- Current
- Browse
- Collections
-
For contributors
- For Authors
- Instructions to authors
- Article processing charge
- e-submission
- For Reviewers
- Instructions for reviewers
- How to become a reviewer
- Best reviewers
- For Readers
- Readership
- Subscription
- Permission guidelines
- About
- Editorial policy
Articles
- Page Path
- HOME > Diabetes Metab J > Volume 40(1); 2016 > Article
-
ReviewObesity and Metabolic Syndrome Brown Fat and Browning for the Treatment of Obesity and Related Metabolic Disorders
- So Hun Kim1, Jorge Plutzky2
-
Diabetes & Metabolism Journal 2016;40(1):12-21.
DOI: https://doi.org/10.4093/dmj.2016.40.1.12
Published online: January 21, 2016
1Division of Endocrinology and Metabolism, Department of Internal Medicine, Inha University School of Medicine, Incheon, Korea.
2Cardiovascular Division, Brigham and Women's Hospital, Harvard Medical School, Boston, MA, USA.
- Corresponding author: Jorge Plutzky. Cardiovascular Division, Brigham and Women's Hospital, Harvard Medical School, 77 Ave Louis Pasteur, NRB 742, Boston, MA 02115, USA. jplutzky@rics.bwh.harvard.edu
Copyright © 2016 Korean Diabetes Association
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/3.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
ABSTRACT
- Brown fat is a specialized fat depot that can increase energy expenditure and produce heat. After the recent discovery of the presence of active brown fat in human adults and novel transcription factors controlling brown adipocyte differentiation, the field of the study of brown fat has gained great interest and is rapidly growing. Brown fat expansion and/or activation results in increased energy expenditure and a negative energy balance in mice and limits weight gain. Brown fat is also able to utilize blood glucose and lipid and results in improved glucose metabolism and blood lipid independent of weight loss. Prolonged cold exposure and beta adrenergic agonists can induce browning of white adipose tissue. The inducible brown adipocyte, beige adipocyte evolving by thermogenic activation of white adipose tissue have different origin and molecular signature from classical brown adipocytes but share the characteristics of high mitochondria content, UCP1 expression and thermogenic capacity when activated. Increasing browning may also be an efficient way to increase whole brown fat activity. Recent human studies have shown possibilities that findings in mice can be reproduced in human, making brown fat a good candidate organ to treat obesity and its related disorders.
- Obesity has increased at an alarming rate worldwide. Since obesity is associated with many diseases, such as type 2 diabetes, insulin resistance, dyslipidemia, hypertension, cardiovascular disease, sleep apnea, and some types of cancer, the rapid increase in obesity is a major health burden [1]. Although there is an epidemic of obesity worldwide the effort to decrease this epidemic has not been effective and there is a growing need of novel therapeutics to prevent and treat obesity [2]. Obesity is thought to be caused by an imbalance between energy intake and energy consumption. Pharmacologic agents currently approved have the effect of mainly decreasing energy intake and there are currently no approved drug that can increase energy consumption.
- Fat tissue had been considered a simple storage organ until the late 1980s. Many lines of evidence subsequently established adipose tissue as an endocrine organ secreting many hormones and cytokines that can influence systemic metabolism [3]. Moreover, recent work has established distinct adipose depots that play specific roles. In contrast to white fat, which mainly stores energy and is increased in obesity, brown fat generates heat (thermogenesis), thus increasing consumption of energy; as such, brown fat and the induction of brown fat-like properties in white fat, has been considered as a target for fighting obesity. Brown fat, also known as brown adipose tissue (BAT) by dissipating energy as heat, has an essential role of maintaining body temperature in rodents and human neonates [4]. In human adults, the existence of BAT was debated, and if present, thought to be a remnant, physiologically non-significant organ until recently. Several groups have shown using fluorodeoxy glucose (FDG)-positron emission tomography (PET) in combination with computed tomography (CT), the presence of brown fat and the association with age, leanness, and environmental temperature with brown fat activity [567]. These studies have made brown fat to be a plausible target organ for the management of obesity and its related diseases in human. By increasing the amount and/or activity of brown fat, energy consumption can be increased, and this will lead to a negative energy balance. The field of basic science has also shown much progress in the understanding of brown fat development and physiology [48]. The finding of an inducible thermogenic adipocyte, the beige (inducible, brite) adipocyte has also been studied extensively.
- In this review, we will review the development and function of brown and beige adipocytes, the role and significance of brown fat and browning in the treatment of obesity and diabetes, and the relevance in humans.
INTRODUCTION
- Brown adipocytes are the major constituents of BAT, occupying the largest area. Traditionally adipocytes have been divided into white adipocytes and brown adipocytes. White adipocytes and brown adipocytes both have fat droplets but these differ in morphology and function. White adipocytes have a unilocular fat droplet, relatively few mitochondria, and mainly store fat. In contrast, brown adipocytes have multilocular fat droplets, a high content of mitochondria, and a high level of expression of uncoupling protein 1 (UCP1) in the inner membrane of mitochondria. UCP1 is a critical player in allowing electrons to be released rather than stored, resulting in heat release. The most important and well-studied factor influencing brown adipocytes is norepinephrine (NE). NE is able to affect activation, cell proliferation and differentiation of brown adipocytes. NE mainly functions through the β-adrenergic receptor, especially the β3-adrenoreceptor. After receptor binding, via adenylyl cyclase activation, cyclic adenosine monophosphate (cAMP) level is increased and protein kinase A (PKA) is activated leading to triglyceride breakdown and release of free fatty acids (FFAs) which are acute substrates for thermogenesis and regulators of the activity of UCP1. PKA can phosphorylate cAMP-response-element-binding (CREB) and p38 mitogen-activated protein kinases (MAPK) which drives a thermogenic transcriptional response including the induction of UCP1 gene expression [4910]. Brown adipocytes can dissipate chemical energy stored as triglycerides by channeling fatty acids into β oxidation when activated. UCP1 is able to uncouple electron transport from adenosine triphosphate (ATP) production and produces heat in brown adipocytes [811].
- Beige adipocytes (also called 'brite,' 'brown-like,' 'inducible brown') are an inducible form of thermogenic adipocytes and have a low UCP1 content in basal conditions but when induced have a high UCP1 expression level and increased energy consumption [412]. The origin and characteristics of classical brown adipocytes and beige adipocytes are different (Table 1). Classical brown adipocytes originate from precursor cells in the embryonic mesoderm that express Myf5 and Pax7 [13]. Beige adipocytes are thought to come from a distinct cell lineage mainly of a Myf5 negative lineage. The origin of beige adipocytes residing in white fat tissue has been a focus of great debate [4]. Some studies have shown that the origin was trans-differentiation from mature white adipocytes [1415] whereas a recent study using a pulse-chase fate-mapping technique, has shown that most of the beige adipocytes arise by de novo differentiation from a precursor population [16]. Beige and white adipocytes arising from the white adipose tissue (WAT) are thought to arise from a different type of precursor cells. Wu et al. [17] has identified two types of preadipocytes (white and beige) using global gene profiling and differentiation analysis. Beige preadipocytes expressed Cd137 and transmembrane protein 26 (Tmem26) on the cell surface and only the adipocytes differentiated from the beige preadipocytes were able to induce a thermogenic gene program with β-adrenergic agonist treatment [17]. Beige adipocytes are most abundant in the subcutaneous depots of rodents [14]. In epididymal WAT of male mice which is a visceral fat depot, beige adipocytes develop from a bipotent precursor that can also differentiate into white adipocytes. These bipotent precursors express platelet-derived growth factor receptor α and represent a subpopulation of stromal cells expressing the common stem cell markers CD34 and Sca-1 [18].
- Master regulators of adipogenesis, peroxisome proliferator-activated receptor γ (PPARγ) and CCAAT/enhancer-binding proteins (C/EBPs), are involved in the differentiation of both white and brown adipocytes [8]. A large zinc finger-containing transcriptional factor, PR domain containing 16 (PRDM 16) plays a major role in the cell fate decision process promoting the development of brown adipocytes from Myf5 expressing precursors [13]. PRDM16 was also able to induce brown fat cells in WAT [19]. PRDM16 stimulates brown adipogenesis by binding to PPARγ coactivator 1α (PGC-1α), PGC-1β, C/EBP-β and PPARγ and activating its transcriptional function [131920].
- BAT, due to its ability to uncouple electron gradients, generate ATP and promote energy dissipation, can be a target for obesity management. In rodents, BAT is found in the interscapular, perirenal, and periaortic regions. In human infants, similar to rodents, BAT depots mainly reside in the interscapular and perirenal area and this depot gradually disappears with increasing age [2122]. Human adults mainly have BAT in the cervical, supraclavicular, axillary and paravertebral areas as demonstrated in studies using 18F-FDG-PET/CT [567]. BAT is composed of brown adipocytes with a high content of the BAT specific mitochondrial protein, UCP1 [23]. UCP1 has no activity in basal states but can be activated by long chain fatty acids generated within the mitochondrial inner membrane [24]. BAT is highly vascularized and densely innervated by the sympathetic nervous system. BAT is activated by cold exposure and is mainly controlled by the sympathetic nervous system. Sympathetic activation of BAT results in increased thermogenic gene expression and recruitment of enzymes needed for uptake, mobilization and oxidation of lipids [23]. The thyroid hormone system also plays a synergistic role and is essential for BAT activation [25]. BAT can also be activated by increasing caloric intake in rodents and this process is termed diet-induced thermogenesis [1126]. This will be of great relevance to the BAT based obesity treatment but this has not yet been confirmed in humans.
BROWN ADIPOCYTES AND BEIGE ADIPOCYTES
- Clusters of thermogenic beige adipocytes can be seen in traditional WAT depots after chronic cold exposure or through the genetic manipulation of specific pathways [27]. Whether white adipocytes can be induced to transdifferentiate into a more brown adipocyte like state remains unresolved. Regardless, both processes are referred to in general as 'browning' of WAT [8]. Chronic treatment with β3-adrenergic receptor activators and thiazolidinediones can also induce the browning process [2829]. Increasing the amount of beige fat may be a valid method to increase the amount of BAT and increase energy consumption. Accordingly, many rodent models have shown that increased browning of the WAT was able to resist diet induced obesity and improve metabolism [430313233]. Recent studies showing that the adult BAT shows characteristics of beige adipocytes reinforces the browning of adipose tissue as an interesting therapeutic possibility [17]. The browning process is regulated by a complex hormonal interplay and many environmental factors such as chronic cold exposure, exercise and environmental enrichment (Table 1) [834].
- Chronic cold exposure
- Cold is sensed by thermoreceptors and leads to a sympathetic outflow to BAT through a neural circuitry [35]. Classically, NE released from the sympathetic nerve terminal activates the BAT thermogenic program via PKA and p38 MAPK signaling and leads to lipolysis and production of FFA for UCP1 activation [34]. Recent studies have elucidated an efferent beige fat thermogenic circuit-consisting of eosinophils, type 2 cytokines interleukin (IL)-4/13, and alternatively activated macrophages-which regulate the development of cold-induced beige fat. Cold exposure induces eosinophil IL-4/13 production and this leads to M2 macrophage activation which induces tyrosine hydroxylase expression and catecholamine production leading to browning of subcutaneous WAT [3637]. Meteorin-like (Metrnl) is a PGC-1α4-regulated hormone that is induced upon exercise and cold exposure promoting browning by inducing IL-4/13 and M2 macrophage activation, which is required for long-term adaptations to cold temperatures [37].
- Exercise
- Exercise has been reported to increase browning of WAT and increase energy expenditure. There is a possibility that this mechanism may be an additional pathway leading to the chronic benefits of exercise training on glucose and lipid metabolism [38]. PGC-1α is induced in the muscle by exercise and stimulates many beneficial effects of exercise in muscle, including mitochondrial biogenesis and muscle fibre-type switching [39]. PGC-1α is able to increase expression of FNDC5 (fibronectin domain-containing 5), a membrane protein that is cleaved and secreted as irisin. Although controversial, irisin has been reported to be induced by exercise in mice and humans and capable of inducing browning of WAT, resulting in improvements in obesity and glucose homeostasis [38]. Metrnl is a myokine induced by resistance exercise and PGC-1α4. Metrnl is able to promote activation of M2 macrophages and catecholamine production from these cells to induce WAT browning [37]. IL-6 is a major myokine induced by exercise and has been reported to play a role in exercise induced WAT browning [40].
- Environmental enrichment
- Living in an enriched environment with complex physical and social stimulation was able to induce browning of WAT in mice. This is mediated by induction of hypothalamic brain-derived neurotropic factor (BDNF) expression, which leads to selective sympathetic nervous system activation of white fat to induce browning and increase energy dissipation. Environmental enrichment was able to resist diet-induced obesity through the browning effect. Hypothalamic overexpression of BDNF was able to reproduce the enrichment-associated activation of browning of WAT and the associated lean phenotype [41].
- Endocrine factors and metabolites
- There are many novel factors and signaling pathways that can induce brown and/or beige. Among these factors fibroblast growth factors 21 (FGF21) [42434445], cardiac natriuretic peptides (NPs) [46], retinaldehyde (Rald) [31], bone morphongenetic proteins (BMPs) [4748] are secreted molecules that can activate BAT and/or induce browning in WAT. FGF21 is an endocrine factor produced in liver, BAT, and skeletal muscle [49]. Cold exposure induces FGF21 gene transcription and FGF21 release in brown adipocytes via cAMP-mediated PKA and p38 MAPK activation [43]. Cold induced increase in plasma FGF21 levels was also observed in humans [50]. FGF21 plays a physiological role in browning of WAT. Adipose-derived FGF21 acts in an autocrine and paracrine manner to increase UCP1 and other thermogenic genes in fat tissues. These processes are in part regulated by enhancing adipose tissue PGC-1α protein levels without affecting mRNA expression. Mice deficient of FGF21 showed an impaired ability to adapt to chronic cold exposure and decreased browning of WAT [45].
- The cardiac NPs, atrial NP (ANP) and its ventricular companion, brain-type NP (BNP) are key hormones in fluid and hemodynamic homeostasis. NPs are expressed in adipose tissue and ANP was shown to increase lipolysis in human adipocytes [51]. Bordicchia et al. [46] showed that NPs promote browning of white adipocytes to increase energy expenditure and increase thermogenic gene expression in BAT. In human adipocytes, ANP and BNP activated PGC-1α and UCP1 expression, induced mitochondriogenesis and increased uncoupled and total respiration. ANP and β-adrenergic receptor agonists additively enhanced expression of brown fat and mitochondrial markers in a p38 MAPK-dependent manner. Mice exposed to cold temperatures had increased levels of circulating NPs and a higher expression of NP signaling receptor in BAT and WAT. Infusion of BNP into mice robustly increased Ucp1 and Pgc-1α expression in WAT and BAT with corresponding elevation of respiration and energy expenditure. NP bind to NP receptor A, whose intracellular domain possesses guanylyl cyclase activity to generate cyclic guanosine monophosphate (cGMP). Activation of guanylyl cyclase and generation of cGMP leads to activation of cGMP-dependent protein kinase (PKG) [46]. PKG works in parallel with the β-adrenergic-PKA pathway to trigger lipolysis and stimulate thermogenesis [4].
- BMPs are members of the transforming growth factor β superfamily of extracellular signaling proteins that influence the differentiation of mesenchymal stem cells. Several BMP members have been shown to play a role in the regulation of adipocyte differentiation and energy expenditure [52]. BMP7 promotes differentiation of brown preadipocytes through induction of PRDM16 and PGC-1α, which are early regulators of brown fat fate. BMP7 can also trigger commitment of mesenchymal progenitor cells to a brown adipocyte lineage. BMP7 knockout embryos show a marked decrease in brown fat and almost complete absence of UCP1. Adenoviral expression of BMP7 in mice results in a significant increase in BAT mass and leads to an increase in energy expenditure and a reduction in weight gain [53]. BMP7 is also able to induce differentiation of Sca-1 positive progenitor cells from muscle and subcutaneous WAT into brown-like adipocytes [47]. BMP4 is expressed at an elevated level in WAT of lean human subjects. Induced expression of BMP4 in WAT induces browning of WAT and increases whole body metabolic rate and insulin sensitivity. PGC-1α mediates the BMP4 induced browning of WAT [48]. BMP8B appears to have both central and peripheral actions. BMP8B is induced by nutritional and thermogenic factors in mature BAT, increasing the response to noradrenaline through enhanced p38MAPK/CREB signaling and increased lipase activity. Central BMP8B treatment increases sympathetic activation of BAT, dependent on the level of AMP-activated protein kinase (AMPK) in the ventromedial nucleus of the hypothalamus. BMP8B null mice show decreased energy expenditure and increased body weight gain. BMP8B is a thermogenic protein that can act centrally with hypothalamic AMPK to regulate energy expenditure [54].
- Retinaldehyde dehydrogenase 1 (Aldh1a1) is the rate-limiting enzyme that converts Rald to retinoic acid. Aldh1a1 is expressed predominately in WAT, with the highest levels found in visceral WAT in mice and humans. Deficiency of the Aldh1a1 in mice induced browning of WAT that drove uncoupled respiration and adaptive thermogenesis, protecting against diet-induced obesity and diabetes [31]. In addition to this phenotype in the knockout mouse, antisense oligonucleotide-mediated Aldh1a1 knockdown in visceral WAT was able to replicate this response, promoting browning of WAT with increased thermogenesis, decreased weight gain and improved glucose homeostasis in high fat diet (HFD) fed mice. These effects seem to be related to increased Rald levels, since Rald was able to induce UCP1 mRNA and protein levels in white adipocytes by selectively activating the retinoic acid receptor, recruiting PGC-1α and inducing UCP1 promoter activity [31].
BROWNING OF ADIPOSE TISSUE
- Increasing BAT amount and/or increasing BAT activity can lead to increased energy expenditure which will be favorable in preventing and managing obesity. Increasing BAT amount and/or activity will also have a direct beneficial effect on glucose and lipid metabolism independent from the effect on body weight (Fig. 1) [55]. Cold exposure can accelerate plasma clearance of triglycerides as a result of increased uptake into BAT in mice. This process is dependent on local lipoprotein lipase activity and transmembrane receptor CD36. In pathophysiological settings of dyslipidemia and insulin resistance, cold exposure corrected hyperlipidemia and improved the deleterious effects of insulin resistance [55]. BAT can clear a substantial portion of total glucose and triglycerides from the circulation when activated. Therefore targeting BAT will have beneficial effects on metabolic disorders related to obesity.
- Evidence of the beneficial effects of increasing brown fat amount can be seen from genetic models of increased BAT [4] and BAT transplantation [56]. BAT transplantation into the visceral cavity in mice resulted in improved glucose tolerance, increased insulin sensitivity, lower body weight, and decreased fat mass. BAT transplantation also resulted in complete reversal of HFD-induced insulin resistance [56]. The beneficial effect of BAT transplantation can also be attributed to secreted factors from the BAT. Another method to increase BAT amount can be increased browning of WAT.
- PGC-1α plays a central role in thermogenic activation of adipocytes. PGC-1α was discovered as a cold-induced interacting partner of PPARγ in brown fat [57]. PGC-1α is a master regulator of mitochondrial biogenesis and oxidative metabolism and in adipocytes, can also induce the expression of UCP1 and other thermogenic components [4]. PGC-1α is essential for cold induced and β-adrenergic agonist induced thermogenic activation of brown adipocytes [58]. PGC-1α expression and activity are regulated directly by the β-adrenergic pathway, linking physiologic activator of brown fat thermogenesis and the transcriptional machinery in brown adipocytes [459]. cAMP and PKA dependent activation of p38 MAPK in brown adipocytes phosphorylates activating transcription factor 2 (ATF-2) and PGC-1α. Activation of ATF-2 by p38 MAPK additionally serves as the cAMP sensor that increases expression of the PGC-1α gene itself in BAT [59].
TARGETING BROWN FAT FOR THE TREATMENT OF OBESITY AND RELATED DISORDERS
- The beneficial effects of BAT have been shown mainly in animal models, leaving unresolved whether thermogenesis might be harnessed in humans. However, the field of the study of human brown fat is emerging rapidly and during recent years, many researchers using sophisticated methods are tackling the issue of the characteristics of human brown fat and its therapeutic possibilities [3460]. Many studies have tried to characterize the human BAT using markers of classical brown adipocytes and beige adipocytes of mice. The interscapular BAT that is seen in human infants show characteristics of classic brown adipocytes [22]. The supraclavicular BAT in adult humans express high levels of beige-adipocyte enriched genes, including T-box transcription factor 1 (Tbx1), Tmem26, Cd137 [17]. On the contrary recent studies have shown that adult BAT express classical brown adipocyte-selective markers, including upregulation of miR260, miR-133b, LIM homeobox protein 8 (Lhx8) and zinc finger protein 1 (Zic1) and down regulation of homeobox C8 (Hoxc8) and homeobox C9 (Hoxc9) [61]. This discrepancy is probably due to the heterogeneity of human BAT and the difference in gene signature according to depth, with deeper depots showing more characteristics of classical brown [62]. Shinoda et al. [63] isolated clonally derived adipocytes from stromal vascular fractions of adult human BAT and globally analyzed their molecular signature and found it resembled those of murine beige adipocytes. Sidossis et al. [64] showed that human subcutaneous WAT undergoes browning and is associated with increased whole-body metabolic rate using burn trauma as a model of prolonged adrenergic stress.
- There have been many clinical studies in human adults that suggest the beneficial effect of activating BAT [34]. Ouellet et al. [65] quantified BAT oxidative metabolism and glucose and nonesterified fatty acid (NEFA) turnover in healthy men under controlled cold exposure conditions. Upon cold exposure, there was increased NEFA and glucose uptake and activation of oxidative metabolism in BAT associated with a 1.8-fold increase in whole-body energy expenditure [65]. Yoneshiro et al. [66] showed that daily 2 hours cold exposure at 17℃ for 6 weeks resulted in increases in BAT activity and cold induced increments of energy expenditure and a concomitant decrease in body fat mass. Chondronikola et al. [67] reported that prolonged cold exposure for 5 to 8 hours was able to increase resting energy expenditure (REE) by 15% in BAT positive men, and plasma glucose (30%) and FFA (70%) contributed to the observed increase in REE. Glucose disposal was increased in BAT and whole-body glucose disposal was significantly increased [67]. In type 2 diabetes subjects, 10 days of cold acclimation increased peripheral insulin sensitivity by 43%. Basal skeletal muscle glucose transporter type 4 (GLUT4) translocation was markedly increased and glucose uptake in skeletal muscle was increased after cold acclimation [68]. In summary, BAT activation through cold exposure was able to increase energy expenditure and have beneficial effects on glucose metabolism supporting its role in treating obesity and related metabolic disorders in humans.
BROWN FAT AND BROWNING IN HUMANS
- The current epidemic of obesity and its related complications like diabetes and heart disease is alarming and underscores the need for novel therapeutics. Targeting BAT and browning of WAT has arisen as a potentially important, efficient strategy to treat obesity and its related metabolic disorders. Increasing the amount and/or activity of theromogenesis will lead to a negative energy balance by increasing energy expenditure; and decrease blood glucose and triglyceride substantially, improving diabetes and dyslipidemia. Many recent human studies have shown that the effects of manipulating brown fat pathways seen in mice are also present in humans. However, more studies are needed to understand the differential physiology and role of brown and beige adipocyte. Understanding their specific mechanism and physiology will enable the development of more safe and efficient therapeutic agents for the treatment of obesity and related metabolic disorders.
CONCLUSIONS
-
Acknowledgements
- This work was supported by a research grant from the Korean Diabetes Association (2010).
ACKNOWLEDGMENTS
-
CONFLICTS OF INTEREST: No potential conflict of interest relevant to this article was reported.
NOTES
- 1. Jensen MD, Ryan DH, Apovian CM, Ard JD, Comuzzie AG, Donato KA, Hu FB, Hubbard VS, Jakicic JM, Kushner RF, Loria CM, Millen BE, Nonas CA, Pi-Sunyer FX, Stevens J, Stevens VJ, Wadden TA, Wolfe BM, Yanovski SZ, Jordan HS, Kendall KA, Lux LJ, Mentor-Marcel R, Morgan LC, Trisolini MG, Wnek J, Anderson JL, Halperin JL, Albert NM, Bozkurt B, Brindis RG, Curtis LH, DeMets D, Hochman JS, Kovacs RJ, Ohman EM, Pressler SJ, Sellke FW, Shen WK, Smith SC Jr, Tomaselli GF. American College of Cardiology/American Heart Association Task Force on Practice Guidelines. Obesity Society. 2013 AHA/ACC/TOS guideline for the management of overweight and obesity in adults: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and The Obesity Society. Circulation 2014;129(25 Suppl 2):S102-S138. PubMed
- 2. Apovian CM, Aronne LJ, Bessesen DH, McDonnell ME, Murad MH, Pagotto U, Ryan DH, Still CD. Endocrine Society. Pharmacological management of obesity: an endocrine Society clinical practice guideline. J Clin Endocrinol Metab 2015;100:342-362. ArticlePubMed
- 3. Kershaw EE, Flier JS. Adipose tissue as an endocrine organ. J Clin Endocrinol Metab 2004;89:2548-2556. ArticlePubMed
- 4. Harms M, Seale P. Brown and beige fat: development, function and therapeutic potential. Nat Med 2013;19:1252-1263. ArticlePubMedPDF
- 5. Cypess AM, Lehman S, Williams G, Tal I, Rodman D, Goldfine AB, Kuo FC, Palmer EL, Tseng YH, Doria A, Kolodny GM, Kahn CR. Identification and importance of brown adipose tissue in adult humans. N Engl J Med 2009;360:1509-1517. ArticlePubMedPMC
- 6. van Marken Lichtenbelt WD, Vanhommerig JW, Smulders NM, Drossaerts JM, Kemerink GJ, Bouvy ND, Schrauwen P, Teule GJ. Cold-activated brown adipose tissue in healthy men. N Engl J Med 2009;360:1500-1508. ArticlePubMed
- 7. Virtanen KA, Lidell ME, Orava J, Heglind M, Westergren R, Niemi T, Taittonen M, Laine J, Savisto NJ, Enerback S, Nuutila P. Functional brown adipose tissue in healthy adults. N Engl J Med 2009;360:1518-1525. ArticlePubMed
- 8. Bartelt A, Heeren J. Adipose tissue browning and metabolic health. Nat Rev Endocrinol 2014;10:24-36. ArticlePubMedPDF
- 9. Cao W, Medvedev AV, Daniel KW, Collins S. Beta-adrenergic activation of p38 MAP kinase in adipocytes: cAMP induction of the uncoupling protein 1 (UCP1) gene requires p38 MAP kinase. J Biol Chem 2001;276:27077-27082. PubMed
- 10. Thonberg H, Fredriksson JM, Nedergaard J, Cannon B. A novel pathway for adrenergic stimulation of cAMP-response-element-binding protein (CREB) phosphorylation: mediation via alpha1-adrenoceptors and protein kinase C activation. Biochem J 2002;364(Pt 1):73-79. PubMedPMC
- 11. Cannon B, Nedergaard J. Brown adipose tissue: function and physiological significance. Physiol Rev 2004;84:277-359. ArticlePubMed
- 12. Giralt M, Villarroya F. White, brown, beige/brite: different adipose cells for different functions. Endocrinology 2013;154:2992-3000. ArticlePubMedPDF
- 13. Seale P, Bjork B, Yang W, Kajimura S, Chin S, Kuang S, Scime A, Devarakonda S, Conroe HM, Erdjument-Bromage H, Tempst P, Rudnicki MA, Beier DR, Spiegelman BM. PRDM16 controls a brown fat/skeletal muscle switch. Nature 2008;454:961-967. ArticlePubMedPMCPDF
- 14. Vitali A, Murano I, Zingaretti MC, Frontini A, Ricquier D, Cinti S. The adipose organ of obesity-prone C57BL/6J mice is composed of mixed white and brown adipocytes. J Lipid Res 2012;53:619-629. ArticlePubMedPMC
- 15. Himms-Hagen J, Melnyk A, Zingaretti MC, Ceresi E, Barbatelli G, Cinti S. Multilocular fat cells in WAT of CL-316243-treated rats derive directly from white adipocytes. Am J Physiol Cell Physiol 2000;279:C670-C681. ArticlePubMed
- 16. Wang QA, Tao C, Gupta RK, Scherer PE. Tracking adipogenesis during white adipose tissue development, expansion and regeneration. Nat Med 2013;19:1338-1344. ArticlePubMedPMCPDF
- 17. Wu J, Bostrom P, Sparks LM, Ye L, Choi JH, Giang AH, Khandekar M, Virtanen KA, Nuutila P, Schaart G, Huang K, Tu H, van Marken Lichtenbelt WD, Hoeks J, Enerback S, Schrauwen P, Spiegelman BM. Beige adipocytes are a distinct type of thermogenic fat cell in mouse and human. Cell 2012;150:366-376. ArticlePubMedPMC
- 18. Lee YH, Petkova AP, Mottillo EP, Granneman JG. In vivo identification of bipotential adipocyte progenitors recruited by beta3-adrenoceptor activation and high-fat feeding. Cell Metab 2012;15:480-491. PubMedPMC
- 19. Seale P, Kajimura S, Yang W, Chin S, Rohas LM, Uldry M, Tavernier G, Langin D, Spiegelman BM. Transcriptional control of brown fat determination by PRDM16. Cell Metab 2007;6:38-54. ArticlePubMedPMC
- 20. Kajimura S, Seale P, Kubota K, Lunsford E, Frangioni JV, Gygi SP, Spiegelman BM. Initiation of myoblast to brown fat switch by a PRDM16-C/EBP-beta transcriptional complex. Nature 2009;460:1154-1158. ArticlePubMedPMCPDF
- 21. Heaton JM. The distribution of brown adipose tissue in the human. J Anat 1972;112(Pt 1):35-39. PubMedPMC
- 22. Lidell ME, Betz MJ, Dahlqvist Leinhard O, Heglind M, Elander L, Slawik M, Mussack T, Nilsson D, Romu T, Nuutila P, Virtanen KA, Beuschlein F, Persson A, Borga M, Enerback S. Evidence for two types of brown adipose tissue in humans. Nat Med 2013;19:631-634. ArticlePubMedPDF
- 23. Townsend KL, Tseng YH. Brown fat fuel utilization and thermogenesis. Trends Endocrinol Metab 2014;25:168-177. ArticlePubMedPMC
- 24. Fedorenko A, Lishko PV, Kirichok Y. Mechanism of fatty-acid-dependent UCP1 uncoupling in brown fat mitochondria. Cell 2012;151:400-413. ArticlePubMedPMC
- 25. Whittle A, Relat-Pardo J, Vidal-Puig A. Pharmacological strategies for targeting BAT thermogenesis. Trends Pharmacol Sci 2013;34:347-355. ArticlePubMed
- 26. Feldmann HM, Golozoubova V, Cannon B, Nedergaard J. UCP1 ablation induces obesity and abolishes diet-induced thermogenesis in mice exempt from thermal stress by living at thermoneutrality. Cell Metab 2009;9:203-209. ArticlePubMed
- 27. Young P, Arch JR, Ashwell M. Brown adipose tissue in the parametrial fat pad of the mouse. FEBS Lett 1984;167:10-14. ArticlePubMedPDF
- 28. Cousin B, Cinti S, Morroni M, Raimbault S, Ricquier D, Penicaud L, Casteilla L. Occurrence of brown adipocytes in rat white adipose tissue: molecular and morphological characterization. J Cell Sci 1992;103(Pt 4):931-942. ArticlePubMedPDF
- 29. Petrovic N, Walden TB, Shabalina IG, Timmons JA, Cannon B, Nedergaard J. Chronic peroxisome proliferator-activated receptor gamma (PPARgamma) activation of epididymally derived white adipocyte cultures reveals a population of thermogenically competent, UCP1-containing adipocytes molecularly distinct from classic brown adipocytes. J Biol Chem 2010;285:7153-7164. PubMed
- 30. Vegiopoulos A, Muller-Decker K, Strzoda D, Schmitt I, Chichelnitskiy E, Ostertag A, Berriel Diaz M, Rozman J, Hrabe de Angelis M, Nusing RM, Meyer CW, Wahli W, Klingenspor M, Herzig S. Cyclooxygenase-2 controls energy homeostasis in mice by de novo recruitment of brown adipocytes. Science 2010;328:1158-1161. ArticlePubMed
- 31. Kiefer FW, Vernochet C, O'Brien P, Spoerl S, Brown JD, Nallamshetty S, Zeyda M, Stulnig TM, Cohen DE, Kahn CR, Plutzky J. Retinaldehyde dehydrogenase 1 regulates a thermogenic program in white adipose tissue. Nat Med 2012;18:918-925. ArticlePubMedPMCPDF
- 32. Seale P, Conroe HM, Estall J, Kajimura S, Frontini A, Ishibashi J, Cohen P, Cinti S, Spiegelman BM. Prdm16 determines the thermogenic program of subcutaneous white adipose tissue in mice. J Clin Invest 2011;121:96-105. ArticlePubMed
- 33. Ye L, Kleiner S, Wu J, Sah R, Gupta RK, Banks AS, Cohen P, Khandekar MJ, Bostrom P, Mepani RJ, Laznik D, Kamenecka TM, Song X, Liedtke W, Mootha VK, Puigserver P, Griffin PR, Clapham DE, Spiegelman BM. TRPV4 is a regulator of adipose oxidative metabolism, inflammation, and energy homeostasis. Cell 2012;151:96-110. ArticlePubMedPMC
- 34. Sidossis L, Kajimura S. Brown and beige fat in humans: thermogenic adipocytes that control energy and glucose homeostasis. J Clin Invest 2015;125:478-486. ArticlePubMedPMC
- 35. Morrison SF, Madden CJ, Tupone D. Central control of brown adipose tissue thermogenesis. Front Endocrinol (Lausanne) 2012;3:pii00005.Article
- 36. Qiu Y, Nguyen KD, Odegaard JI, Cui X, Tian X, Locksley RM, Palmiter RD, Chawla A. Eosinophils and type 2 cytokine signaling in macrophages orchestrate development of functional beige fat. Cell 2014;157:1292-1308. ArticlePubMedPMC
- 37. Rao RR, Long JZ, White JP, Svensson KJ, Lou J, Lokurkar I, Jedrychowski MP, Ruas JL, Wrann CD, Lo JC, Camera DM, Lachey J, Gygi S, Seehra J, Hawley JA, Spiegelman BM. Meteorin-like is a hormone that regulates immune-adipose interactions to increase beige fat thermogenesis. Cell 2014;157:1279-1291. ArticlePubMedPMC
- 38. Bostrom P, Wu J, Jedrychowski MP, Korde A, Ye L, Lo JC, Rasbach KA, Bostrom EA, Choi JH, Long JZ, Kajimura S, Zingaretti MC, Vind BF, Tu H, Cinti S, Hojlund K, Gygi SP, Spiegelman BM. A PGC1-alpha-dependent myokine that drives brown-fat-like development of white fat and thermogenesis. Nature 2012;481:463-468. ArticlePubMedPMCPDF
- 39. Handschin C, Spiegelman BM. The role of exercise and PGC1alpha in inflammation and chronic disease. Nature 2008;454:463-469. ArticlePubMedPMCPDF
- 40. Knudsen JG, Murholm M, Carey AL, Bienso RS, Basse AL, Allen TL, Hidalgo J, Kingwell BA, Febbraio MA, Hansen JB, Pilegaard H. Role of IL-6 in exercise training- and cold-induced UCP1 expression in subcutaneous white adipose tissue. PLoS One 2014;9:e84910ArticlePubMedPMC
- 41. Cao L, Choi EY, Liu X, Martin A, Wang C, Xu X, During MJ. White to brown fat phenotypic switch induced by genetic and environmental activation of a hypothalamic-adipocyte axis. Cell Metab 2011;14:324-338. ArticlePubMedPMC
- 42. Chartoumpekis DV, Habeos IG, Ziros PG, Psyrogiannis AI, Kyriazopoulou VE, Papavassiliou AG. Brown adipose tissue responds to cold and adrenergic stimulation by induction of FGF21. Mol Med 2011;17:736-740. ArticlePubMedPMCPDF
- 43. Hondares E, Iglesias R, Giralt A, Gonzalez FJ, Giralt M, Mampel T, Villarroya F. Thermogenic activation induces FGF21 expression and release in brown adipose tissue. J Biol Chem 2011;286:12983-12990. ArticlePubMedPMC
- 44. Coskun T, Bina HA, Schneider MA, Dunbar JD, Hu CC, Chen Y, Moller DE, Kharitonenkov A. Fibroblast growth factor 21 corrects obesity in mice. Endocrinology 2008;149:6018-6027. ArticlePubMedPDF
- 45. Fisher FM, Kleiner S, Douris N, Fox EC, Mepani RJ, Verdeguer F, Wu J, Kharitonenkov A, Flier JS, Maratos-Flier E, Spiegelman BM. FGF21 regulates PGC-1alpha and browning of white adipose tissues in adaptive thermogenesis. Genes Dev 2012;26:271-281. ArticlePubMedPMC
- 46. Bordicchia M, Liu D, Amri EZ, Ailhaud G, Dessi-Fulgheri P, Zhang C, Takahashi N, Sarzani R, Collins S. Cardiac natriuretic peptides act via p38 MAPK to induce the brown fat thermogenic program in mouse and human adipocytes. J Clin Invest 2012;122:1022-1036. ArticlePubMedPMC
- 47. Schulz TJ, Huang TL, Tran TT, Zhang H, Townsend KL, Shadrach JL, Cerletti M, McDougall LE, Giorgadze N, Tchkonia T, Schrier D, Falb D, Kirkland JL, Wagers AJ, Tseng YH. Identification of inducible brown adipocyte progenitors residing in skeletal muscle and white fat. Proc Natl Acad Sci U S A 2011;108:143-148. ArticlePubMed
- 48. Qian SW, Tang Y, Li X, Liu Y, Zhang YY, Huang HY, Xue RD, Yu HY, Guo L, Gao HD, Liu Y, Sun X, Li YM, Jia WP, Tang QQ. BMP4-mediated brown fat-like changes in white adipose tissue alter glucose and energy homeostasis. Proc Natl Acad Sci U S A 2013;110:E798-E807. ArticlePubMedPMC
- 49. Wang GX, Zhao XY, Lin JD. The brown fat secretome: metabolic functions beyond thermogenesis. Trends Endocrinol Metab 2015;26:231-237. ArticlePubMedPMC
- 50. Lee P, Linderman JD, Smith S, Brychta RJ, Wang J, Idelson C, Perron RM, Werner CD, Phan GQ, Kammula US, Kebebew E, Pacak K, Chen KY, Celi FS. Irisin and FGF21 are cold-induced endocrine activators of brown fat function in humans. Cell Metab 2014;19:302-309. ArticlePubMedPMC
- 51. Sengenes C, Berlan M, De Glisezinski I, Lafontan M, Galitzky J. Natriuretic peptides: a new lipolytic pathway in human adipocytes. FASEB J 2000;14:1345-1351. ArticlePubMedPDF
- 52. Zamani N, Brown CW. Emerging roles for the transforming growth factor-{beta} superfamily in regulating adiposity and energy expenditure. Endocr Rev 2011;32:387-403. PubMed
- 53. Tseng YH, Kokkotou E, Schulz TJ, Huang TL, Winnay JN, Taniguchi CM, Tran TT, Suzuki R, Espinoza DO, Yamamoto Y, Ahrens MJ, Dudley AT, Norris AW, Kulkarni RN, Kahn CR. New role of bone morphogenetic protein 7 in brown adipogenesis and energy expenditure. Nature 2008;454:1000-1004. ArticlePubMedPMCPDF
- 54. Whittle AJ, Carobbio S, Martins L, Slawik M, Hondares E, Vazquez MJ, Morgan D, Csikasz RI, Gallego R, Rodriguez-Cuenca S, Dale M, Virtue S, Villarroya F, Cannon B, Rahmouni K, Lopez M, Vidal-Puig A. BMP8B increases brown adipose tissue thermogenesis through both central and peripheral actions. Cell 2012;149:871-885. ArticlePubMedPMC
- 55. Bartelt A, Bruns OT, Reimer R, Hohenberg H, Ittrich H, Peldschus K, Kaul MG, Tromsdorf UI, Weller H, Waurisch C, Eychmuller A, Gordts PL, Rinninger F, Bruegelmann K, Freund B, Nielsen P, Merkel M, Heeren J. Brown adipose tissue activity controls triglyceride clearance. Nat Med 2011;17:200-205. ArticlePubMedPDF
- 56. Stanford KI, Middelbeek RJ, Townsend KL, An D, Nygaard EB, Hitchcox KM, Markan KR, Nakano K, Hirshman MF, Tseng YH, Goodyear LJ. Brown adipose tissue regulates glucose homeostasis and insulin sensitivity. J Clin Invest 2013;123:215-223. ArticlePubMed
- 57. Puigserver P, Wu Z, Park CW, Graves R, Wright M, Spiegelman BM. A cold-inducible coactivator of nuclear receptors linked to adaptive thermogenesis. Cell 1998;92:829-839. ArticlePubMed
- 58. Uldry M, Yang W, St-Pierre J, Lin J, Seale P, Spiegelman BM. Complementary action of the PGC-1 coactivators in mitochondrial biogenesis and brown fat differentiation. Cell Metab 2006;3:333-341. ArticlePubMed
- 59. Cao W, Daniel KW, Robidoux J, Puigserver P, Medvedev AV, Bai X, Floering LM, Spiegelman BM, Collins S. p38 mitogen-activated protein kinase is the central regulator of cyclic AMP-dependent transcription of the brown fat uncoupling protein 1 gene. Mol Cell Biol 2004;24:3057-3067. ArticlePubMedPMCPDF
- 60. Celi FS, Le TN, Ni B. Physiology and relevance of human adaptive thermogenesis response. Trends Endocrinol Metab 2015;26:238-247. ArticlePubMed
- 61. Jespersen NZ, Larsen TJ, Peijs L, Daugaard S, Homoe P, Loft A, de Jong J, Mathur N, Cannon B, Nedergaard J, Pedersen BK, Moller K, Scheele C. A classical brown adipose tissue mRNA signature partly overlaps with brite in the supraclavicular region of adult humans. Cell Metab 2013;17:798-805. ArticlePubMed
- 62. Cypess AM, White AP, Vernochet C, Schulz TJ, Xue R, Sass CA, Huang TL, Roberts-Toler C, Weiner LS, Sze C, Chacko AT, Deschamps LN, Herder LM, Truchan N, Glasgow AL, Holman AR, Gavrila A, Hasselgren PO, Mori MA, Molla M, Tseng YH. Anatomical localization, gene expression profiling and functional characterization of adult human neck brown fat. Nat Med 2013;19:635-639. ArticlePubMedPMCPDF
- 63. Shinoda K, Luijten IH, Hasegawa Y, Hong H, Sonne SB, Kim M, Xue R, Chondronikola M, Cypess AM, Tseng YH, Nedergaard J, Sidossis LS, Kajimura S. Genetic and functional characterization of clonally derived adult human brown adipocytes. Nat Med 2015;21:389-394. ArticlePubMedPMCPDF
- 64. Sidossis LS, Porter C, Saraf MK, Borsheim E, Radhakrishnan RS, Chao T, Ali A, Chondronikola M, Mlcak R, Finnerty CC, Hawkins HK, Toliver-Kinsky T, Herndon DN. Browning of subcutaneous white adipose tissue in humans after severe adrenergic stress. Cell Metab 2015;22:219-227. ArticlePubMedPMC
- 65. Ouellet V, Labbe SM, Blondin DP, Phoenix S, Guerin B, Haman F, Turcotte EE, Richard D, Carpentier AC. Brown adipose tissue oxidative metabolism contributes to energy expenditure during acute cold exposure in humans. J Clin Invest 2012;122:545-552. ArticlePubMedPMC
- 66. Yoneshiro T, Aita S, Matsushita M, Kayahara T, Kameya T, Kawai Y, Iwanaga T, Saito M. Recruited brown adipose tissue as an antiobesity agent in humans. J Clin Invest 2013;123:3404-3408. ArticlePubMedPMC
- 67. Chondronikola M, Volpi E, Borsheim E, Porter C, Annamalai P, Enerback S, Lidell ME, Saraf MK, Labbe SM, Hurren NM, Yfanti C, Chao T, Andersen CR, Cesani F, Hawkins H, Sidossis LS. Brown adipose tissue improves whole-body glucose homeostasis and insulin sensitivity in humans. Diabetes 2014;63:4089-4099. ArticlePubMedPMCPDF
- 68. Hanssen MJ, Hoeks J, Brans B, van der Lans AA, Schaart G, van den Driessche JJ, Jorgensen JA, Boekschoten MV, Hesselink MK, Havekes B, Kersten S, Mottaghy FM, van Marken Lichtenbelt WD, Schrauwen P. Short-term cold acclimation improves insulin sensitivity in patients with type 2 diabetes mellitus. Nat Med 2015;21:863-865. ArticlePubMedPDF
REFERENCES
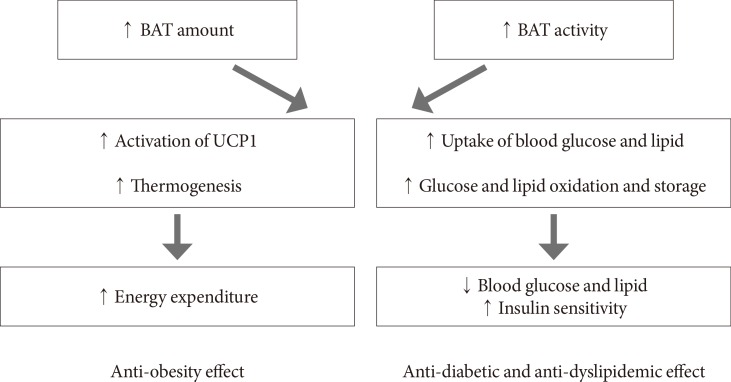
Brown adipose tissue (BAT) targeted treatment of obesity and related metabolic disorders. Increasing BAT amount and/or BAT activity leads to increased activation of uncoupling protein 1 (UCP1) and thermogenesis leading to energy expenditure which will have anti-obesity effects. On the other hand, BAT can also increase the uptake of blood glucose and lipid. Glucose and fatty acids are oxidized or stored as glycogen or triglyceride. This results in decrease in blood glucose and lipid and increase in insulin sensitivity, leading to anti-diabetic and anti-dyslipidemic effects.

Characteristics of brown and beige adipocytes
Lhx8, LIM homeobox protein 8; Zic1, zinc finger protein 1; Tmem26, transmembrane protein 26; Tbx1, T-box transcription factor 1; FGF21, fibroblast growth factor 21; ANP, atrial natriuretic peptide; BNP, brain-type natriuretic peptide; BMP, bone morphogenetic protein; BDNF, brain-derived neurotropic factor.
Figure & Data
References
Citations

- Modulation of angiogenic switch in reprogramming browning and lipid metabolism in white adipocytes
Sreelekshmi Sreekumar, Karyath Palliyath Gangaraj, Manikantan Syamala Kiran
Biochimica et Biophysica Acta (BBA) - Molecular and Cell Biology of Lipids.2024; 1869(1): 159423. CrossRef - Anti-Obesity Effects of GABA in C57BL/6J Mice with High-Fat Diet-Induced Obesity and 3T3-L1 Adipocytes
Heegu Jin, Hyein Han, Gunju Song, Hyun-Ji Oh, Boo-Yong Lee
International Journal of Molecular Sciences.2024; 25(2): 995. CrossRef - Citrus aurantium L. and synephrine improve brown adipose tissue function in adolescent mice programmed by early postnatal overfeeding
Andressa Cardoso Guimarães, Egberto Gaspar de Moura, Stephanie Giannini Silva, Bruna Pereira Lopes, Iala Milene Bertasso, Carla Bruna Pietrobon, Fernanda Torres Quitete, Tayanne de Oliveira Malafaia, Érica Patrícia Garcia Souza, Patrícia Cristina Lisboa,
Frontiers in Nutrition.2024;[Epub] CrossRef - Au@16-pH-16/miR-21 mimic nanosystem: An efficient treatment for obesity through browning and thermogenesis induction
Said Lhamyani, Adriana-Mariel Gentile, María Mengual-Mesa, Elia Grueso, Rosa M. Giráldez-Pérez, José Carlos Fernandez-Garcia, Antonio Vega-Rioja, Mercedes Clemente-Postigo, John R. Pearson, Isabel González-Mariscal, Gabriel Olveira, Francisco-Javier Bermu
Biomedicine & Pharmacotherapy.2024; 171: 116104. CrossRef - Walnut supplementation increases levels of UCP1 and CD36 in brown adipose tissue independently of diet type
Tamara Dakic, Dusan Jeremic, Iva Lakic, Nebojsa Jasnic, Aleksandra Ruzicic, Predrag Vujovic, Tanja Jevdjovic
Molecular and Cellular Biochemistry.2024;[Epub] CrossRef - A Newly Synbiotic Combination Alleviates Obesity by Modulating the Gut Microbiota–Fat Axis and Inhibiting the Hepatic TLR4/NF‐κB Signaling Pathway
Yongbo Kang, Peng Ren, Xiaorong Shen, Xiaoyu Kuang, Xiaodan Yang, Haixia Liu, Huan Yan, Hao Yang, Xing Kang, Zeyuan Ding, Xuguang Luo, Jieqiong Ma, Ying Yang, Weiping Fan
Molecular Nutrition & Food Research.2023;[Epub] CrossRef - Lacticaseibacillus paracasei AO356 ameliorates obesity by regulating adipogenesis and thermogenesis in C57BL/6J male mice
Young In Kim, Eun-Sook Lee, Eun-Ji Song, Dong-Uk Shin, Ji-Eun Eom, Hee Soon Shin, Jung Eun Kim, Ju Yeoun Oh, Young-Do Nam, So-Young Lee
Journal of Functional Foods.2023; 101: 105404. CrossRef - Effects of caffeoylquinic acid analogs derived from aerial parts of Artemisia iwayomogi on adipogenesis
Su-Young Han, Jisu Kim, Bo Kyeong Kim, Wan Kyunn Whang, Hyeyoung Min
Food Science and Biotechnology.2023; 32(9): 1215. CrossRef - Anti-obesity effects of Lactiplantibacillus plantarum SKO-001 in high-fat diet-induced obese mice
Mi Jin Choi, Hana Yu, Jea Il Kim, Hee Seo, Ju Gyeong Kim, Seul-Ki Kim, Hak Sung Lee, Hyae Gyeong Cheon
European Journal of Nutrition.2023; 62(4): 1611. CrossRef - Meteorin-like Protein and Asprosin Levels in Children and Adolescents with Obesity and Their Relationship with Insulin Resistance and Metabolic Syndrome
Nariman Moradi, Reza Fadaei, Maryam Roozbehkia, Mitra Nourbakhsh, Mona Nourbakhsh, Maryam Razzaghy-Azar, Bagher Larijani
Laboratory Medicine.2023; 54(5): 457. CrossRef - A Novel Mix of Polyphenols and Micronutrients Reduces Adipogenesis and Promotes White Adipose Tissue Browning via UCP1 Expression and AMPK Activation
Francesca Pacifici, Gina Malatesta, Caterina Mammi, Donatella Pastore, Vincenzo Marzolla, Camillo Ricordi, Francesca Chiereghin, Marco Infante, Giulia Donadel, Francesco Curcio, Annalisa Noce, Valentina Rovella, Davide Lauro, Manfredi Tesauro, Nicola Di D
Cells.2023; 12(5): 714. CrossRef - Thromboxane A2-TP axis promotes adipose tissue macrophages M1 polarization leading to insulin resistance in obesity
Ruijie Xu, Yufeng Dai, Xu Zheng, Yongheng Yan, Zhao He, Hao Zhang, Haitao Li, Wei Chen
Biochemical Pharmacology.2023; 210: 115465. CrossRef - Green Tea Epigallocatechin Gallate Inhibits Preadipocyte Growth via the microRNA‐let‐7a/HMGA2 Signaling Pathway
Wen‐Ting Chen, Meei‐Ju Yang, Yi‐Wei Tsuei, Tsung‐Chen Su, An‐Ci Siao, Yow‐Chii Kuo, Ling‐Ru Huang, Yi Chen, Sy‐Jou Chen, Po‐Chuan Chen, Ching‐Feng Cheng, Hui‐Chen Ku, Yung‐Hsi Kao
Molecular Nutrition & Food Research.2023;[Epub] CrossRef - Current Role and Potential of Polymeric Biomaterials in Clinical Obesity Treatment
Rui-Chian Tang, I-Hsuan Yang, Feng-Huei Lin
Biomacromolecules.2023; 24(8): 3438. CrossRef - Short-duration cold exposure decreases fasting-induced glucose intolerance but has no effect on resting energy expenditure
Rima Solianik, Katerina Židonienė, Marius Brazaitis
Cryobiology.2023; 113: 104564. CrossRef - Caffeine promotes the production of Irisin in muscles and thus facilitates the browning of white adipose tissue
Chang Liu, Yi Li, Ge Song, Xuehan Li, Songyue Chen, Dixin Zou, Huixin Li, Chengyi Hu, Haotian Zhao, Yi Yan
Journal of Functional Foods.2023; 108: 105702. CrossRef - Thermogenic Modulation of Adipose Depots: A Perspective on Possible Therapeutic Intervention with Early Cardiorenal Complications of Metabolic Impairment
Ahmed F. El-Yazbi, Mohamed A. Elrewiny, Hosam M. Habib, Ali H. Eid, Perihan A. Elzahhar, Ahmed S.F. Belal
Molecular Pharmacology.2023; 104(5): 187. CrossRef - Rabbit Meat Extract Induces Browning in 3T3−L1 Adipocytes via the AMP−Activated Protein Kinase Pathway
In-Seon Bae, Jeong Ah Lee, Soo-Hyun Cho, Hyoun-Wook Kim, Yunseok Kim, Kangmin Seo, Hyun-Woo Cho, Min Young Lee, Ju Lan Chun, Ki Hyun Kim
Foods.2023; 12(19): 3671. CrossRef - Metabolic-Dysfunction-Associated Steatotic Liver Disease—Its Pathophysiology, Association with Atherosclerosis and Cardiovascular Disease, and Treatments
Hidekatsu Yanai, Hiroki Adachi, Mariko Hakoshima, Sakura Iida, Hisayuki Katsuyama
International Journal of Molecular Sciences.2023; 24(20): 15473. CrossRef - Brown Fat and Nutrition: Implications for Nutritional Interventions
Lloyd Noriega, Cheng-Ying Yang, Chih-Hao Wang
Nutrients.2023; 15(18): 4072. CrossRef - Metabolic Syndrome: A Narrative Review from the Oxidative Stress to the Management of Related Diseases
Giovanni Martemucci, Giuseppe Fracchiolla, Marilena Muraglia, Roberta Tardugno, Roberta Savina Dibenedetto, Angela Gabriella D’Alessandro
Antioxidants.2023; 12(12): 2091. CrossRef - Metabolic responses of light and taste receptors – unexpected actions of GPCRs in adipocytes
Onyinye Nuella Ekechukwu, Mark Christian
Reviews in Endocrine and Metabolic Disorders.2022; 23(1): 111. CrossRef - The ATF3 inducer protects against diet-induced obesity via suppressing adipocyte adipogenesis and promoting lipolysis and browning
Hui-Chen Ku, Tsai-Yun Chan, Jia-Fang Chung, Yung-Hsi Kao, Ching-Feng Cheng
Biomedicine & Pharmacotherapy.2022; 145: 112440. CrossRef - Prednisone stimulates white adipocyte browning via β3-AR/p38 MAPK/ERK signaling pathway
Sulagna Mukherjee, Jong Won Yun
Life Sciences.2022; 288: 120204. CrossRef - Tangeretin prevents obesity by modulating systemic inflammation, fat browning, and gut microbiota in high-fat diet-induced obese C57BL/6 mice
Qiyang Chen, Dan Wang, Yue Gu, Zixiao Jiang, Zhiqin Zhou
The Journal of Nutritional Biochemistry.2022; 101: 108943. CrossRef - Evaluation of thermal sensitivity is of potential clinical utility for the predictive, preventive, and personalized approach advancing metabolic syndrome management
Sujeong Mun, Kihyun Park, Siwoo Lee
EPMA Journal.2022; 13(1): 125. CrossRef - Effects of a Novel Selective Peroxisome Proliferator-Activated Receptor α Modulator, Pemafibrate, on Metabolic Parameters: A Retrospective Longitudinal Study
Hidekatsu Yanai, Hisayuki Katsuyama, Mariko Hakoshima
Biomedicines.2022; 10(2): 401. CrossRef - Historical and cultural aspects of obesity: From a symbol of wealth and prosperity to the epidemic of the 21st century
Marta Sumińska, Rafał Podgórski, Klaudia Bogusz‐Górna, Bogda Skowrońska, Artur Mazur, Marta Fichna
Obesity Reviews.2022;[Epub] CrossRef - Molecular Biological and Clinical Understanding of the Statin Residual Cardiovascular Disease Risk and Peroxisome Proliferator-Activated Receptor Alpha Agonists and Ezetimibe for Its Treatment
Hidekatsu Yanai, Hiroki Adachi, Mariko Hakoshima, Hisayuki Katsuyama
International Journal of Molecular Sciences.2022; 23(7): 3418. CrossRef - Pep19 Has a Positive Effect on Insulin Sensitivity and Ameliorates Both Hepatic and Adipose Tissue Phenotype of Diet-Induced Obese Mice
Renata Silvério, Robson Barth, Andrea S. Heimann, Patrícia Reckziegel, Gustavo J. dos Santos, Silvana Y. Romero-Zerbo, Francisco J. Bermúdez-Silva, Alex Rafacho, Emer S. Ferro
International Journal of Molecular Sciences.2022; 23(8): 4082. CrossRef - Thermogenic T cells: a cell therapy for obesity?
Ulf H. Beier, Daniel J. Baker, Joseph A. Baur
American Journal of Physiology-Cell Physiology.2022; 322(6): C1085. CrossRef - Accumulation of γδ T cells in visceral fat with aging promotes chronic inflammation
Maria E. C. Bruno, Sujata Mukherjee, Whitney L. Powell, Stephanie F. Mori, Franklyn K. Wallace, Beverly K. Balasuriya, Leon C. Su, Arnold J. Stromberg, Donald A. Cohen, Marlene E. Starr
GeroScience.2022; 44(3): 1761. CrossRef - Deletion of GPR30 Drives the Activation of Mitochondrial Uncoupling Respiration to Induce Adipose Thermogenesis in Female Mice
Jing Luo, Yao Wang, Elizabeth Gilbert, Dongmin Liu
Frontiers in Endocrinology.2022;[Epub] CrossRef - Inhibition of STAT3 enhances UCP1 expression and mitochondrial function in brown adipocytes
Lini Song, Xi Cao, Wenyi Ji, Lili Zhao, Weili Yang, Ming Lu, Jinkui Yang
European Journal of Pharmacology.2022; 926: 175040. CrossRef - TRPC5 deletion in the central amygdala antagonizes high-fat diet-induced obesity by increasing sympathetic innervation
Huan Ma, Chengkang He, Li Li, Peng Gao, Zongshi Lu, Yingru Hu, Lijuan Wang, Yu Zhao, Tingbing Cao, Yuanting Cui, Hongting Zheng, Gangyi Yang, Zhencheng Yan, Daoyan Liu, Zhiming Zhu
International Journal of Obesity.2022; 46(8): 1544. CrossRef - Adapalene induces adipose browning through the RARβ-p38 MAPK-ATF2 pathway
Na Hyun Lee, Mi Jin Choi, Hana Yu, Jea Il Kim, Hyae Gyeong Cheon
Archives of Pharmacal Research.2022; 45(5): 340. CrossRef - Engineering Functional Vascularized Beige Adipose Tissue from Microvascular Fragments of Models of Healthy and Type II Diabetes Conditions
Francisca M. Acosta, Katerina Stojkova, Jingruo Zhang, Eric Ivan Garcia Huitron, Jean X. Jiang, Christopher R. Rathbone, Eric M. Brey
Journal of Tissue Engineering.2022; 13: 204173142211093. CrossRef - Atractylenolide III from Atractylodes macrocephala Koidz promotes the activation of brown and white adipose tissue through SIRT1/PGC-1α signaling pathway
Xin Liu, Yuan Huang, Xu Liang, Qiong Wu, Nan Wang, Li-jun Zhou, Wen-wu Liu, Qun Ma, Bei Hu, Huan Gao, Ya-ling Cui, Xiang Li, Qing-chun Zhao
Phytomedicine.2022; 104: 154289. CrossRef - The pathobiology of perivascular adipose tissue (PVAT), the fourth layer of the blood vessel wall
Cassie Hillock-Watling, Avrum I. Gotlieb
Cardiovascular Pathology.2022; 61: 107459. CrossRef - RNA-Binding Proteins in the Regulation of Adipogenesis and Adipose Function
Pengpeng Zhang, Wenyan Wu, Chaofeng Ma, Chunyu Du, Yueru Huang, Haixia Xu, Cencen Li, Xiaofang Cheng, Ruijie Hao, Yongjie Xu
Cells.2022; 11(15): 2357. CrossRef - The Effect of Swimming Training with Cinnamon Consumption on β3-AR and ERK2 Gene Expression in the Visceral Adipose Tissue of Diabetic Rats
Kianoosh Mohammadi, Ali Khajehlandi, Amin Mohammadi
Gene, Cell and Tissue.2022;[Epub] CrossRef - Of mice and men: Considerations on adipose tissue physiology in animal models of obesity and human studies
Ioannis G. Lempesis, Dimitrios Tsilingiris, Junli Liu, Maria Dalamaga
Metabolism Open.2022; 15: 100208. CrossRef - The comparison of the effect of acute moderate and high-intensity exercise on the uncoupling protein -1 secretion
Desiana Merawati, Sugiharto Sugiharto, Adi Pranoto, Olivia Andiana, Prayogi Dwina Angga
Jurnal SPORTIF : Jurnal Penelitian Pembelajaran.2022; 8(2): 201. CrossRef - Omega-3 Polyunsaturated Fatty Acids Protect against High-Fat Diet-Induced Morphological and Functional Impairments of Brown Fat in Transgenic Fat-1 Mice
Lei Hao, Yong-Hui Nie, Chih-Yu Chen, Xiang-Yong Li, Kanakaraju Kaliannan, Jing X. Kang
International Journal of Molecular Sciences.2022; 23(19): 11903. CrossRef - Modulation of hypothalamic AMPK phosphorylation by olanzapine controls energy balance and body weight
Vitor Ferreira, Cintia Folgueira, Maria Guillén, Pablo Zubiaur, Marcos Navares, Assel Sarsenbayeva, Pilar López-Larrubia, Jan W. Eriksson, Maria J. Pereira, Francisco Abad-Santos, Guadalupe Sabio, Patricia Rada, Ángela M. Valverde
Metabolism.2022; 137: 155335. CrossRef - Okra (Abelmoschus esculentus L. Moench) prevents obesity by reducing lipid accumulation and increasing white adipose browning in high-fat diet-fed mice
Heegu Jin, Hyun-Ji Oh, Sehaeng Cho, Ok-Hwan Lee, Boo-Yong Lee
Food & Function.2022; 13(22): 11840. CrossRef - Functional Attenuation of UCP1 as the Potential Mechanism for a Thickened Blubber Layer in Cetaceans
Ming Zhou, Tianzhen Wu, Yue Chen, Shixia Xu, Guang Yang, Anne Yoder
Molecular Biology and Evolution.2022;[Epub] CrossRef - Brown adipose tissue transplantation as a novel alternative to obesity treatment: a systematic review
Moloud Payab, Mina Abedi, Najmeh Foroughi Heravani, Mahdieh Hadavandkhani, Maryam Arabi, Akram Tayanloo-Beik, Motahareh Sheikh Hosseini, Hadis Gerami, Fateme Khatami, Bagher Larijani, Mohammad Abdollahi, Babak Arjmand
International Journal of Obesity.2021; 45(1): 109. CrossRef - Corylin reduces obesity and insulin resistance and promotes adipose tissue browning through SIRT-1 and β3-AR activation
Chin-Chuan Chen, Chen-Hsin Kuo, Yann-Lii Leu, Shu-Huei Wang
Pharmacological Research.2021; 164: 105291. CrossRef - Inducible beige adipocytes improve impaired glucose metabolism in interscapular BAT-removal mice
Xiao-Wei Jia, Dong-Liang Fang, Xin-Yi Shi, Tao Lu, Chun Yang, Yan Gao
Biochimica et Biophysica Acta (BBA) - Molecular and Cell Biology of Lipids.2021; 1866(3): 158871. CrossRef - NNT‐induced tumor cell “slimming” reverses the pro‐carcinogenesis effect of HIF2a in tumors
Zhiyong Xiong, Wei Xiong, Wen Xiao, Changfei Yuan, Jian Shi, Yu Huang, Cheng Wang, Xiangui Meng, Zhixian Chen, Hongmei Yang, Ke Chen, Xiaoping Zhang
Clinical and Translational Medicine.2021;[Epub] CrossRef - CD10 marks non-canonical PPARγ-independent adipocyte maturation and browning potential of adipose-derived stem cells
Smarajit Chakraborty, Wee Kiat Ong, Winifred W. Y. Yau, Zhihong Zhou, K. N. Bhanu Prakash, Sue-Anne Toh, Weiping Han, Paul M. Yen, Shigeki Sugii
Stem Cell Research & Therapy.2021;[Epub] CrossRef - Regulatory roles of G-protein coupled receptors in adipose tissue metabolism and their therapeutic potential
Hyeonyeong Im, Ji-Hyun Park, Seowoo Im, Juhyeong Han, Kyungmin Kim, Yun-Hee Lee
Archives of Pharmacal Research.2021; 44(2): 133. CrossRef - 3-N-butylphthalide protects against high-fat-diet-induced obesity in C57BL/6 mice and increases metabolism in lipid-accumulating cells
Kang-Yun Lu, Shinn-Zong Lin, Kingsley Theras Primus Dass, Wei-Ju Lin, Shih-Ping Liu, Horng-Jyh Harn
Biomedicine & Pharmacotherapy.2021; 139: 111687. CrossRef - Ellagic acid induces beige remodeling of white adipose tissue by controlling mitochondrial dynamics and SIRT3
Woo Yong Park, Jinbong Park, Kwang Seok Ahn, Hyun Jeong Kwak, Jae‐Young Um
The FASEB Journal.2021;[Epub] CrossRef - Cajanolactone A, a Stilbenoid From Cajanus canjan (L.) Millsp, Prevents High-Fat Diet-Induced Obesity via Suppressing Energy Intake
Zhuohui Luo, Jiawen Huang, Zhiping Li, Zhiwen Liu, Linchun Fu, Yingjie Hu, Xiaoling Shen
Frontiers in Pharmacology.2021;[Epub] CrossRef - Zinc and the Innovative Zinc-α2-Glycoprotein Adipokine Play an Important Role in Lipid Metabolism: A Critical Review
Michalina Banaszak, Ilona Górna, Juliusz Przysławski
Nutrients.2021; 13(6): 2023. CrossRef - Natural products in the management of obesity: Fundamental mechanisms and pharmacotherapy
Yinghan Chan, Sin Wi Ng, Joycelin Zhu Xin Tan, Gaurav Gupta, Poonam Negi, Lakshmi Thangavelu, Sri Renukadevi Balusamy, Haribalan Perumalsamy, Wei Hsum Yap, Sachin Kumar Singh, Vanni Caruso, Kamal Dua, Dinesh Kumar Chellappan
South African Journal of Botany.2021; 143: 176. CrossRef - Group IIA secreted phospholipase A2 (PLA2G2A) augments adipose tissue thermogenesis
Michael S. Kuefner, Erin Stephenson, Mladen Savikj, Heather S. Smallwood, Qingming Dong, Christine Payré, Gérard Lambeau, Edwards A. Park
The FASEB Journal.2021;[Epub] CrossRef - N-butylidenephthalide ameliorates high-fat diet-induced obesity in mice and promotes browning through adrenergic response/AMPK activation in mouse beige adipocytes
Kang-Yun Lu, Kingsley Theras Primus Dass, Shinn-Zong Lin, Yu-Hua Tseng, Shih-Ping Liu, Horng-Jyh Harn
Biochimica et Biophysica Acta (BBA) - Molecular and Cell Biology of Lipids.2021; 1866(12): 159033. CrossRef - Green tea aqueous extract (GTAE) prevents high‐fat diet‐induced obesity by activating fat browning
Jie Li, Qiyang Chen, Xiuming Zhai, Dan Wang, Yujia Hou, Min Tang
Food Science & Nutrition.2021; 9(12): 6548. CrossRef - Ipragliflozin, an SGLT2 Inhibitor, Ameliorates High-Fat Diet-Induced Metabolic Changes by Upregulating Energy Expenditure through Activation of the AMPK/ SIRT1 Pathway
Ji-Yeon Lee, Minyoung Lee, Ji Young Lee, Jaehyun Bae, Eugene Shin, Yong-ho Lee, Byung-Wan Lee, Eun Seok Kang, Bong-Soo Cha
Diabetes & Metabolism Journal.2021; 45(6): 921. CrossRef - The increase of uncoupling protein-1 expression after moderate intensity continuous exercises in obese females
Sugiharto, Banih Sakti Adji, Desiana Merawati, Adi Pranoto
Jurnal SPORTIF : Jurnal Penelitian Pembelajaran.2021; 7(2): 194. CrossRef - Effects of Royal Jelly and Tocotrienol Rich Fraction in obesity treatment of calorie-restricted obese rats: a focus on white fat browning properties and thermogenic capacity
Naimeh Mesri Alamdari, Pardis Irandoost, Neda Roshanravan, Mohammadreza Vafa, Mohammad Asghari Jafarabadi, Shahriar Alipour, Leila Roshangar, Mohammadreza Alivand, Farnaz Farsi, Farzad Shidfar
Nutrition & Metabolism.2020;[Epub] CrossRef - Metabolic Benefits of MicroRNA-22 Inhibition
Marc Thibonnier, Christine Esau
Nucleic Acid Therapeutics.2020; 30(2): 104. CrossRef - Grape pomace extract supplementation activates FNDC5/irisin in muscle and promotes white adipose browning in rats fed a high-fat diet
Cecilia Rodriguez Lanzi, Diahann J. Perdicaro, Julián Gambarte Tudela, Victoria Muscia, Ariel R. Fontana, Patricia I. Oteiza, Marcela A. Vazquez Prieto
Food & Function.2020; 11(2): 1537. CrossRef - Citrus aurantium L. polymethoxyflavones promote thermogenesis of brown and white adipose tissue in high-fat diet induced C57BL/6J mice
Guangning Kou, Yan Hu, Zixiao Jiang, Zhenqing Li, Peiyuan Li, Hongjie Song, Qiyang Chen, Zhiqin Zhou, Quanjun Lyu
Journal of Functional Foods.2020; 67: 103860. CrossRef - Beneficial effects of pomegranate peel extract treatment on anthropometry and body composition of overweight patients with diabetes mellitus type-2: A randomised clinical trial
Milkica Grabež, Ranko Škrbić, Miloš Stojiljković, Vesna Rudić-Grujić, Katarina Šavikin, Nebojša Menković, Gordana Zdunić, Nađa Vasiljević
Scripta Medica.2020; 51(1): 21. CrossRef - Milk fat globule membrane and its component phosphatidylcholine induce adipose browning both in vivo and in vitro
Tiange Li, Min Du, Hanning Wang, Xueying Mao
The Journal of Nutritional Biochemistry.2020; 81: 108372. CrossRef - Dynamic contrast‐enhanced MRI of brown and beige adipose tissues
Jadegoud Yaligar, Sanjay Kumar Verma, Venkatesh Gopalan, Rengaraj Anantharaj, Giang Thi Thu Le, Kavita Kaur, Karthik Mallilankaraman, MK Leow, SS Velan
Magnetic Resonance in Medicine.2020; 84(1): 384. CrossRef - Taurine Stimulates Thermoregulatory Genes in Brown Fat Tissue and Muscle without an Influence on Inguinal White Fat Tissue in a High-Fat Diet-Induced Obese Mouse Model
Kyoung Soo Kim, Hari Madhuri Doss, Hee-Jin Kim, Hyung-In Yang
Foods.2020; 9(6): 688. CrossRef - White adipose tissue browning in critical illness: A review of the evidence, mechanisms and future perspectives
Elham Alipoor, Mohammad Javad Hosseinzadeh‐Attar, Mahsa Rezaei, Shima Jazayeri, Marianne Chapman
Obesity Reviews.2020;[Epub] CrossRef - Metabolic and energetic benefits of microRNA-22 inhibition
Marc Thibonnier, Christine Esau, Sujoy Ghosh, Edward Wargent, Claire Stocker
BMJ Open Diabetes Research & Care.2020; 8(1): e001478. CrossRef - Apple polyphenols induce browning of white adipose tissue
Yuki Tamura, Shigeto Tomiya, Junya Takegaki, Karina Kouzaki, Arata Tsutaki, Koichi Nakazato
The Journal of Nutritional Biochemistry.2020; 77: 108299. CrossRef - Adipose TBX1 regulates β-adrenergic sensitivity in subcutaneous adipose tissue and thermogenic capacity in vivo
Kathleen R. Markan, Lauren K. Boland, Abdul Qaadir King-McAlpin, Kristin E. Claflin, Michael P. Leaman, Morgan K. Kemerling, Madison M. Stonewall, Brad A. Amendt, James A. Ankrum, Matthew J. Potthoff
Molecular Metabolism.2020; 36: 100965. CrossRef - A systematic review of the association of neuregulin 4, a brown fat–enriched secreted factor, with obesity and related metabolic disturbances
Helda Tutunchi, Alireza Ostadrahimi, Mohammad‐Javad Hosseinzadeh‐Attar, Mahsa Miryan, Majid Mobasseri, Mehrangiz Ebrahimi‐Mameghani
Obesity Reviews.2020;[Epub] CrossRef - Deficiency of glutathione peroxidase-1 and catalase attenuated diet-induced obesity and associated metabolic disorders
Hyung-Ran Kim, Eun-Jeong Choi, Jeong-Hae Kie, Joo-Ho Lee, Ju-Young Seoh
Acta Diabetologica.2020; 57(2): 151. CrossRef - Clinical Application Potential of Small Molecules that Induce Brown Adipose Tissue Thermogenesis by Improving Fat Metabolism
Kang-Yun Lu, Kingsley Theras Primus Dass, Sheng-Feng Tsai, Hong-Meng Chuang, Shinn-Zong Lin, Shih-Ping Liu, Horng-Jyh Harn
Cell Transplantation.2020; 29: 096368972092739. CrossRef - MiR‐92a regulates brown adipocytes differentiation, mitochondrial oxidative respiration, and heat generation by targeting SMAD7
Zhipin Zhang, Huixin Jiang, Xiang Li, Xiaomin Chen, Yihua Huang
Journal of Cellular Biochemistry.2020; 121(8-9): 3825. CrossRef - Bilirubin remodels murine white adipose tissue by reshaping mitochondrial activity and the coregulator profile of peroxisome proliferator–activated receptor α
Darren M. Gordon, Kari L. Neifer, Abdul-Rizaq Ali Hamoud, Charles F. Hawk, Andrea L. Nestor-Kalinoski, Scott A. Miruzzi, Michael P. Morran, Samuel O. Adeosun, Jeffrey G. Sarver, Paul W. Erhardt, Robert E. McCullumsmith, David E. Stec, Terry D. Hinds
Journal of Biological Chemistry.2020; 295(29): 9804. CrossRef - The Presence of Active Brown Adipose Tissue Determines Cold-Induced Energy Expenditure and Oxylipin Profiles in Humans
Oana C Kulterer, Laura Niederstaetter, Carsten T Herz, Alexander R Haug, Andrea Bileck, Dietmar Pils, Alexandra Kautzky-Willer, Christopher Gerner, Florian W Kiefer
The Journal of Clinical Endocrinology & Metabolism.2020; 105(7): 2203. CrossRef - Downregulation of osteopontin inhibits browning of white adipose tissues through PI3K-AKT pathway in C57BL / 6 mice
Yi Lu, Yuhong Xu, Wanwan Yuan, Mengxi Wang, Yumeng Zhou, Kai Chen, Qiren Huang
European Journal of Pharmacology.2020; 866: 172822. CrossRef - Angiotensin AT1 receptor antagonism by losartan stimulates adipocyte browning via induction of apelin
Dong Young Kim, Mi Jin Choi, Tae Kyung Ko, Na Hyun Lee, Ok-Hee Kim, Hyae Gyeong Cheon
Journal of Biological Chemistry.2020; 295(44): 14878. CrossRef - Isoliquiritigenin Enhances the Beige Adipocyte Potential of Adipose-Derived Stem Cells by JNK Inhibition
Hanbyeol Moon, Jung-Won Choi, Byeong-Wook Song, Il-Kwon Kim, Soyeon Lim, Seahyoung Lee, Ki-Chul Hwang, Sang Woo Kim
Molecules.2020; 25(23): 5660. CrossRef - In vitro evaluation of Hydrilla verticillata for anti-adipogenesis activity on 3T3 L1 cell lines
SPandi Prabha, S Sadhana, C Karthik, DG Caroline
Pharmacognosy Magazine.2020; 16(5): 498. CrossRef - Leptin Promotes White Adipocyte Browning by Inhibiting the Hh Signaling Pathway
Jie Wang, Jing Ge, Haigang Cao, Xiaoyu Zhang, Yuan Guo, Xiao Li, Bo Xia, Gongshe Yang, Xin’e Shi
Cells.2019; 8(4): 372. CrossRef - Impact of Gut Microbiota on Host Glycemic Control
Céline Gérard, Hubert Vidal
Frontiers in Endocrinology.2019;[Epub] CrossRef - Effect of resveratrol on adipokines and myokines involved in fat browning: Perspectives in healthy weight against obesity
Oh Yoen Kim, Ji Yeon Chung, Juhyun Song
Pharmacological Research.2019; 148: 104411. CrossRef - A comprehensive diagnostic approach to detect underlying causes of obesity in adults
Eline S. van der Valk, Erica L.T. van den Akker, Mesut Savas, Lotte Kleinendorst, Jenny A. Visser, Mieke M. Van Haelst, Arya M. Sharma, Elisabeth F.C. van Rossum
Obesity Reviews.2019; 20(6): 795. CrossRef - Prostacyclin: A major prostaglandin in the regulation of adipose tissue development
Mohammad Sharifur Rahman
Journal of Cellular Physiology.2019; 234(4): 3254. CrossRef - The expression of brown fat‐associated proteins in colorectal cancer and the relationship of uncoupling protein 1 with prognosis
Abdo Alnabulsi, Beatriz Cash, Yehfang Hu, Linda Silina, Ayham Alnabulsi, Graeme I. Murray
International Journal of Cancer.2019; 145(4): 1138. CrossRef - Garlic augments the functional and nutritional behavior of Doenjang, a traditional Korean fermented soybean paste
Ashutosh Bahuguna, Shruti Shukla, Jong Suk Lee, Vivek K. Bajpai, So-Young Kim, Yun Suk Huh, Young-Kyu Han, Myunghee Kim
Scientific Reports.2019;[Epub] CrossRef - Clomiphene promotes browning of white adipocytes via casein kinase-2 inhibition
Hyun-Jin Kim, Dong Young Kim, Hyae Gyeong Cheon
European Journal of Pharmacology.2019; 861: 172596. CrossRef - Neuroendocrine Regulation of Energy Metabolism Involving Different Types of Adipose Tissues
Qi Zhu, Bradley J. Glazier, Benjamin C. Hinkel, Jingyi Cao, Lin Liu, Chun Liang, Haifei Shi
International Journal of Molecular Sciences.2019; 20(11): 2707. CrossRef - Tumor Cell “Slimming” Regulates Tumor Progression through PLCL1/UCP1‐Mediated Lipid Browning
Zhiyong Xiong, Wen Xiao, Lin Bao, Wei Xiong, Haibing Xiao, Yan Qu, Changfei Yuan, Hailong Ruan, Qi Cao, Keshan Wang, Zhengshuai Song, Cheng Wang, Wenjun Hu, Zeyuan Ru, Junwei Tong, Gong Cheng, Tianbo Xu, Xiangui Meng, Jian Shi, Zhixian Chen, Hongmei Yang,
Advanced Science.2019;[Epub] CrossRef - Soyasaponin Ab alleviates postmenopausal obesity through browning of white adipose tissue
Han-Jun Kim, Eun-Ji Choi, Hyo Sung Kim, Chan-Woong Choi, Sik-Won Choi, Sun-Lim Kim, Woo-Duck Seo, Sun Hee Do
Journal of Functional Foods.2019; 57: 453. CrossRef - Beneficial Effects of Pomegranate Peel Extract and Probiotics on Pre-adipocyte Differentiation
Valeria Sorrenti, Cinzia Lucia Randazzo, Cinzia Caggia, Gabriele Ballistreri, Flora Valeria Romeo, Simona Fabroni, Nicolina Timpanaro, Marco Raffaele, Luca Vanella
Frontiers in Microbiology.2019;[Epub] CrossRef - Visfatin; a potential novel mediator of brown adipose tissue
Parmida Pourvali-Talatappeh, Elham Alipoor
Obesity Medicine.2019; 15: 100122. CrossRef - Strategies and methods for the correction of obesity and associated cardiovascular risk
T. Yu. Kuznetsova, M. A. Druzhilov, G. A. Chumakova, N. D. Veselovskaya
Russian Journal of Cardiology.2019; (4): 61. CrossRef - Polymeric Carriers for Controlled Drug Delivery in Obesity Treatment
Di Huang, Meng Deng, Shihuan Kuang
Trends in Endocrinology & Metabolism.2019; 30(12): 974. CrossRef - Tbx15 is required for adipocyte browning induced by adrenergic signaling pathway
Wei Sun, Xuemei Zhao, Zhengqi Wang, Yi Chu, Liufeng Mao, Shaoqiang Lin, Xuefei Gao, Yuna Song, Xiaoyan Hui, Shiqi Jia, Shibing Tang, Yong Xu, Aimin Xu, Kerry Loomes, Cunchuan Wang, Donghai Wu, Tao Nie
Molecular Metabolism.2019; 28: 48. CrossRef - Effects of caloric restriction on the expression of lipocalin-2 and its receptor in the brown adipose tissue of high-fat diet-fed mice
Kyung-Ah Park, Zhen Jin, Hyeong Seok An, Jong Youl Lee, Eun Ae Jeong, Eun Bee Choi, Kyung Eun Kim, Hyun Joo Shin, Jung Eun Lee, Gu Seob Roh
The Korean Journal of Physiology & Pharmacology.2019; 23(5): 335. CrossRef - Peripherally administered melanocortins induce mice fat browning and prevent obesity
Adriana R. Rodrigues, Maria J. Salazar, Sílvia Rocha-Rodrigues, Inês O. Gonçalves, Célia Cruz, Delminda Neves, Henrique Almeida, José Magalhães, Alexandra M. Gouveia
International Journal of Obesity.2019; 43(5): 1058. CrossRef - Chinese medicine Jinlida granules improve high-fat-diet induced metabolic disorders via activation of brown adipose tissue in mice
Hui Zhang, Yuanyuan Hao, Cong Wei, Bing Yao, Shen Liu, Hongru Zhou, Dan Huang, Chuanhai Zhang, Yiling Wu
Biomedicine & Pharmacotherapy.2019; 114: 108781. CrossRef - Effects of lobeglitazone, a novel thiazolidinedione, on adipose tissue remodeling and brown and beige adipose tissue development in db/db mice
G Kim, Y-h Lee, M R Yun, J-Y Lee, E G Shin, B-W Lee, E S Kang, B-S Cha
International Journal of Obesity.2018; 42(3): 542. CrossRef - Air Pollution Has a Significant Negative Impact on Intentional Efforts to Lose Weight: A Global Scale Analysis
Morena Ustulin, So Young Park, Sang Ouk Chin, Suk Chon, Jeong-taek Woo, Sang Youl Rhee
Diabetes & Metabolism Journal.2018; 42(4): 320. CrossRef - Phytol stimulates the browning of white adipocytes through the activation of AMP-activated protein kinase (AMPK) α in mice fed high-fat diet
Fenglin Zhang, Wei Ai, Xiaoquan Hu, Yingying Meng, Cong Yuan, Han Su, Lina Wang, Xiaotong Zhu, Ping Gao, Gang Shu, Qingyan Jiang, Songbo Wang
Food & Function.2018; 9(4): 2043. CrossRef - Nobiletin induces brown adipocyte-like phenotype and ameliorates stress in 3T3-L1 adipocytes
Jameel Lone, Hilal Ahmad Parray, Jong Won Yun
Biochimie.2018; 146: 97. CrossRef - Regular aerobic exercise correlates with reduced anxiety and incresed levels of irisin in brain and white adipose tissue
Nazan Uysal, Oguz Yuksel, Servet Kizildag, Zeynep Yuce, Hikmet Gumus, Aslı Karakilic, Guven Guvendi, Basar Koc, Sevim Kandis, Mehmet Ates
Neuroscience Letters.2018; 676: 92. CrossRef - The Root of Atractylodes macrocephala Koidzumi Prevents Obesity and Glucose Intolerance and Increases Energy Metabolism in Mice
Mi Song, Soo-Kyoung Lim, Jing-Hua Wang, Hojun Kim
International Journal of Molecular Sciences.2018; 19(1): 278. CrossRef - Differential actions of PPAR-α and PPAR-β/δ on beige adipocyte formation: A study in the subcutaneous white adipose tissue of obese male mice
Tamiris Lima Rachid, Flavia Maria Silva-Veiga, Francielle Graus-Nunes, Isabele Bringhenti, Carlos Alberto Mandarim-de-Lacerda, Vanessa Souza-Mello, Nobuyuki Takahashi
PLOS ONE.2018; 13(1): e0191365. CrossRef - Coordination Among Lipid Droplets, Peroxisomes, and Mitochondria Regulates Energy Expenditure Through the CIDE-ATGL-PPARα Pathway in Adipocytes
Linkang Zhou, Miao Yu, Muhammad Arshad, Wenmin Wang, Ye Lu, Jingyi Gong, Yangnan Gu, Peng Li, Li Xu
Diabetes.2018; 67(10): 1935. CrossRef - Lithocholic Acid Improves the Survival of Drosophila Melanogaster
Stefanie Staats, Gerald Rimbach, Axel Kuenstner, Simon Graspeuntner, Jan Rupp, Hauke Busch, Christian Sina, Ignacio R. Ipharraguerre, Anika E. Wagner
Molecular Nutrition & Food Research.2018;[Epub] CrossRef - Preconditioning lessens high fat induced metabolic syndrome along with markers of increased metabolic capacity in muscle and adipose tissue
Songpei Li, Xiu Zhou, Eunjung Jo, Ali Mahzari, Sherouk Fouda, Dongli Li, Kun Zhang, Ji-Ming Ye
Bioscience Reports.2018;[Epub] CrossRef - Alternative mRNA Splicing in the Pathogenesis of Obesity
Chi-Ming Wong, Lu Xu, Mabel Yau
International Journal of Molecular Sciences.2018; 19(2): 632. CrossRef - Krüppel-Like Factors
Nina M. Pollak, Matthew Hoffman, Ira J. Goldberg, Konstantinos Drosatos
JACC: Basic to Translational Science.2018; 3(1): 132. CrossRef - Dietary n-3 long-chain polyunsaturated fatty acids upregulate energy dissipating metabolic pathways conveying anti-obesogenic effects in mice
Stefanie Worsch, Mathias Heikenwalder, Hans Hauner, Bernhard L. Bader
Nutrition & Metabolism.2018;[Epub] CrossRef - Combination of Capsaicin and Hesperidin Reduces the Effectiveness of Each Compound To Decrease the Adipocyte Size and To Induce Browning Features in Adipose Tissue of Western Diet Fed Rats
Andrea Mosqueda-Solís, Juana Sánchez, María P. Portillo, Andreu Palou, Catalina Picó
Journal of Agricultural and Food Chemistry.2018; 66(37): 9679. CrossRef - Regulation of Adipose Tissue Metabolism by the Endocannabinoid System
Robin van Eenige, Mario van der Stelt, Patrick C.N. Rensen, Sander Kooijman
Trends in Endocrinology & Metabolism.2018; 29(5): 326. CrossRef - Cardiovascular and Metabolic Heterogeneity of Obesity
Ian J. Neeland, Paul Poirier, Jean-Pierre Després
Circulation.2018; 137(13): 1391. CrossRef - Zinc alpha2 glycoprotein promotes browning in adipocytes
Xin-Hua Xiao, Xiao-Yan Qi, Ya-Di Wang, Li Ran, Jing Yang, Huan-Li Zhang, Can-Xin Xu, Ge-Bo Wen, Jiang-Hua Liu
Biochemical and Biophysical Research Communications.2018; 496(2): 287. CrossRef - Impacts of High Sodium Intake on Obesity-related Gene Expression
Minjee Lee, Miyoung Park, Juhee Kim, Soyoung Sung, Myoungsook Lee
Journal of the East Asian Society of Dietary Life.2018; 28(5): 364. CrossRef - Programming mediated by fatty acids affects uncoupling protein 1 (UCP-1) in brown adipose tissue
Perla P. Argentato, Helena de Cássia César, Débora Estadella, Luciana P. Pisani
British Journal of Nutrition.2018; 120(6): 619. CrossRef - Reversal of Fatty Infiltration After Suprascapular Nerve Compression Release Is Dependent on UCP1 Expression in Mice
Zili Wang, Brian T. Feeley, Hubert T. Kim, Xuhui Liu
Clinical Orthopaedics & Related Research.2018; 476(8): 1665. CrossRef - Increase in relative skeletal muscle mass over time and its inverse association with metabolic syndrome development: a 7-year retrospective cohort study
Gyuri Kim, Seung-Eun Lee, Ji Eun Jun, You-Bin Lee, Jiyeon Ahn, Ji Cheol Bae, Sang-Man Jin, Kyu Yeon Hur, Jae Hwan Jee, Moon-Kyu Lee, Jae Hyeon Kim
Cardiovascular Diabetology.2018;[Epub] CrossRef - Myricetin-induced brown adipose tissue activation prevents obesity and insulin resistance in db/db mice
Tao Hu, Xiaoxue Yuan, Gang Wei, Haoshu Luo, Hyuek Jong Lee, Wanzhu Jin
European Journal of Nutrition.2018; 57(1): 391. CrossRef - Effects of growth hormone on uncoupling protein 1 in white adipose tissues in obese mice
Misa Hayashi, Kumi Futawaka, Rie Koyama, Yue Fan, Midori Matsushita, Asuka Hirao, Yuki Fukuda, Ayako Nushida, Syoko Nezu, Tetsuya Tagami, Kenji Moriyama
Growth Hormone & IGF Research.2017; 37: 31. CrossRef - Position paper of the European Society of Cardiology–working group of coronary pathophysiology and microcirculation: obesity and heart disease
Lina Badimon, Raffaele Bugiardini, Edina Cenko, Judit Cubedo, Maria Dorobantu, Dirk J. Duncker, Ramón Estruch, Davor Milicic, Dimitris Tousoulis, Zorana Vasiljevic, Gemma Vilahur, Cor de Wit, Akos Koller
European Heart Journal.2017; 38(25): 1951. CrossRef - Browning of Abdominal Aorta Perivascular Adipose Tissue Inhibits Adipose Tissue Inflammation
Run-Mei Li, Sui-Qing Chen, Ning-Xi Zeng, Shu-Hui Zheng, Li Guan, Hai-Mei Liu, Le-Quan Zhou, Jin-Wen Xu
Metabolic Syndrome and Related Disorders.2017; 15(9): 450. CrossRef - The role of adipose tissue in cancer-associated cachexia
Janina A Vaitkus, Francesco S Celi
Experimental Biology and Medicine.2017; 242(5): 473. CrossRef - Hormonal factors in the control of the browning of white adipose tissue
Jiamiao Hu, Mark Christian
Hormone Molecular Biology and Clinical Investigation.2017;[Epub] CrossRef - European contribution to the study of ROS: A summary of the findings and prospects for the future from the COST action BM1203 (EU-ROS)
Javier Egea, Isabel Fabregat, Yves M. Frapart, Pietro Ghezzi, Agnes Görlach, Thomas Kietzmann, Kateryna Kubaichuk, Ulla G. Knaus, Manuela G. Lopez, Gloria Olaso-Gonzalez, Andreas Petry, Rainer Schulz, Jose Vina, Paul Winyard, Kahina Abbas, Opeyemi S. Adem
Redox Biology.2017; 13: 94. CrossRef - Resveratrol enhances brown adipocyte formation and function by activating AMP‐activated protein kinase (AMPK) α1 in mice fed high‐fat diet
Songbo Wang, Xingwei Liang, Qiyuan Yang, Xing Fu, Meijun Zhu, B. D. Rodgers, Qingyan Jiang, Michael V. Dodson, Min Du
Molecular Nutrition & Food Research.2017;[Epub] CrossRef - Adipoz doku ve enerji metabolizması üzerine etkileri
Meltem Mermer, Nilüfer Acar TEK
SDÜ Sağlık Bilimleri Dergisi.2017;[Epub] CrossRef - Physiological roles of macrophages
Siamon Gordon, Luisa Martinez-Pomares
Pflügers Archiv - European Journal of Physiology.2017; 469(3-4): 365. CrossRef - Brown Adipose Tissue Bioenergetics: A New Methodological Approach
María Calderon‐Dominguez, Martín Alcalá, David Sebastián, Antonio Zorzano, Marta Viana, Dolors Serra, Laura Herrero
Advanced Science.2017;[Epub] CrossRef - Honokiol exerts dual effects on browning and apoptosis of adipocytes
Jameel Lone, Jong Won Yun
Pharmacological Reports.2017; 69(6): 1357. CrossRef - The Mixed Herbal Extract, CAPA, Prevents Obesity and Glucose Intolerance in Obese Mice
Miyoung Song
Journal of Korean Medicine for Obesity Research.2017; 17(2): 119. CrossRef - Brown Adipose Tissue: an Update on Recent Findings
Kara L. Marlatt, Eric Ravussin
Current Obesity Reports.2017; 6(4): 389. CrossRef - Radix Stellariae extract prevents high-fat-diet-induced obesity in C57BL/6 mice by accelerating energy metabolism
Yin Li, Xin Liu, Yu Fan, Baican Yang, Cheng Huang
PeerJ.2017; 5: e3305. CrossRef - Adipocyte arrestin domain-containing 3 protein (Arrdc3) regulates uncoupling protein 1 (Ucp1) expression in white adipose independently of canonical changes in β-adrenergic receptor signaling
Shannon H. Carroll, Ellen Zhang, Bing F. Wang, Katherine B. LeClair, Arifeen Rahman, David E. Cohen, Jorge Plutzky, Parth Patwari, Richard T. Lee, Makoto Kanzaki
PLOS ONE.2017; 12(3): e0173823. CrossRef - Effect of Long-Term Green Tea Extract Supplementation on Peripheral Blood Leukocytes in CrossFit-Trained and Untrained Men
Agata Żak, Ilona Pokora
Central European Journal of Sport Sciences and Medicine.2017; 19: 67. CrossRef - Rapid modulation of lipid metabolism in C57BL/6J mice induced by eicosapentaenoic acid-enriched phospholipid from Cucumaria frondosa
Lingyu Zhang, Dan Wang, Min Wen, Lei Du, Changhu Xue, Jingfeng Wang, Jie Xu, Yuming Wang
Journal of Functional Foods.2017; 28: 28. CrossRef - Egr1 deficiency induces browning of inguinal subcutaneous white adipose tissue in mice
Cécile Milet, Marianne Bléher, Kassandra Allbright, Mickael Orgeur, Fanny Coulpier, Delphine Duprez, Emmanuelle Havis
Scientific Reports.2017;[Epub] CrossRef - Purinergic Receptors in Adipose Tissue As Potential Targets in Metabolic Disorders
Marco Tozzi, Ivana Novak
Frontiers in Pharmacology.2017;[Epub] CrossRef - Phyllodulcin, a Natural Sweetener, Regulates Obesity-Related Metabolic Changes and Fat Browning-Related Genes of Subcutaneous White Adipose Tissue in High-Fat Diet-Induced Obese Mice
Eunju Kim, Soo-Min Lim, Min-Soo Kim, Sang-Ho Yoo, Yuri Kim
Nutrients.2017; 9(10): 1049. CrossRef - Yogurt and Cardiometabolic Diseases: A Critical Review of Potential Mechanisms
Melissa Anne Fernandez, Shirin Panahi, Noémie Daniel, Angelo Tremblay, André Marette
Advances in Nutrition.2017; 8(6): 812. CrossRef - Système endocannabinoïde : effets sur le métabolisme glucidique, mais aussi lipidique
A.-L. Sberna, P. Degrace, B. Vergès
Médecine des Maladies Métaboliques.2016; 10(5): 407. CrossRef - The Fat Side of the Endocannabinoid System: Role of Endocannabinoids in the Adipocyte
Isabelle Matias, Ilaria Belluomo, Daniela Cota
Cannabis and Cannabinoid Research.2016; 1(1): 176. CrossRef - Liraglutide suppresses obesity and induces brown fat-like phenotype via Soluble Guanylyl Cyclase mediated pathwayin vivoandin vitro
Endong Zhu, Yang Yang, Juanjuan Zhang, Yongmei Li, Chunjun Li, Liming Chen, Bei Sun
Oncotarget.2016; 7(49): 81077. CrossRef - NS5ATP6 modulates intracellular triglyceride content through FGF21 and independently of SIRT1 and SREBP1
Zhongshu Li, Shenghu Feng, Li Zhou, Shunai Liu, Jun Cheng
Biochemical and Biophysical Research Communications.2016; 475(1): 133. CrossRef - Novel device for male infertility screening with single-ball lens microscope and smartphone
Yoshitomo Kobori, Peter Pfanner, Gail S. Prins, Craig Niederberger
Fertility and Sterility.2016; 106(3): 574. CrossRef - An Intestinal Microbiota–Farnesoid X Receptor Axis Modulates Metabolic Disease
Frank J. Gonzalez, Changtao Jiang, Andrew D. Patterson
Gastroenterology.2016; 151(5): 845. CrossRef - Feast and famine: Adipose tissue adaptations for healthy aging
Daniele Lettieri Barbato, Katia Aquilano
Ageing Research Reviews.2016; 28: 85. CrossRef - Hypothalamus and thermogenesis: Heating the BAT, browning the WAT
Cristina Contreras, Rubén Nogueiras, Carlos Diéguez, Gema Medina-Gómez, Miguel López
Molecular and Cellular Endocrinology.2016; 438: 107. CrossRef - Concomitant beige adipocyte differentiation upon induction of mesenchymal stem cells into brown adipocytes
Yung-Li Wang, Shih-Pei Lin, Patrick C.H. Hsieh, Shih-Chieh Hung
Biochemical and Biophysical Research Communications.2016; 478(2): 689. CrossRef

 KDA
KDA PubReader
PubReader Cite
Cite