Lee, Soon Jib Yoo, Gwanpyo Koh, Dae Ho Lee, Young Seol Kim, Jeong‐Taek Woo
Diabetes, Obesity and Metabolism.2018; 20(5): 1121. CrossRef - A Global Perspective of Latent Autoimmune Diabetes in Adults
Rajashree Mishra, Kenyaita M. Hodge, Diana L. Cousminer, Richard D. Leslie, Struan F.A. Grant
Trends in Endocrinology & Metabolism.2018; 29(9): 638. CrossRef - The prevalence of latent autoimmune diabetes in adults and its correlates in patients with type 2 diabetes in Kerman, Iran [2011]
Gozashti Mohammad Hossein, Shafiei Maryam, Esmaeilian Saeed, Najafipour Hamid, Mashrouteh Mahdieh
Diabetes & Metabolic Syndrome: Clinical Research & Reviews.2015; 9(2): 104. CrossRef - Low prevalence of latent autoimmune diabetes in adults in northern India
A. Sachan, G. Zaidi, R. P. Sahu, S. Agrawal, P. G. Colman, E. Bhatia
Diabetic Medicine.2015; 32(6): 810. CrossRef - Amelioration of Diabetes-induced Cognitive Deficits by GSK-3β Inhibition is Attributed to Modulation of Neurotransmitters and Neuroinflammation
Ashok Kumar Datusalia, Shyam Sunder Sharma
Molecular Neurobiology.2014; 50(2): 390. CrossRef - Successful treatment of latent autoimmune diabetes in adults with Traditional Chinese Medicine: a case report
Jiaxing Tian, Wenke Liu, Zhong Zhen, Xiaolin Tong
Journal of Traditional Chinese Medicine.2013; 33(6): 766. CrossRef - Clinical characteristics and insulin independence of Koreans with new‐onset type 2 diabetes presenting with diabetic ketoacidosis
H. Seok, C. H. Jung, S. W. Kim, M. J. Lee, W. J. Lee, J. H. Kim, B‐W. Lee
Diabetes/Metabolism Research and Reviews.2013; 29(6): 507. CrossRef - A Case of Latent Autoimmune Diabetes in Adults Developed after Surgical Cure of Growth Hormone Secreting Pituitary Tumor
Wonjin Kim, Jung Ho Kim, Youngsook Kim, Ji Hye Huh, Su Jin Lee, Mi Sung Park, Eun Yeong Choe, Jeong Kyung Park, Myung Won Lee, Jae Won Hong, Byung Wan Lee, Eun Seok Kang, Bong Soo Cha, Eun Jig Lee, Hyun Chul Lee
Endocrinology and Metabolism.2012; 27(4): 318. CrossRef - Latent Autoimmune Diabetes in Adults: Autoimmune Diabetes in Adults with Slowly Progressive β-cell Failure
Hannah Seok, Byung Wan Lee
Diabetes & Metabolism Journal.2012; 36(2): 116. CrossRef
- The worldwide prevalence of latent autoimmune diabetes of adults among adult-onset diabetic individuals: a systematic review and meta-analysis
- Chronic Complications in Adult Diabetic Patients with and without GAD Antibody.
- Jin Ook Chung, Dong Hyeok Cho, Dong Jin Chung, Min Young Chung
- Korean Diabetes J. 2009;33(2):124-133. Published online April 1, 2009
- DOI: https://doi.org/10.4093/kdj.2009.33.2.124
- 2,093 View
- 18 Download
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Although the majority of diabetes mellitus (DM) patients diagnosed as adults have non-autoimmune forms of the disease, islet autoimmunity is encountered in some patients initially thought to have type 2 DM. The phenotype of DM patients with glutamic acid decarboxylase (GAD) antibodies is different from that of patients with GAD antibody-negative type 2 DM, with features such as relative leanness and hyperglycemia which may influence the development of complications. We sought to compare the prevalence of chronic complications in patients with and without the GAD antibody. METHODS: We recruited 427 patients (M: 218, F: 209) that were clinically diagnosed with type 2 DM after the age of 35 years. We measured GAD antibody and assessed the factors associated with chronic microvascular and macrovascular complications. RESULTS: Of these patients, 26 were GAD antibody-positive. The patients with GAD antibody had lower systolic blood pressure, higher high-density lipoprotein cholesterol value, and lower level of fasting and stimulated C-peptide than patients without GAD antibody (P < 0.05). Also, the patients with GAD antibody had lower prevalence of retinopathy compared with the patients without GAD antibody (19.2 vs. 47.9%; P < 0.05). The prevalence of nephropathy, peripheral neuropathy and cardiovascular autonomic neuropathy did not differ between the groups. In addition, the prevalence of coronary heart disease, cerebrovascular disease and peripheral arterial disease did not differ between the two groups. CONCLUSION: This study suggests that diabetic patients with GAD antibody have a lower risk for the development of retinopathy compared with patients without GAD antibody. -
Citations
Citations to this article as recorded by- Relationship between β-Cell Autoantibodies and Their Combination with Anthropometric and Metabolic Components and Microvascular Complications in Latent Autoimmune Diabetes in Adults
Tomislav Bulum, Marijana Vučić Lovrenčić, Jadranka Knežević Ćuća, Martina Tomić, Sandra Vučković-Rebrina, Lea Duvnjak
Biomedicines.2023; 11(9): 2561. CrossRef
- Relationship between β-Cell Autoantibodies and Their Combination with Anthropometric and Metabolic Components and Microvascular Complications in Latent Autoimmune Diabetes in Adults

 KDA
KDA
 First
First Prev
Prev





