Nonalcoholic Fatty Liver Disease in Diabetes. Part I: Epidemiology and Diagnosis
Article information
Abstract
Nonalcoholic fatty liver disease (NAFLD) and diabetes are common metabolic disorders whose prevalence rates are expected to rise worldwide, corresponding to aging and increasingly obese populations. Compared to the general population (around 25%), 50% to 70% of people with diabetes have NAFLD, and NAFLD severity (including fibrosis) tends to be worsened by the presence of diabetes. NAFLD is considered an emerging risk factor for type 2 diabetes mellitus and a contributor to the development of chronic diabetes-related complications. This reciprocal relationship demonstrates the importance of confirming suspected NAFLD in patients with diabetes. Due to the invasive nature of liver biopsy to assess NAFLD status, various alternative non-invasive modalities have been developed and validated. Here, we summarized the epidemiology of NAFLD in patients with diabetes and reviewed currently available imaging modalities and biomarker-based prediction models for their ability to detect liver steatosis and/or fibrosis.
INTRODUCTION
The prevalence of diabetes is rising. According to Diabetes Atlas 2017, 425 million people suffer from diabetes worldwide; the prevalence rate in Korea is 14.4% according to the Diabetes Fact Sheet 2018 [1 2]. Type 2 diabetes mellitus (T2DM) is caused by derangements in multiple organs and by various pathophysiological abnormalities, such that it is implicated in many other diseases related to insulin resistance and obesity, such as nonalcoholic fatty liver disease (NAFLD), sleep apnea, arthritis, cardiovascular disease (CVD), and metabolic syndrome (MetS) [3 4].
NAFLD is considered the hepatic manifestation of ectopic fat accumulation caused by abdominal obesity and insulin resistance; its presence also reflects visceral, intramuscular, epicardial, and perivascular fat accumulation. Recent evidence suggests that NAFLD should be considered a cardiovascular risk factor [4]. NAFLD is a strong clinical signal for insulin resistance and MetS, and is considered a confirmative risk factor for T2DM [2]. Prevalence of NAFLD in patients with T2DM is much higher than in the general population. This review summarizes the epidemiology of NAFLD relative to T2DM, and compares various approaches to diagnose and assess NAFLD characteristics, including steatohepatitis and fibrosis.
PREVALENCE OF NAFLD IN THE GENERAL POPULATION
The current prevalence of NAFLD is proportional to increased rates of obesity. NAFLD incidence in the general population is about 25%, but it rises to more than 90% for very obese individuals undergoing weight reduction procedures/surgeries [5]. In addition, like obesity, NAFLD displays different characteristics among various ethnic groups and across countries [6].
In the general Korean population, some discrepancies exist in NAFLD prevalence. In a study by Park et al. [7] in which 4,967 young, healthy Koreans participated in a health screening program, the age-adjusted NAFLD prevalence rate was 21.6% (men), 11.2% (women), and 16.1% in the whole population. According to Jeong et al. [8], in a cross-sectional study of 140,000 participants in a health screening program, the NAFLD prevalence rate was 25.2%, with some differences based on where participants lived.
PREVALENCE OF NAFLD IN PATIENTS WITH T2DM
NAFLD prevalence in patients with T2DM is much higher than in the general population. In a systemic review by Lonardo et al. [9], the NAFLD incidence rate in patients with T2DM is 50% to 75%, according to ethnicity, across studies. In reverse, the prevalence of diabetes in patients with NAFLD is higher than in the general population. In a study by Browning et al. [10] of 2,287 urban people participating in the Dallas Heart Study, hepatic triglyceride content was measured by 1H-nuclear magnetic resonance spectroscopy (MRS), with prevalence of T2DM or impaired fasting glucose (IFG) reported as 18% to 33% in patients with NAFLD.
There is discrepancy between the studies regarding prevalence of NAFLD in patients with T2DM, which may be accounted for by the diagnostic tools used [11]. The prevalence of NAFLD was 20.3% when plasma alanine aminotransferase was used to define NAFLD, whereas the prevalence reached 72.8% when MRS was used to define NAFLD. In addition, NAFLD prevalence in patients with T2DM significantly increased with increasing obesity [11].
NAFLD prevalence in Asians is never lower than in Caucasians. In 929 Korean patients with T2DM who visited a university-based diabetes clinic, NAFLD was assessed by ultrasonogram [12], and 63.3% of patients had NAFLD. In 8,352 Japanese patients who received health check-ups from 2009 to 2010, NAFLD incidence was 25.6% in those with normal fasting glucose, 56.2% in those with IFG, and 68% in those with T2DM defined as fasting blood glucose ≥126 mg/dL, suggesting NAFLD prevalence could differ by glycemic status [13].
NAFLD AS A RISK FACTOR FOR T2DM
There is convincing evidence that NAFLD often precedes the development of T2DM [14]. Some suggest that the conventional paradigm of NAFLD to represent ‘hepatic manifestation’ of MetS is outdated, as recently NALFD has been shown to be an early predictor and determinant for development of diabetes.
By examining the pathophysiological aspects of insulin resistance in NAFLD development, we can understand the intimate relationship between these conditions. NAFLD is associated with hepatic and peripheral insulin resistance, causing insufficient suppression of hepatic gluconeogenesis, decreased glycogen synthesis, and increased lipid accumulation [3]. The influx of high amounts of free fatty acid (FFA) from white adipose and dietary lipids into the liver promotes further glucose synthesis. De novo synthesis of FFA is driven by sterol regulatory element binding-protein 1c (Srebp-1c) and carbohydrate response element binding-protein (ChREBP), catalyzed by hyperinsulinemia and hyperglycemia. Further factors such as decreased lipid export through very-low density lipoprotein, increased hepatic insulin resistance via diacylglycerol, and increased oxidative stress mediated due to exhaustion of antioxidant capacities of superoxide dismutase and glutamate peroxidase, ultimately result in development of NAFLD and progression to nonalcoholic steatohepatitis (NASH) in insulin resistant patients.
Meta-analyses have shown a 1.6- to 6.8-fold increased risk for diabetes in subjects with NAFLD according to established diagnostic methods, definitions, and the risk factors included for adjustment in the model [4 15]. In 5,372 non-diabetic Koreans in whom health screening was performed repeatedly in 5 years; interval, after adjustment for confounding factors, relative risk for T2DM was 1.97 in all participants and 2.29 after excluding frequent drinkers [16]. In another study analyzed in nondiabetic 11,091 Koreans in whom health screening was performed repeatedly in 5 years; interval, the odds ratio for T2DM was 2.05 after adjustment for confounding factors, and this risk was highest in those with the highest baseline insulin levels [17].
Although NAFLD is a definite risk factor for T2DM, risk could be attenuated if NAFLD is resolved. In 13,218 nondiabetic Korean participants in a health promotion center, incident diabetes was assessed at 5 years [18] by dividing them into six groups according to hepatic steatosis status at baseline and 5 years later. Using “no steatosis at baseline or follow-up” as the reference group, steatosis at baseline and follow-up showed a 2.78-fold increased risk for T2DM, and worsening severity of steatosis at follow-up showed a 7.38-fold increased risk. However, steatosis at baseline but not at follow-up showed no increased risk for T2DM compared to the reference group, suggesting that resolution of steatosis attenuated T2DM risk. Similar results were observed in another study of 4,604 Japanese participants at 10 years of follow-up [19]. In a study by Bae et al. [20], NAFLD status was assessed in 7,849 non-diabetic subjects over 5 years. Those with NAFLD for 5 consecutive years showed a 1.55-fold increased risk for T2DM compared with those who never had NAFLD, and participants with intermittent NAFLD showed no increased risk for T2DM, suggesting that persistent NAFLD presence affects risk for T2DM more strongly.
While it is evident that NAFLD is a significant risk factor for T2DM, certain conditions promote that risk. In a retrospective study of 12,853 non-diabetic Korean participants, those with any of insulin resistance, overweight/obesity, and steatosis independently doubled the risk of T2DM [21]. However, when these three conditions co-occurred, risk increased 14-fold, suggesting their combined influence on T2DM risk. In a study by Bae et al. [22], participants with IFG and NAFLD showed a 9-fold increased risk for T2DM at 5 years compared with the group without IFG and NAFLD. In addition, there was an additive effect of NAFLD on development of T2DM in individuals with MetS, and the risk for T2DM increased when elevated liver enzymes or increased fibrosis scores were accompanied by NAFLD [23 24 25].
It is apparent that NAFLD is an established risk factor for T2DM. Further, NAFLD resolution attenuates T2DM risk, but when obesity, insulin resistance, or hyperglycemia is combined with NAFLD, T2DM risk significantly increases.
T2DM AS A RISK FACTOR FOR NASH AND FIBROSIS
While presence of NAFLD may not predict any clinical abnormalities other than T2DM, progression of NAFLD to NASH or fibrosis, and further development of cirrhosis, is a serious problem. A 10% to 35% of those with normal liver histology progresses to steatosis and 12% to 40% of those with hepatic steatosis progress to steatohepatitis, and up to 15% of patients with NASH are known to progress to cirrhosis [26].
The factors that affect progression of NAFLD to NASH are unknown. One study reports on 129 biopsy-proven subjects with NAFLD that were followed for 13.7 years [27]. Although baseline glycemic status was unknown, 78% of participants at follow-up had diabetes, and insulin resistance was more prominent in those with progressive versus nonprogressive fibrosis, suggesting dysglycemia as a factor for progression to fibrosis. In 1,918 Hong Kong patients with diabetes in whom fibroscan was performed, 17.7% showed significant liver stiffness [28]. In a Rotterdam study of 3,041 participants, those with baseline diabetes and NAFLD showed a significantly higher probability of liver stiffness compared as those without diabetes or NAFLD, and age, diabetes and NAFLD were the factors that aggravated liver stiffness [28 29]. In 108 patients who had two liver biopsies in a median interval of 6.6 years, there was a significantly higher proportion of patients with T2DM among those who progressed to fibrosis compared with those who did not [30]. In one study of biopsy-proven NAFLD patients, the proportion of those with diabetes significantly increased as fibrosis stage worsened from 0 to 4 [31]; and in another study, diabetes was the significant predictor for fibrosis in patients with biopsy-proven NAFLD [32].
Based on these results, Tilg et al. [3] recently suggested a clinical algorithm to screen and manage NAFLD by which patients with NAFLD should be screened for MetS and T2DM and, as patients with T2DM are at very high risk for NAFLD, screening for NAFLD should be performed irrespective of serum liver enzyme levels and elastography should be considered in these patients to detect liver stiffness.
NAFLD AS AN AGGRAVATING FACTOR FOR DIABETIC COMPLICATIONS
There is evidence that presence of NAFLD in patients with T2DM aggravates diabetic complications [33]. In 2,839 T2DM patients, those with NAFLD showed a significantly higher prevalence of CVD [34]. The risk for macrovascular complications remained significantly increased after adjustment for multiple risk factors. In 2,103 patients with T2DM and NAFLD ascertained by history and ultrasonogram, the risk for proliferative retinopathy and chronic kidney disease, respectively, were 1.75- and 1.87-fold increased compared with those who did not have NAFLD, suggesting risk for microvascular as well as macrovascular complications is significantly associated with NAFLD in T2DM [35].
Other study results suggest increased mortality in patients with T2DM and NAFLD. In 337 patients with diabetes followed for 10.9 years, more liver-related deaths occurred in those with versus without NAFLD [36]. In addition, in a multivariate model, NAFLD significantly predicted death in patients with T2DM after adjustment for confounding factors.
Increased risk for diabetic complications in the presence of NAFLD was similarly observed in patients with type 1 diabetes mellitus (T1DM). In 250 T1DM patients, NAFLD prevalence was 44.4%, and the prevalence of CVD and microvascular disease was significantly higher in those with versus without NAFLD [37 38]. These results suggest a deleterious effect of NAFLD on vasculature, which is commonly seen in patients with T1DM and T2DM.
DIAGNOSIS OF NAFLD
In individuals with and without diabetes, a two-step process should be used to diagnose NAFLD: (1) existence of hepatic steatosis, either by imaging or histology; and (2) exclusion of secondary causes of liver steatosis as described in Table 1 [39 40]. Other endocrinologic disorders such as hypothyroidism, hypopituitarism, and hypogonadism are also associated with NAFLD; therefore, related laboratory assessments should be considered for patients with signs or symptoms of these endocrinopathies.
NAFLD spans the spectrum of fatty liver conditions, from simple steatosis (nonalcoholic fatty liver [NAFL]) and steatohepatitis (NASH) to advanced fibrosis or cirrhosis. By histologic liver biopsy, NAFL is defined as ≥5% hepatic steatosis with no evidence of hepatocellular injury (hepatocyte ballooning). NASH is a combination of NAFL and inflammation with hepatocyte injury (e.g., ballooning), with or without fibrosis.
IMAGING MODALITIES TO ASSESS HEPATIC STEATOSIS
Despite its invasive nature and sampling variability [41], liver biopsy remains the gold standard to assess hepatic steatosis, inflammation, and fibrosis in patients with NAFLD. It should be considered for patients suspected to have advanced fibrosis or when exclusion of other chronic liver diseases is needed. To overcome its high costs and risks, alternative noninvasive imaging, clinical, and laboratory modalities have been developed and validated to diagnose NAFLD.
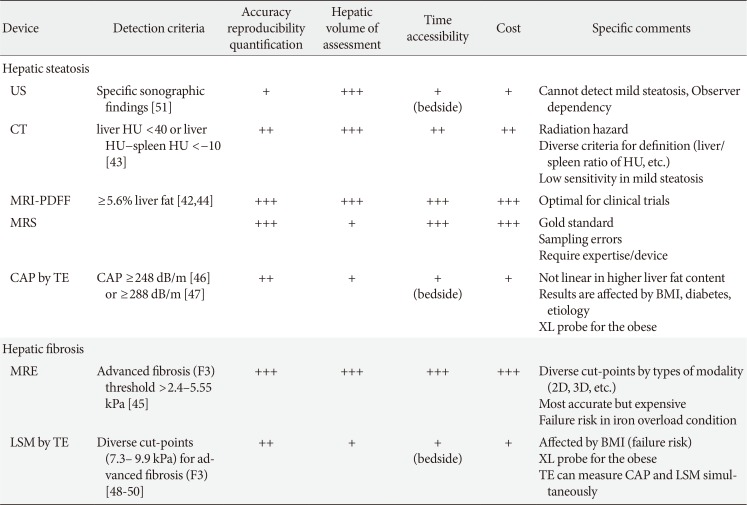
Currently, ultrasonography (US), computed tomography (CT), magnetic resonance imaging (MRI), MRS, and transient elastography (TE) are widely available tools to measure hepatic steatosis (Table 2) [42 43 44 45 46 47 48 49 50 51].
Ultrasonography
US is the recommended first line screening method for patients with T2DM by the European NAFLD guidelines [42]. Although US has interobserver variability and limited sensitivity to detect mild (<20%) steatosis [52] or morbid obesity (body mass index [BMI] >40 kg/m2) [53], it can provide additional information about liver structure. In a meta-analysis, US achieved pooled sensitivity of 84.8% and pooled specificity of 93.6% to detect ≥20% to 30% steatosis, compared with histology [52]. However, US is limited in accuracy and reproducibility as echogenicity, an essential sonographic feature to assess degree of fat content, can be affected by various patient (obesity, coexistent kidney disease) and acquisition (device, operator, instrument settings) factors.
Computed tomography
CT scanners are standardized to obtain pixel value measurements relative to water using a dimensionless unit known as the Hounsfield unit (HU). Radiodensity of water is 0 HU by definition and air is defined as −1,000 HU [54]. In non-contrast CT, normal liver parenchyma and fat are about 50 to 60 and −20 to −100 HU, respectively. Due to inconsistency in HU calibration by external factors, ‘fat-free spleen’ can be used as an internal reference [55]. Although various criteria to define steatosis have been proposed, hepatic HU less than 40 or (liver HU-spleen HU) less than −10 can detect steatosis [43] with sensitivity and specificity ranging from 46% to 72% and 88% to 95%, respectively [56]. Similar to US, CT has limited sensitivity to detect mild steatosis (<30% liver fat). Radiation exposure is an additional drawback. Although CT can quantitatively measure hepatic steatosis, it is an unfavorable modality to diagnose fatty liver in the clinical setting. A few clinical trials of patients with T2DM applied CT scan to monitor changes in hepatic steatosis [57 58].
Magnetic resonance imaging
To date, MRI showed the most powerful performance for assessing steatosis. MRI-based methods are generally divided into two classes: MRS and MRI-proton density fat fraction (MRI-PDFF). MRS is considered the gold standard for quantification of hepatic triglyceride (fat) content [42 44], as it is sensitive enough to detect trace amounts of liver fat. MRS is more a biochemical-based technique than imaging. It quantifies the signal intensity of proton at frequencies corresponding to water or fat within the voxel-of-interest, and the fat signal fraction is calculated. In a recent meta-analysis with histology as the reference, MRS showed high diagnostic accuracy to detect mild steatosis (histological grade ≥5%) with sensitivity and specificity of 89% and 84%, respectively [59]. However, major limitations of MRS are: high cost; time consumption; need for specialized expertise and devices; and small volume of measurements (usually <3×3×3 cm in size), which may cause sampling errors.
Several MRI-based methods have been developed for measuring liver fat content. MRI-PDFF is a fundamental tissue trait and can be calculated as the (proton signal from magnetic resonance [MR]-visible triglyceride)/(total proton signal including triglyceride and water) [54 60]. Therefore, internal calibration or a reference standard is not needed. The diagnostic accuracy of MRI-PDFF to detect steatosis is comparable to MRS or liver biopsy [45 54 61], while it also allows whole imaging of the liver where fat is measured. This can minimize sampling error, making MRI-PDFF useful for monitoring patients sequentially, such as in NAFLD clinical trials [45 62 63].
Transient elastography
Controlled attenuation parameter (CAP) is a simple quantitative index based on the properties of ultrasonic signals examined by transient liver elastography (Fibroscan; Echosens, Paris, France). Based on the concept that fat attenuates US propagation, it quantifies US attenuation at the center frequency of the Fibroscan M probe (3.5 MHz) or XL probe (2.5 MHz) within approximately 3 cm3 of liver volume [64]. Recent meta-analysis with CAP measurements in patients with various chronic liver diseases including NAFLD (20% of the total population), demonstrated its diagnostic accuracy to detect hepatic steatosis with sensitivity and specificity of 69% and 82%, respectively (area under the receiver operating characteristic curve [AUROC]=0.823) [46]. Optimal cut-off values for defining S1, S2, and S3 were 248, 268, and 280 dB/m, respectively. The authors proposed that individual CAP values should be interpreted after adjustment for presence of diabetes, steatosis etiology (NAFLD), and BMI, as these factors can overrate CAP values [46]. Wong et al. [65] recently established validity criteria for CAP measurement by M probe in clinical practice. Interquartile range (IQR), which can be derived from 10 repeated values of CAP, reflects the fluctuation of CAP measurements. If IQR >40 dB/m, accuracy of CAP to diagnose steatosis substantially declines. Caussy et al. [47] proposed a cut-off value of 288 dB/m for CAP measurement of hepatic steatosis (defined as MRI-PDFF ≥5%), with improved diagnostic accuracy when the IQR was <30 dB/m. The discrepancy in CAP cut-points in the two previous studies may be due to differences in obesity prevalence, NAFLD, and diabetes. To reduce the failure rate of CAP measurements in obese (BMI ≥30 kg/m2) patients, XL probe is recommended [66 67]. In biopsy-proven NAFLD patients, MRI-PDFF was more accurate than CAP in diagnosing all grades of steatosis [48 68]. Notably, CAP showed a non-linear relationship with liver fat content in patients with severe fatty liver, indicating a limitation to discriminate moderate and severe steatosis (grade 2 vs. 3). Lee et al. [69] recently conducted an efficacy study of NAFLD using CAP as a primary endpoint in T2DM patients, to assess its utility in clinical trials.
Compared to MRI-PDFF, TE-based CAP showed relatively lower accuracy to detect steatosis whereas its advantages include cost and accessibility. More research on these modalities, to evaluate and define their distinct roles, are warranted [70].
IMAGING MODALITIES TO ASSESS NASH AND HEPATIC FIBROSIS
To date, no imaging technique can reliably diagnose NASH. In contrast, liver fibrosis can be indirectly quantified by measuring liver stiffness using imaging modalities such as magnetic resonance elastography (MRE) and TE, because fibrotic liver contains a high level of collagen resulting in tissue rigidity.
Magnetic resonance elastography
MRE uses vibration to generate low frequency mechanical waves in liver tissue, visualize the propagating waves using a phase contrast MRI technique, and then transform the wave information into quantitative images reflecting liver stiffness [71]. Contrary to the European NAFLD guidelines, United States guidelines state that MRE is useful to identify advanced fibrosis in patients with NAFLD [40] due to its better performance in discriminating stage 1 and ≥2 fibrosis compared to TE [68]; furthermore, MRE's superiority to detect fibrosis was confirmed in a meta-analysis [49]. Although it is reliable, reproducible, and the most accurate method for estimating hepatic fibrosis, MRE is expensive, not widely available in many clinics, and requires specialized expertise to obtain acceptable images.
Transient elastography
TE (Fibroscan) is a point-of-care imaging technique using US in which propagation velocity directly reflects tissue elasticity to 1 cm wide and 4 cm long [72]. This can quickly generate a surrogate marker of liver fibrosis stage called liver stiffness measurement (LSM). Results are described as the median values of 10 validated measurements, ranging from 2.5 to 75.0 kilopascals (kPa), with healthy liver values <5.5 kPa [73]. Importantly, validity criteria of LSM by TE include a success rate (ratio of valid measurements to total measurements) >60% and an IQR/median LSM ratio of <0.3 [74]. TE has been intensively studied in patients with viral hepatitis; however, its diagnostic accuracy for hepatic fibrosis was recently validated in NAFLD patients [50 75]. Notably, LSM was more correlated with fibrosis stage in individuals with severe fibrosis (F3) and cirrhosis (F4) [75 76]. TE has higher negative predictive values for excluding advanced fibrosis than positive predictive values for detection [75], indicating that additional surrogate markers for fibrosis can enhance the ability to diagnose advanced fibrosis or cirrhosis. A major weakness of TE is a high failure risk in obese patients [77] and low accuracy to detect fibrosis in high BMI patients [75]. As T2DM patients tend to be obese, this issue should be carefully considered before utilizing TE. In such cases, XL-probe may provide more reliable results for morbidly obese patients [78]. Due to its accessibility, low cost, and moderate accuracy, TE is recommended by both United States and European NAFLD guidelines as an acceptable non-invasive method to identify patients at low risk of advanced fibrosis/cirrhosis [40 42].
BIOMARKER-BASED PREDICTION MODELS TO ASSESS STEATOSIS, NASH, AND HEPATIC FIBROSIS
Besides imaging modalities, several noninvasive biomarker models have been developed to predict NASH and fibrosis. As NAFLD patients with diabetes are at high risk for NASH and fibrosis, which are significantly associated with morbidity and mortality, evaluation of these conditions is essential for clinical management [42]. Models incorporating both clinical and laboratory parameters, which are directly or indirectly linked to liver status, provide enhanced diagnostic accuracy to identify high risk individuals [79].
Hepatic steatosis
Many noninvasive prediction models have been proposed to detect hepatic steatosis in NAFLD cohorts (Table 3) [80 81 82 83 84 85 86 87]. The majority of models are derived from datasets with fatty liver defined by US. European NAFLD guidelines state that fatty liver index (FLI), SteatoTest (BioPredictive, Paris, France), and NAFLD liver fat score are well-validated models to detect steatosis in the general population [42]. FLI, NAFLD liver fat score, hepatic steatosis index (HSI), and comprehensive/simple NAFLD scores (CNS/SNS) were externally validated in the Korean population. Depending on population characteristics, cut-off values of these models might be adjusted to improve sensitivity and specificity [80]. Epidemiologic studies with no imaging information can apply these models to calculate an operational definition for hepatic steatosis [88], but prudent interpretation/application of multiple models is needed. However, these biomarker-based indices do not add much diagnostic information for clinicians who routinely perform imaging studies such as US for patients with suspected NAFLD.
NASH
Currently there are no well-established prediction models or biomarkers to distinguish NASH from steatosis, despite intensive efforts [42]. Circulating levels of cytokeratin-18 (CK-18) fragments, which are released from apoptotic or dead cells, have been extensively investigated as a novel biomarker [89]; however, its clinical utility remains unknown due to low reproducibility and measurement issues [90]. Other panels combined with novel biomarkers, such as NASH test (BioPredictive) [91], NASH diagnostics [92], and OxNASH score [93] have been introduced. Further research is required to validate their accuracy and practical utility.
Hepatic fibrosis
Severity of hepatic fibrosis is the most powerful determinant of long-term outcomes, including mortality [94 95]; thus, noninvasive assessment of fibrosis is essential to manage patients with NAFLD. Beyond imaging modalities to estimate hepatic fibrosis, several prediction scores have been developed and validated to identify or exclude advanced fibrosis. Focusing on reliable blood-based predictive models in the NAFLD guidelines, equations, cut-points for advanced fibrosis (F3), information about the original development cohort, and external validation in individuals with NAFLD are summarized in Table 4 [96 97 98 99 100 101 102 103 104]. This review does not compare diagnostic performance of these models due to limited space.
Contrary to steatosis or NASH scores, fibrosis prediction models in clinical practice are recommended in the recent NAFLD guidelines [40 42] because some models have achieved acceptable accuracy to detect significant fibrosis and have been widely validated in NAFLD patients. The NAFLD fibrosis score (NFS) [96] and fibrosis-4 (FIB-4) index [97] are currently the most studied decision-making systems and are clinically endorsed by both European and United States NAFLD guide lines. The National Institute for Health and Care Excellence (NICE, London, United Kingdom) recommended use of the Enhanced Liver Fibrosis (ELF) panel, a commercial diagnostic kit using fibrosis-related biomarkers, for NAFLD management. These blood-based fibrosis prediction models perform better when excluding advanced fibrosis versus diagnosing it, due to higher negative predictive values [105]. Therefore, combining results from both imaging modalities and biomarker-based scores may be a better approach to identify ambiguous patients at risk for advanced fibrosis or who need liver biopsy.
CONCLUSIONS
Compared to the general population, NAFLD is widely prevalent in patients with T2DM, and incidence of both metabolic diseases is steadily increasing worldwide. Accumulating evidence indicates that T2DM is considered an emerging risk factor for NASH and/or fibrosis and that NAFLD may worsen diabetes-related health outcomes, such as vascular complications, and mortality. Extensive assessment of NAFLD severity and of cardiometabolic risk profiles is highly recommended for management of patients with T2DM. Although many imaging modalities and biomarker-based prediction models have been developed to evaluate NAFLD disease status, more investigation is required before their application in routine clinical care.
ACKNOWLEDGMENTS
Editorial assistance was provided by Caron Modeas.
Notes
CONFLICTS OF INTEREST: No potential conflict of interest relevant to this article was reported.