
- Current
- Browse
- Collections
-
For contributors
- For Authors
- Instructions to authors
- Article processing charge
- e-submission
- For Reviewers
- Instructions for reviewers
- How to become a reviewer
- Best reviewers
- For Readers
- Readership
- Subscription
- Permission guidelines
- About
- Editorial policy
Articles
- Page Path
- HOME > Diabetes Metab J > Volume 44(1); 2020 > Article
-
Original ArticleLifesytle Combined Aerobic and Resistance Exercise Training Reduces Circulating Apolipoprotein J Levels and Improves Insulin Resistance in Postmenopausal Diabetic Women
-
Yun Kyung Jeon1,2
 , Sang Soo Kim1,2,3
, Sang Soo Kim1,2,3 , Jong Ho Kim1,2, Hyun Jeong Kim3, Hyun Jun Kim4, Jang Jun Park4, Yuen Suk Cho5, So Hee Joung6, Ji Ryang Kim7, Bo Hyun Kim1,2, Sang Heon Song2,8, In Joo Kim1,2, Yong Ki Kim7, Young-Bum Kim3
, Jong Ho Kim1,2, Hyun Jeong Kim3, Hyun Jun Kim4, Jang Jun Park4, Yuen Suk Cho5, So Hee Joung6, Ji Ryang Kim7, Bo Hyun Kim1,2, Sang Heon Song2,8, In Joo Kim1,2, Yong Ki Kim7, Young-Bum Kim3
-
Diabetes & Metabolism Journal 2020;44(1):103-112.
DOI: https://doi.org/10.4093/dmj.2018.0160
Published online: February 21, 2020
1Division of Endocrinology and Metabolism, Department of Internal Medicine, Pusan National University Hospital, Pusan National University School of Medicine, Busan, Korea.
2Biomedical Research Institute, Pusan National University Hospital, Busan, Korea.
3Division of Endocrinology, Diabetes, and Metabolism, Department of Medicine, Beth Israel Deaconess Medical Center, Harvard Medical School, Boston, MA, USA.
4Department of Physical Education, Kyungnam University College of Education, Changwon, Korea.
5Department of Marine Sports, Pukyong National University, Busan, Korea.
6Nutrition Service Team, Pusan National University Hospital, Busan, Korea.
7Kim Yong Ki Internal Medicine Clinic, Busan, Korea.
8Division of Nephrology, Department of Internal Medicine, Pusan National University Hospital, Pusan National University School of Medicine, Busan, Korea.
- Corresponding author: Young-Bum Kim. Division of Endocrinology, Diabetes, and Metabolism, Department of Medicine, Beth Israel Deaconess Medical Center, Harvard Medical School, 330 Brookline Avenue, CLS-745, Boston, MA 02215, USA. ykim2@bidmc.harvard.edu
- Corresponding author: Sang Soo Kim. Division of Endocrinology and Metabolism, Department of Internal Medicine, Pusan National University Hospital, Pusan National University School of Medicine, 179 Gudeok-ro, Seo-gu, Busan 49241, Korea. drsskim7@gmail.com
Copyright © 2020 Korean Diabetes Association
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
ABSTRACT
-
Background
- Circulating apolipoprotein J (ApoJ) is closely associated with insulin resistance; however, the effect of exercise on circulating ApoJ levels and the association of ApoJ with metabolic indices remain unknown. Here, we investigated whether a combined exercise can alter the circulating ApoJ level, and whether these changes are associated with metabolic indices in patients with type 2 diabetes mellitus.
-
Methods
- Postmenopausal women with type 2 diabetes mellitus were randomly assigned into either an exercise (EXE, n=30) or control (CON, n=15) group. Participants in the EXE group were enrolled in a 12-week program consisting of a combination of aerobic and resistance exercises. At baseline, 4, 8, and 12 weeks, body composition and metabolic parameters including homeostatic model assessment of insulin resistance (HOMA-IR) and serum ApoJ levels were assessed.
-
Results
- In the EXE group, ApoJ levels decreased 26.3% and 19.4%, relative to baseline, at 8 and 12 weeks, respectively. Between-group differences were significant at 8 and 12 weeks (P<0.05 and P<0.001, respectively). In the EXE group, 12 weeks of exercise resulted in significant decreases in body weight, percent body fat, and HOMA-IR indices. Concurrently, weight-adjusted appendicular skeletal muscle mass (ASM/wt) was increased in the EXE group compared with the CON group. Importantly, changes in the ApoJ level were significantly correlated with changes in ASM/wt.
-
Conclusion
- Exercise training resulted in a significant decrease in the circulating ApoJ level, with changes in ApoJ associated with an improvement in some insulin resistance indices. These data suggest that circulating ApoJ may be a useful metabolic marker for assessing the effects of exercise on insulin resistance.
- The clinical and economic burden associated with diabetes mellitus and its management remain an enduring challenge to the healthcare community [12]. The primary clinical outcomes of type 2 diabetes mellitus (T2DM) include insulin resistance, abdominal obesity, and elevated glucose and triglyceride levels [3]. Metabolic organs including muscle, liver, and adipose tissue are involved in insulin resistance, of which the failure of muscle to response to insulin is thought to be a key pathophysiological factor in the development of T2DM [4]. These tissues have been shown to regulate glucose homeostasis via the secretion of various biologically and metabolically active polypeptide factors, providing an important conceptual framework to understand the pathophysiology of insulin resistance and T2DM.
- Apolipoprotein J (ApoJ), also known as clusterin, is a disulfide-linked heterodimeric protein that is ubiquitously expressed in various tissues and bodily fluids [5]. An increase in the level of circulating ApoJ has been linked to various pathophysiologic conditions, including Alzheimer's disease, neoplastic conditions, and cardiovascular diseases [678]. Emerging data suggest that circulating ApoJ is closely correlated with markers of cardiovascular metabolism, suggesting a link between ApoJ and insulin resistance in human subjects [91011]. Previous work by our group demonstrated that changes in serum ApoJ levels by insulin-sensitizing therapy was inversely associated with changes in the glucose disposal rate in patients with T2DM, suggesting that circulating ApoJ is a marker of insulin resistance [12].
- Exercise is recognized as a critical factor for T2DM prevention and treatment, providing significant improvements in insulin sensitivity and diabetes-related health complications with minimal undesired side effects [13]. Whereas aerobic exercise enhances insulin sensitivity, resistance training improves blood glucose uptake by increasing muscle mass and Glut4 expression, with synergistic effects possible between the two exercise types [14]. Based on these observations, current guidelines recommend that patients with T2DM should enroll in combined exercise programs to manage their glucose levels and insulin resistance [15]; however, details regarding the effects of combined exercise training on insulin resistance in diabetic individuals are limited [16].
- Here, we examined the circulating ApoJ level and various cardiometabolic risk factors in postmenopausal patients with T2DM after introduction of combined aerobic exercise and resistance training for 12 weeks. The goal of this study was to assess the effects of combined aerobic and resistance training on the circulating ApoJ level and other cardiometabolic risk factors as potential markers of insulin resistance in postmenopausal women with T2DM.
INTRODUCTION
- Participants
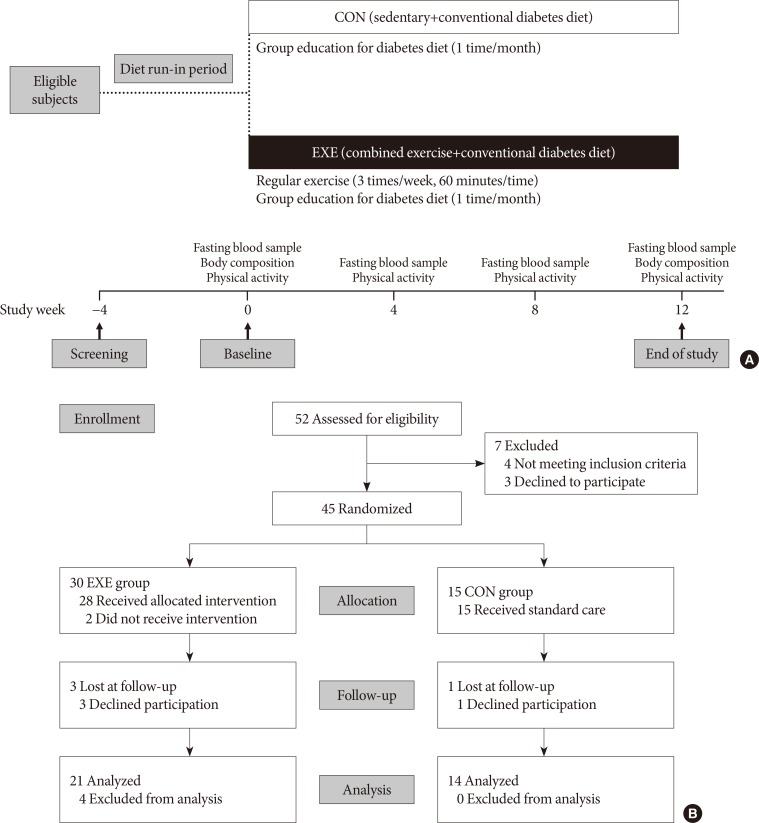
- This study was approved by the Institutional Review Broad of Pusan National University Hospital (1306-004-019) and was performed in accordance with the Declaration of Helsinki. The current study was registered at the National Clinical Trial Registry (clinical trial no. KCT0004671; https://cris.nih.go.kr/cris/). Written informed consent was obtained from all subjects before enrollment in the study. To establish the effect of combined exercise on cardiometabolic parameters in T2DM, we enrolled postmenopausal women with T2DM from Pusan National University Hospital in Busan, Korea. The exclusion criteria were as follows: (1) active infection within the past month; (2) a recent history of acute myocardial infarction, stroke, trauma, or surgery; (3) neoplastic disorder; (4) occlusive peripheral vascular disease; (5) severe liver dysfunction; (6) taking antidepressants or neurotrophic drugs; and (7) Alzheimer's disease. We used power analysis to determine the sample size. Extrapolating for a medium size effect of 0.40, a minimum sample of 46 subjects was needed to achieve a power of 0.85 with an alpha level of 0.05. However, taking into account the possible 10% sample loss, a total of 50 patients were selected. A flowchart describing the selection of participants from the initial screening to the study endpoint is shown in Fig. 1. Of the initial 52 patients who were recruited, seven were excluded during the screening process, with the remaining 45 randomly assigned to either of the two groups. All participants were provided dietary consultation for diabetes by a clinical nutritionist (S.H.J.) 1 month before randomization. Then, they were randomly assigned to two groups, the exercise (EXE, n=30) and control (CON, n=15) groups at a ratio of 2:1. The participants in the EXE group performed combined aerobic exercise and resistance training, whereas those in the CON group performed no additional exercise during the 12-week period. Dietary consultation was provided to participants in both groups every month during the study period. At baseline, 4, 8, and 12 weeks, we measured body composition and metabolic parameters including homeostatic model assessment of insulin resistance (HOMA-IR) and the serum ApoJ level using enzyme-linked immunosorbent assay (ELISA).
- Exercise protocol
- The combined exercise program consisted of aerobic exercise and resistance training for 12 weeks. All exercise sessions were supervised by exercise physiologists and endocrinologists. Aerobic exercises entailed folk dances composed of rhythmic movements to music matching the emotions of older women. Exercise frequency was three times a week (Monday, Wednesday, and Friday) for a total of 12 weeks. Exercise duration was 20 minutes each day, including warm-up for 5 minutes and cool-down for 5 minutes. To enhance the aerobic effect and interest in the programs, exercise intensity was provided as rated perceived exertion (RPE) scale 11 to 12 (light) for weeks 1 to 4 and RPE scale 13 to 14 (somewhat hard) for weeks 5 to 12. Heart rate was measured using an X-trainer heart rate monitor (Polar Electro Oy, Kempele, Finland).
- Resistance training involved performance of rubber band exercises three times each week. The exercise duration was approximately 30 minutes each day. The intensity was provided as RPE 11 to 12 (light) for weeks 1 to 4 and RPE 13 to 14 (somewhat hard) for weeks 5 to 12. Rubber band exercises consisted of nine movements to work the large and small muscle groups as described previously [17]: bench press, squat, elbow curl, seated row, knee curl, sit-up, knee extension, overhead press, and seated leg press. Each movement was performed at 70% of the maximal single-repetition resistance. Resistance was increased slowly if the participant could perform 20 repetitions without failure. To increase resistance within the recommended stretch distance of the rubber resistance equipment, participants increased the thickness of the rubber band being stretched. This was achieved using the range of different thicknesses of the resistance product.
- Metabolic and anthropometric measurements
- Body height and weight were measured using a digital electronic scale with participants wearing light clothing and no shoes. Waist circumference was measured horizontally at the level of the umbilicus. Body composition was measured using dual-energy X-ray absorptiometry (Lunar Prodigy; GE Medical Systems, Milwaukee, WI, USA). Blood samples were drawn at 8:00 AM after at least 12 hours of fasting from the antecubital vein of each participant. The blood samples were collected at baseline (0 week), 4, 8, and 12 weeks after randomization. Plasma samples were prepared within 30 minutes of collection by centrifugation for 15 minutes at 3,000 rpm; plasma was removed and stored at −70℃ until analysis. The plasma concentration of ApoJ was measured using a commercial ELISA kit (Boster Biological Technology, Pleasanton, CA, USA) according to the manufacture's protocols. Samples were diluted to enable analysis within the range of the standard curve (0.78 to 50 ng/mL). The sensitivity of the assay was <20 pg/mL. The intra- and inter-assay coefficients of variation were 4.2% to 4.6% and 6.9% to 7.5%, respectively. All samples were analyzed in duplicate. Serum glucose concentrations were measured within 4 hours of collection using Cobas (Roche Diagnostics, Mannheim, Germany). Serum insulin levels were measured by radioimmunoassay (Asbach Medical Products GmBH, Obrigheim, Germany). The intra- and inter-assay coefficients of variation were 2.1% and 6.5%, respectively. The HOMA-IR index was calculated using the formula: fasting plasma glucose (mmol/L)×fasting plasma insulin (mU/L)/22.5 [18].
- Statistical analysis
- Statistical analyses were performed using SPSS version 18.0 for Windows (SPSS Inc., Chicago, IL, USA). Data are presented as mean±standard deviation for normally distributed values and as median (interquartile range) for nonparametric values. Distributions of the continuous variables were examined for skewedness and kurtosis, and variables with a non-Gaussian distribution were logarithm-transformed prior to analysis. Geometric means are presented with 95% confidence intervals. The Mann-Whitney U test or independent Student's t-test was used to compare the baseline characteristics, as well as changes in the metabolic and anthropometric parameters and ApoJ levels, of the subjects between the between the CON and EXE groups after the 12-week period. Categorical variables are reported as frequencies and percentages and were compared using the chi-square test. Spearman's rank correlation analysis was used to assess the correlations between individual continuous variables. We used repeated-measures analysis of variance (ANOVA) on both time (baseline vs. post-exercise) and group (CON vs. EXE) factors to compare circulating ApoJ levels and other parameters at baseline, 4, 8, and 12 weeks after intervention. A P value of <0.05 derived from two-tailed Student's t-tests was considered statistically significant.
METHODS
- During the follow-up period, four subjects declined participation (EXE, n=3; CON, n=1). An additional four participants from the EXE group did not meet attendance criteria for the exercise program (≥80%). Thus, the final data analyses were based on 34 participants (EXE, n=20; CON, n=14) (Fig. 1B). The key characteristics of the subjects (n=34) utilized in the analyses, including anthropometric measures, metabolic parameters, and demographic features, are shown in Table 1. The mean age of the patients was 61.3±8.8 years. The mean duration of diabetes was 9.5±7.9 years, and the mean body mass index (BMI) was 24.9±2.8 kg/m2 . There were no significant differences in any metabolic or anthropometric parameter between the two groups at baseline (Table 1). At baseline, the median serum ApoJ level was 133.3±22.0 µg/mL and did not differ significantly between the two groups (135.6±22.9 µg/mL in EXE vs. 128.3±20.6 µg/mL in CON, P=0.299).
- At week 12, body weight was significantly lower in the EXE than CON group (P=0.014 vs. at baseline in EXE; P=0.451 vs. at baseline in CON). After 12 weeks, total fat (%) and total fat mass (g) were decreased in both the CON and EXE groups (P=0.017 vs. P=0.040 and P=0.011 vs. P=0.017, respectively) relative to baseline. Weight-adjusted appendicular skeletal muscle mass (ASM/wt) was significantly increased in the EXE (P=0.005) but not the CON (P=0.820) group at 12 weeks relative to baseline. There was no significant change in glycosylated hemoglobin (HbA1c), android fat mass, or ASM between baseline and week 12 in either the EXE or CON group (P=0.278 vs. P=0.363, P=0.289 vs. P=0.865, P=0.170 vs. P=0.460, and P=0.434 vs. P=0.650, respectively). However, the level of high density lipoprotein (HDL)-cholesterol was greatly increased in the EXE (P=0.026), but not CON (P=0.573), group at week 12. The HOMA-IR value at the end of exercise was below that at baseline in the EXE, although this difference was not statistically significant (P=0.054). No significant difference was found in the HOMA-IR value between baseline and week 12 in the CON (P=0.617).
- At baseline, the circulating ApoJ level in all patients was significantly correlated with the level of HDL-cholesterol (r=302, P=0.048) and ASM/wt (r=−0.332, P=0.019) (Supplementary Table 1). In contrast, the level of circulating ApoJ was positively correlated, albeit not significantly, with HbA1c (r=286, P=0.079) and HOMA-IR (r=297, P=0.067) at baseline.
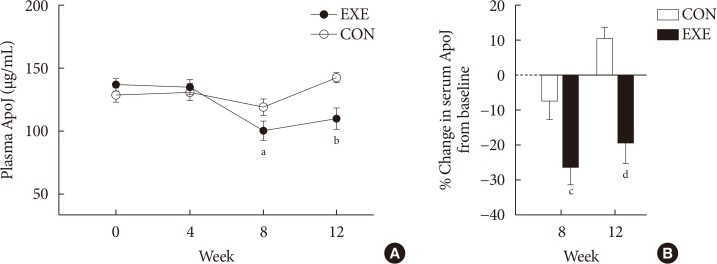
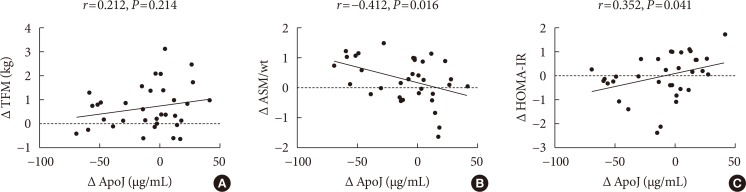
- At weeks 8 and 12, the circulating ApoJ level was significantly lower in the EXE than CON (P=0.019 at week 8 and P=0.007 at week 12 by repeated-measures ANOVA) (Fig. 2A). In the EXE, the ApoJ level decreased 26.3% and 19.4% relative to baseline at weeks 8 and 12, respectively (Fig. 2B), and was significantly different between the two groups at weeks 8 and 12 (P<0.05 and P<0.001, respectively). Changes in the ApoJ level from baseline to the end of the 12-week period were not significantly correlated with changes in HbA1c, blood pressure, lipid profiles, body weight, or fat mass in all participants (Table 2). No relationship between the changes in body fat and ApoJ level was observed (r=0.212, P=0.214) (Fig. 3A); however, the decreased circulating ApoJ level after 12 weeks of combined exercise was significantly correlated with the changes in ASM/wt (r=−0.412, P=0.016) (Fig. 3B) and HOMA-IR (r=0.352, P=0.041) (Fig. 3C) in an unadjusted analysis (Table 2). After adjusting for age, the change in ApoJ level remained significantly associated with ASM/wt only (r=−0.408, P=0.024).
RESULTS
- The data presented here show that exercise training resulted in significant improvements in insulin resistance-related outcomes, including increased ASM/wt, and these improvements were associated with a decreased circulating ApoJ level in postmenopausal women with T2DM. This study provides clear evidence supporting circulating ApoJ as a metabolic marker of insulin resistance, as well as the ability of a combined exercise to improve sarcopenic obesity in insulin-resistant individuals.
- The circulating ApoJ level was significantly increased in individuals with conditions associated with insulin resistance such as obesity, metabolic syndrome, and T2DM [91219]. Following therapeutic intervention using a combination of weight reduction and thiazolidinedione to improve insulin sensitivity, circulating ApoJ levels were reduced [1220]. The data presented here build on those previous results, showing that a decrease in the circulating ApoJ level induced by physical exercise is accompanied by improvements in important insulin resistance indices, such as HOMA-IR, in T2DM. Together, these data support the notion that upregulation of circulating ApoJ is a feature of metabolically dysregulated states in insulin resistance conditions, including T2DM. Further support for this hypothesis comes from the finding that oral administration of ApoJ reduced atherosclerosis in ApoE-null mice and improved HDL inflammatory properties in monkeys [21]. In line with these findings, ApoJ was shown to play a protective role in individuals with insulin resistance, and an elevated serum ApoJ level may be the manifestation of adaptive or secondary effects, suggesting that circulating ApoJ is a useful maker for evaluating insulin resistance.
- Sarcopenic obesity, defined as a loss of muscle mass and muscle strength, is prevalent among older diabetic patients and is closely related to insulin resistance [2223]. Of note, the current study found that the reduced circulating ApoJ level after exercise was correlated with an increase in skeletal muscle mass, although it remains uncertain whether exercise or the change in muscle mass itself was responsible for the change in the serum ApoJ level. Whereas no significant change in the serum ApoJ level was observed in subjects without changes in muscle mass in the EXE (data not shown), definitive conclusions are not possible due to the small number of subjects in the study and the strong correlation between muscle mass and the reduction in circulating ApoJ. Recent work from our lab demonstrated that muscle-specific deletion of low density lipoprotein (LDL) receptor-related protein 2, a potential receptor for ApoJ, resulted in an increased serum ApoJ level and insulin resistance in mice (not published). However, the mechanism by which acute endurance exercise affects the metabolic actions of ApoJ on muscle metabolism is unclear. Future study is needed to clarify this important issue.
- A prior study found that the ApoJ level was not correlated with either BMI or the degree of weight loss, although weight loss lowered circulating ApoJ concentrations in obese patients [20]. These results are consistent with the data presented here showing that the circulating ApoJ level was not correlated with either body weight or fat mass. However, when we reclassified patients as those with and those without body weight change after exercise, ApoJ levels were significantly decreased only in the body weight change group (Supplementary Fig. 1). These data suggest that both an increase in skeletal muscle mass and a decrease in adiposity can affect the level of circulating ApoJ. Thus, we are able to explain why changes in the serum ApoJ level were not correlated with changes in ASM but were correlated with changes in ASM/wt.
- Emerging evidence suggests that the circulating ApoJ level is independently correlated with insulin sensitivity in both healthy subjects and diabetic patients [1112]. However, we observed only marginal correlations between several insulin sensitivity indices and the circulating ApoJ level at baseline. In addition, there was a weak correlation between changes in insulin resistance and the circulating ApoJ level with physical exercise training, although this association did not reach statistically significance. These results are concordant with our previous data showing that circulating ApoJ was clearly correlated with metabolic parameters of insulin resistance in healthy subjects but not in those with T2DM [12]. This discrepancy could be explained by several possibilities. First, the diabetic patients in the current study had a relatively long duration of diabetes (approximately 10 years) and insulin deficiency due to β-cell failure. Second, because we did not exclude patients who were using insulin at enrollment, it is possible that insulin supplementation could have affected the serum ApoJ level during the course of exercise training. Third, many of the subjects enrolled in this study were taking a variety of prescriptions that potentially could have affected insulin sensitivity during the study period (Supplementary Table 2). However, there was no significant difference in the proportion of prescriptions affecting insulin sensitivity between the groups and no changes reported during the study period. Last, HOMA-IR might be not a reliable method for estimating insulin resistance, particularly in patients with advanced T2DM.
- Rather, this variable is likely appropriate for epidemiologic studies involving a larger number of subjects [24]. The glucose clamp technique may be a more suitable method for assessing insulin sensitivity in skeletal muscle [25].
- Several studies have reported that circulating ApoJ is significantly correlated with total cholesterol and LDL-cholesterol levels [102627]; however, there was no discernible evidence of a close relationship between changes in the ApoJ level and lipid profiles after combined exercise. One possible explanation for this could be that most participants had already taken cholesterol-lowering statins (Supplementary Table 2).
- The limitations of the current study include the relatively small number of participants and the narrow spectrum of the population stemming from our selective use of Korean postmenopausal women with T2DM. We cannot exclude the possibility that circulating ApoJ levels induced by exercise training vary among different populations of obese patients with T2DM in Western countries. As this study was performed only in postmenopausal women, these findings cannot be generalized to either men or premenopausal women. Second, the 12-week intervention period may have been too brief to accurately determine the effects of exercise on ApoJ level and insulin sensitivity. Finally, changes in the serum ApoJ level were not correlated with changes in ASM but rather with changes in ASM/wt. Further studies examining a larger cohort of patients will be needed to clarify this discrepancy.
- Taken together, the data presented here provide the first evidence demonstrating the regulation of circulating ApoJ in response to physical exercise in humans with T2DM. Interestingly, the circulating ApoJ level was markedly decreased by exercise training, and the change in the ApoJ level was inversely correlated with the change in muscle mass in patients with T2DM, along with an improvement in insulin sensitivity. Thus, circulating ApoJ could be a useful metabolic marker of the insulin-sensitizing effect of physical exercise in patients with T2DM.
DISCUSSION
-
Acknowledgements
- None
ACKNOWLEDGMENTS
-
CONFLICTS OF INTEREST: This work was supported by grants from the National Institutes of Health (R01DK111529 and R01DK106076 to Young-Bum Kim), R&D project grant from Yuhan pharmaceutical corporation (to Sang Soo Kim) and National Research Foundation of Korea (2018R1C1B6002854 to Sang Soo Kim).
-
AUTHOR CONTRIBUTION:
Conception or design: Y.K.J., S.S.K., I.J.K., Y.B.K.
Acquisition, analysis, or interpretation of data: Y.K.J., S.S.K., J.H.K., H.J.K., H.J.K., J.J.P., Y.S.C., S.H.J., J.R.K., B.H.K., S.H.S., I.J.K., Y.K.K., Y.B.K.
Drafting the work or revising: Y.K.J., S.S.K., Y.B.K.
Final approval of the manuscript: Y.K.J., S.S.K., J.H.K., H.J.K., H.J.K., J.J.P., Y.S.C., S.H.J., J.R.K., B.H.K., S.H.S., I.J.K., Y.K.K., Y.B.K.
NOTES
SUPPLEMENTARY MATERIALS
Supplementary Table 1
Supplementary Fig. 1
- 1. Danaei G, Finucane MM, Lu Y, Singh GM, Cowan MJ, Paciorek CJ, Lin JK, Farzadfar F, Khang YH, Stevens GA, Rao M, Ali MK, Riley LM, Robinson CA, Ezzati M. Global Burden of Metabolic Risk Factors of Chronic Diseases Collaborating Group (Blood Glucose). National, regional, and global trends in fasting plasma glucose and diabetes prevalence since 1980: systematic analysis of health examination surveys and epidemiological studies with 370 country-years and 2·7 million participants. Lancet 2011;378:31-40. ArticlePubMed
- 2. Miller BR, Nguyen H, Hu CJ, Lin C, Nguyen QT. New and emerging drugs and targets for type 2 diabetes: reviewing the evidence. Am Health Drug Benefits 2014;7:452-463. PubMedPMC
- 3. Wilcox G. Insulin and insulin resistance. Clin Biochem Rev 2005;26:19-39. PubMedPMC
- 4. Kim YB, Nikoulina SE, Ciaraldi TP, Henry RR, Kahn BB. Normal insulin-dependent activation of Akt/protein kinase B, with diminished activation of phosphoinositide 3-kinase, in muscle in type 2 diabetes. J Clin Invest 1999;104:733-741. ArticlePubMedPMC
- 5. Trougakos IP, Gonos ES. Clusterin/apolipoprotein J in human aging and cancer. Int J Biochem Cell Biol 2002;34:1430-1448. ArticlePubMed
- 6. Miwa Y, Takiuchi S, Kamide K, Yoshii M, Horio T, Tanaka C, Banno M, Miyata T, Sasaguri T, Kawano Y. Insertion/deletion polymorphism in clusterin gene influences serum lipid levels and carotid intima-media thickness in hypertensive Japanese females. Biochem Biophys Res Commun 2005;331:1587-1593. ArticlePubMed
- 7. Thambisetty M, Simmons A, Velayudhan L, Hye A, Campbell J, Zhang Y, Wahlund LO, Westman E, Kinsey A, Guntert A, Proitsi P, Powell J, Causevic M, Killick R, Lunnon K, Lynham S, Broadstock M, Choudhry F, Howlett DR, Williams RJ, Sharp SI, Mitchelmore C, Tunnard C, Leung R, Foy C, O'Brien D, Breen G, Furney SJ, Ward M, Kloszewska I, Mecocci P, Soininen H, Tsolaki M, Vellas B, Hodges A, Murphy DG, Parkins S, Richardson JC, Resnick SM, Ferrucci L, Wong DF, Zhou Y, Muehlboeck S, Evans A, Francis PT, Spenger C, Lovestone S. Association of plasma clusterin concentration with severity, pathology, and progression in Alzheimer disease. Arch Gen Psychiatry 2010;67:739-748. ArticlePubMedPMC
- 8. Bi J, Guo AL, Lai YR, Li B, Zhong JM, Wu HQ, Xie Z, He YL, Lv ZL, Lau SH, Wang Q, Huang XH, Zhang LJ, Wen JM, Guan XY. Overexpression of clusterin correlates with tumor progression, metastasis in gastric cancer: a study on tissue microarrays. Neoplasma 2010;57:191-197. ArticlePubMed
- 9. Won JC, Park CY, Oh SW, Lee ES, Youn BS, Kim MS. Plasma clusterin (ApoJ) levels are associated with adiposity and systemic inflammation. PLoS One 2014;9:e103351. ArticlePubMedPMC
- 10. Baralla A, Sotgiu E, Deiana M, Pasella S, Pinna S, Mannu A, Canu E, Sotgiu G, Ganau A, Zinellu A, Sotgia S, Carru C, Deiana L. Plasma clusterin and lipid profile: a link with aging and cardiovascular diseases in a population with a consistent number of centenarians. PLoS One 2015;10:e0128029. ArticlePubMedPMC
- 11. Hoofnagle AN, Wu M, Gosmanova AK, Becker JO, Wijsman EM, Brunzell JD, Kahn SE, Knopp RH, Lyons TJ, Heinecke JW. Low clusterin levels in high-density lipoprotein associate with insulin resistance, obesity, and dyslipoproteinemia. Arterioscler Thromb Vasc Biol 2010;30:2528-2534. ArticlePubMedPMC
- 12. Seo JA, Kang MC, Ciaraldi TP, Kim SS, Park KS, Choe C, Hwang WM, Lim DM, Farr O, Mantzoros C, Henry RR, Kim YB. Circulating ApoJ is closely associated with insulin resistance in human subjects. Metabolism 2018;78:155-166. ArticlePubMed
- 13. Zanuso S, Jimenez A, Pugliese G, Corigliano G, Balducci S. Exercise for the management of type 2 diabetes: a review of the evidence. Acta Diabetol 2010;47:15-22. ArticlePubMedPDF
- 14. Oliveira C, Simoes M, Carvalho J, Ribeiro J. Combined exercise for people with type 2 diabetes mellitus: a systematic review. Diabetes Res Clin Pract 2012;98:187-198. ArticlePubMed
- 15. Colberg SR, Sigal RJ, Fernhall B, Regensteiner JG, Blissmer BJ, Rubin RR, Chasan-Taber L, Albright AL, Braun B. American College of Sports Medicine. American Diabetes Association. Exercise and type 2 diabetes: the American College of Sports Medicine and the American Diabetes Association: joint position statement executive summary. Diabetes Care 2010;33:2692-2696. PubMedPMC
- 16. Way KL, Hackett DA, Baker MK, Johnson NA. The effect of regular exercise on insulin sensitivity in type 2 diabetes mellitus: a systematic review and meta-analysis. Diabetes Metab J 2016;40:253-271. ArticlePubMedPMCPDF
- 17. Kim HJ, Lee S, Kim TW, Kim HH, Jeon TY, Yoon YS, Oh SW, Kwak H, Lee JG. Effects of exercise-induced weight loss on acylated and unacylated ghrelin in overweight children. Clin Endocrinol (Oxf) 2008;68:416-422. ArticlePubMedPDF
- 18. Matthews DR, Hosker JP, Rudenski AS, Naylor BA, Treacher DF, Turner RC. Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia 1985;28:412-419. ArticlePubMedPDF
- 19. Trougakos IP, Poulakou M, Stathatos M, Chalikia A, Melidonis A, Gonos ES. Serum levels of the senescence biomarker clusterin/apolipoprotein J increase significantly in diabetes type II and during development of coronary heart disease or at myocardial infarction. Exp Gerontol 2002;37:1175-1187. ArticlePubMed
- 20. Arnold T, Brandlhofer S, Vrtikapa K, Stangl H, Hermann M, Zwiauer K, Mangge H, Karwautz A, Huemer J, Koller D, Schneider WJ, Strobl W. Effect of obesity on plasma clusterin, [corrected] a proposed modulator of leptin action. Pediatr Res 2011;69:237-242. ArticlePubMed
- 21. Navab M, Anantharamaiah GM, Reddy ST, Van Lenten BJ, Wagner AC, Hama S, Hough G, Bachini E, Garber DW, Mishra VK, Palgunachari MN, Fogelman AM. An oral apoJ peptide renders HDL antiinflammatory in mice and monkeys and dramatically reduces atherosclerosis in apolipoprotein E-null mice. Arterioscler Thromb Vasc Biol 2005;25:1932-1937. ArticlePubMed
- 22. Choi KM. Sarcopenia and sarcopenic obesity. Korean J Intern Med 2016;31:1054-1060. ArticlePubMedPMCPDF
- 23. Jang HC. Sarcopenia, frailty, and diabetes in older adults. Diabetes Metab J 2016;40:182-189. ArticlePubMedPMCPDF
- 24. Kang ES, Yun YS, Park SW, Kim HJ, Ahn CW, Song YD, Cha BS, Lim SK, Kim KR, Lee HC. Limitation of the validity of the homeostasis model assessment as an index of insulin resistance in Korea. Metabolism 2005;54:206-211. ArticlePubMed
- 25. DeFronzo RA, Tobin JD, Andres R. Glucose clamp technique: a method for quantifying insulin secretion and resistance. Am J Physiol 1979;237:E214-E223. ArticlePubMed
- 26. Rull A, Martinez-Bujidos M, Perez-Cuellar M, Perez A, Ordonez-Llanos J, Sanchez-Quesada JL. Increased concentration of clusterin/apolipoprotein J (apoJ) in hyperlipemic serum is paradoxically associated with decreased apoJ content in lipoproteins. Atherosclerosis 2015;241:463-470. ArticlePubMed
- 27. Aronis KN, Vamvini MT, Chamberland JP, Mantzoros CS. Circulating clusterin (apolipoprotein J) levels do not have any day/night variability and are positively associated with total and LDL cholesterol levels in young healthy individuals. J Clin Endocrinol Metab 2011;96:E1871-E1875. ArticlePubMedPMC
REFERENCES
Study design and patient disposition. (A) Schematic of the study design. (B) Details of patient disposition. CON, control group; EXE, exercise group.
Effects of a combined exercise regimen on the circulating apolipoprotein J (ApoJ) level in postmenopausal women with type 2 diabetes mellitus. (A) Change in the serum ApoJ level over the course of the exercise program. Significant differences in the circulating ApoJ level between the exercise group (EXE) and control group (CON) are shown. (B) Percent changes in the serum ApoJ level, relative to baseline, at weeks 8 and 12. Values are mean±standard error. aP=0.019 at week 8, bP=0.007 at week 12, by repeated-measures analysis of variance, cP<0.05 vs. CON, dP<0.001 vs. CON.
Correlations of changes in the circulating apolipoprotein J (ApoJ) level with changes in (A) total fat mass (TFM), (B) weight-adjusted appendicular skeletal muscle mass (ASM/wt), and (C) homeostatic model assessment of insulin resistance (HOMA-IR). Data represent Spearman's rank correlation coefficients and P values. Δ indicates the value at baseline minus that at 12 weeks.
Metabolic and anthropometric parameters of study participants at baseline and at 12 weeks after intervention week after intervention
Values are presented as mean±standard deviation and median (interquartile range).
EXE, exercise group; CON, control group; NA, not applicable; SBP, systolic blood pressure; DBP, diastolic blood pressure; HbA1c, glycosylated hemoglobin; eGFR, estimated glomerular filtration rate; LDL-C, low-density lipoprotein cholesterol; HDL-C, high-density lipoprotein cholesterol; CRP, C-reactive protein; HOMA-IR, homeostatic model assessment of insulin resistance; ApoJ, apolipoprotein J; ACR, albumin-to-creatinine ratio; WC, waist circumference; BMI, body mass index; ASM, appendicular skeletal muscle mass; wt, weight.
aP>0.05 by two sample t-test or Mann-Whitney U test between two groups at baseline, bPaired t-test or Wilcoxon signed ranks test for within group, cTwo-way repeated measures analysis of variance over time for between groups, dLogarithm-transformed values were used for comparison.
Correlations of ΔApoJ with changes in other metabolic and anthropometric parameters at the end of the 12 weeks after combined exercise
Data represent Spearman's rank correlation coefficient values and P values. Δ indicates data at baseline minus data at 12 weeks.
ApoJ, apolipoprotein J; BMI, body mass index; SBP, systolic blood pressure; DBP, diastolic blood pressure; HbA1c, glycosylated hemoglobin; LDL-C, low-density lipoprotein cholesterol; HDL-C, high-density lipoprotein cholesterol; HOMA-IR, homeostatic model assessment of insulin resistance; WC, waist circumference; ASM, appendicular skeletal muscle mass; wt, weight.
aOnly age (not BMI) adjusted in anthropometric parameters, bLogarithm-transformed values were used for comparison.
Figure & Data
References
Citations

- The function of previously unappreciated exerkines secreted by muscle in regulation of neurodegenerative diseases
Xuepeng Bian, Qian Wang, Yibing Wang, Shujie Lou
Frontiers in Molecular Neuroscience.2024;[Epub] CrossRef - Exercise modalities for type 2 diabetes: A systematic review and network meta‐analysis of randomized trials
Liangying Hou, Qi Wang, Bei Pan, Rui Li, Yanfei Li, Juanjuan He, Tianzhu Qin, Liujiao Cao, Na Zhang, Changhao Cao, Long Ge, Kehu Yang
Diabetes/Metabolism Research and Reviews.2023;[Epub] CrossRef - Estimating the Effect of Aerobic Exercise Training on Novel Lipid Biomarkers: A Systematic Review and Multivariate Meta-Analysis of Randomized Controlled Trials
Gina Wood, Emily Taylor, Vanessa Ng, Anna Murrell, Aditya Patil, Tom van der Touw, Mitch Wolden, Nick Andronicos, Neil A. Smart
Sports Medicine.2023; 53(4): 871. CrossRef - 2023 update on Italian guidelines for the treatment of type 2 diabetes
Edoardo Mannucci, Riccardo Candido, Lina delle Monache, Marco Gallo, Andrea Giaccari, Maria Luisa Masini, Angela Mazzone, Gerardo Medea, Basilio Pintaudi, Giovanni Targher, Marina Trento, Giuseppe Turchetti, Valentina Lorenzoni, Matteo Monami
Acta Diabetologica.2023; 60(8): 1119. CrossRef - The Effect of Eight Weeks of Concurrent Training on Serum Levels of Paraxonase-1, Irisin, Lipid Profile, and Insulin Resistance in Men With Metabolic Syndrome
Seyed Amir Hosain Diba Hosaini, Morvarid Vafaee, Bahram Abedi
Hormozgan Medical Journal.2023; 27(1): 43. CrossRef - An Overview of the TRP-Oxidative Stress Axis in Metabolic Syndrome: Insights for Novel Therapeutic Approaches
Mizael C. Araújo, Suzany H. S. Soczek, Jaqueline P. Pontes, Leonardo A. C. Marques, Gabriela S. Santos, Gisele Simão, Laryssa R. Bueno, Daniele Maria-Ferreira, Marcelo N. Muscará, Elizabeth S. Fernandes
Cells.2022; 11(8): 1292. CrossRef - Effect of Yijinjing combined with elastic band exercise on muscle mass and function in middle-aged and elderly patients with prediabetes: A randomized controlled trial
Yunda Huang, Junhua Han, Qing Gu, Yanwei Cai, Jingyuan Li, Shasha Wang, Suijun Wang, Ru Wang, Xiangyun Liu
Frontiers in Medicine.2022;[Epub] CrossRef - Effect of combined aerobic and resistance exercise on blood pressure in postmenopausal women: A systematic review and meta-analysis of randomized controlled trials
Huihui Xi, Yayu He, Yirou Niu, Xin Sui, Jun Zhang, Ruiting Zhu, Haiyan Xu, Shuang Zhang, Yang Li, Yuan Yuan, Lirong Guo
Experimental Gerontology.2021; 155: 111560. CrossRef - Effects of Augmented-Reality-Based Exercise on Muscle Parameters, Physical Performance, and Exercise Self-Efficacy for Older Adults
Sangwan Jeon, Jiyoun Kim
International Journal of Environmental Research and Public Health.2020; 17(9): 3260. CrossRef - Apolipoprotein J is a hepatokine regulating muscle glucose metabolism and insulin sensitivity
Ji A Seo, Min-Cheol Kang, Won-Mo Yang, Won Min Hwang, Sang Soo Kim, Soo Hyun Hong, Jee-In Heo, Achana Vijyakumar, Leandro Pereira de Moura, Aykut Uner, Hu Huang, Seung Hwan Lee, Inês S. Lima, Kyong Soo Park, Min Seon Kim, Yossi Dagon, Thomas E. Willnow, V
Nature Communications.2020;[Epub] CrossRef - Impact of Skeletal Muscle Mass on Metabolic Health
Gyuri Kim, Jae Hyeon Kim
Endocrinology and Metabolism.2020; 35(1): 1. CrossRef - Habitual Combined Exercise Protects against Age-Associated Decline in Vascular Function and Lipid Profiles in Elderly Postmenopausal Women
Elizabeth J. Pekas, John Shin, Won-Mok Son, Ronald J. Headid, Song-Young Park
International Journal of Environmental Research and Public Health.2020; 17(11): 3893. CrossRef

 KDA
KDA PubReader
PubReader Cite
Cite






