- Current
- Browse
- Collections
-
For contributors
- For Authors
- Instructions to authors
- Article processing charge
- e-submission
- For Reviewers
- Instructions for reviewers
- How to become a reviewer
- Best reviewers
- For Readers
- Readership
- Subscription
- Permission guidelines
- About
- Editorial policy
Articles
- Page Path
- HOME > Diabetes Metab J > Volume 46(6); 2022 > Article
-
Short CommunicationTechnology/Devise Comparison of Laser and Conventional Lancing Devices for Blood Glucose Measurement Conformance and Patient Satisfaction in Diabetes Mellitus
-
Jung A Kim1,2
 , Min Jeong Park1, Eyun Song1, Eun Roh1, So Young Park1, Da Young Lee1, Jaeyoung Kim3, Ji Hee Yu1, Ji A Seo1, Kyung Mook Choi1, Sei Hyun Baik1, Hye Jin Yoo1
, Min Jeong Park1, Eyun Song1, Eun Roh1, So Young Park1, Da Young Lee1, Jaeyoung Kim3, Ji Hee Yu1, Ji A Seo1, Kyung Mook Choi1, Sei Hyun Baik1, Hye Jin Yoo1 , Nan Hee Kim1,4
, Nan Hee Kim1,4
-
Diabetes & Metabolism Journal 2022;46(6):936-940.
DOI: https://doi.org/10.4093/dmj.2021.0293
Published online: March 30, 2022
1Division of Endocrinology and Metabolism, Department of Internal Medicine, Korea University College of Medicine, Seoul, Korea
2Division of Endocrinology and Metabolism, Department of Internal Medicine, Daejin Medical Center, Bundang Jesaeng Hospital, Seongnam, Korea
3Research Institute for Skin Imaging, Korea University College of Medicine, Seoul, Korea
4BK21 FOUR R&E Center for Learning Health Systems, Korea University, Seoul, Korea
- Corresponding authors: Hye Jin Yoo Division of Endocrinology and Metabolism, Department of Internal Medicine, Korea University Guro Hospital, Korea University College of Medicine, 148 Gurodong-ro, Guro-gu, Seoul 08308, Korea E-mail: deisy21@naver.com
- Nan Hee Kim Division of Endocrinology and Metabolism, Department of Internal Medicine, Korea University Ansan Hospital, Korea University College of Medicine, 123 Jeokgeum-ro, Danwon-gu, Ansan 15355, Korea E-mail: nhkendo@gmail.com
Copyright © 2022 Korean Diabetes Association
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
ABSTRACT
- Self-monitoring of capillary blood glucose is important for controlling diabetes. Recently, a laser lancing device (LMT-1000) that can collect capillary blood without skin puncture was developed. We enrolled 150 patients with type 1 or 2 diabetes mellitus. Blood sampling was performed on the same finger on each hand using the LMT-1000 or a conventional lancet. The primary outcome was correlation between glucose values using the LMT-1000 and that using a lancet. And we compared the pain and satisfaction of the procedures. The capillary blood sampling success rates with the LMT-1000 and lancet were 99.3% and 100%, respectively. There was a positive correlation (r=0.974, P<0.001) between mean blood glucose levels in the LMT-1000 (175.8±63.0 mg/dL) and conventional lancet samples (172.5±63.6 mg/dL). LMT-1000 reduced puncture pain by 75.0% and increased satisfaction by 80.0% compared to a lancet. We demonstrated considerable consistency in blood glucose measurements between samples from the LMT-1000 and a lancet, but improved satisfaction and clinically significant pain reduction were observed with the LMT-1000 compared to those with a lancet.
- Self-monitoring of blood glucose (SMBG) has been proven to reduce glycosylated hemoglobin (HbA1c) level and is useful for optimizing glycemic control and preventing diabetic complications by helping one understand their pattern of blood glucose level and facilitating lifestyle modifications [1-4]. Despite the importance of SMBG in glucose control, only 33% of patients with diabetes perform SMBG routinely [5] because of puncture pain, fear of needles, inconvenience, complexity, cost, and increased risk of infection [6]. Lancing pain is the main reason for noncompliance among patients with diabetes.
- Recently, LAMEDITECH developed a lancing device, LMT-1000 (HandyRay-Lite, LAMEDITECH, Seoul, Korea), that uses a 2,940 nm single-pulse (erbium-doped yttrium aluminum garnet or erbium YAG) laser that generates high energy and obtains capillary blood in a short time. Previous study with healthy subjects, the laser lancing device is less painful than lancing, has a high success rate of blood sampling [7].
- In this study, we aimed to use the LMT-1000 and a conventional lancet to measure capillary glucose levels in patients with diabetes to evaluate the correlation of glucose values and to compare puncture pain and treatment satisfaction between the two devices.
INTRODUCTION
- Study population and design
- A total of 150 patients aged 19 to 79 years and diagnosed with type 1 diabetes mellitus (T1DM) or type 2 diabetes mellitus (T2DM) from Korea University Guro Hospital or Ansan Hospital were enrolled in this study. The primary outcome was the correlation between glucose values using the LMT-1000 and that using a lancet. In addition, we compared the pain and satisfaction of the procedures. Blood sampling was performed on the same fingers on both hands using the LMT-1000 and the lancet. The initial energy power of the LMT-1000 was 140 mJ, and the initial depth of the lancet was the same as that used by the patients. If initial blood sampling failed, a second attempt was performed using the same device, but the energy level of the LMT-1000 was increased (180 mJ) and the lancet was injected to a greater depth. Capillary blood glucose concentration was measured by Barozehn plus (i-SenS Inc., Seoul, Korea). All patients were required to evaluate the grade of pain (numeric rating scale [NRS]) [8] and satisfaction (visual analog scale [VAS]) [9] with each procedure immediately after sampling. Written informed consent was obtained from each participant, and the study was conducted in accordance with the World Medical Association Declaration of Helsinki. The study protocol was approved by the Korea University Institutional Review Board (2020GR0582).
- Laser lancing device (LMT-1000)
- The LMT-1000 is a laser lancing device. The LMT-1000 energy level can be categorized into three levels: level 1, 100 mJ; level 2, 140 mJ; and level 3, 180 mJ. Energy level 1 is usually used for pediatric patients. Energy levels 2 and 3 were used.
- Conventional lancing device (lancet)
- A 28-gauge lancet and manual lancing device named LANZO (GMMC, Seoul, Korea) were used. The patients were instructed to collect capillary blood at the level of depth used on a daily basis.
- Statistical methods
- Descriptive data were presented as mean±standard deviation, median (interquartile range [IQR]), and number (%). Comparisons of baseline characteristics, pain, and satisfaction between the groups were assessed using a Mann-Whitney U test or chi-square test. The correlation of glucose values between the LMT-1000 and lancet groups was analyzed using linear regression and Passing-Bablok regression. A Bland-Altman analysis was used to evaluate the agreement between the glucose values derived from the LMT-1000 and the lancet. Clarke error grid analysis was performed to assess the clinical relevance of errors between measurements using LMT-1000 and lancet samples [10]. Statistical analysis was performed using SPSS version 20 (IBM Co., Armonk, NY, USA) and MedCalc v.19.0 (https://www.medcalc.org). A P<0.05 indicated clinical significance.
METHODS
- Baseline characteristics
- A total of 150 patients (men 86, women 64) with diabetes were enrolled in this study. Five (3.3%) patients had T1DM and 145 (96.7%) patients had T2DM. The mean HbA1c level was 7.2% (IQR, 6.7% to 8.1%). The number of patients using insulin was 47 (31.3%). The mean frequency of SMBG was three times per week (IQR, 1.0 to 7.0).
- Comparison of glucose concentration between the LMT-1000 and lancet samples
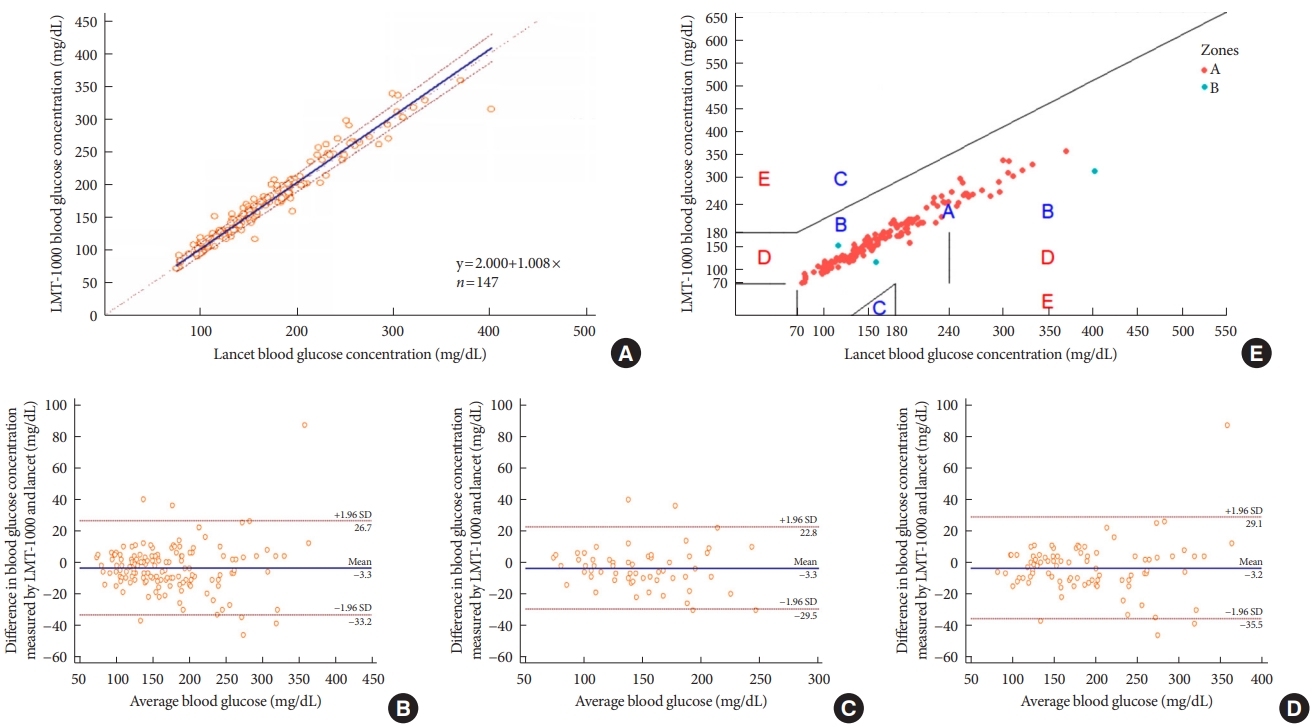
- In the correlation test, we excluded three patients due to failure to puncture the skin in two and glucose level >600 mg/dL in one. Mean capillary glucose levels of the LMT-1000 and lancet samples were 175.8±63.0 and 172.5±63.6 mg/dL, respectively. Pearson correlation analysis showed a positive correlation between the LMT-1000 and lancet samples (r=0.974, P<0.001). Passing-Bablok regression exhibited no significant deviation from linearity (P=0.37) (Fig. 1A). Bland-Altman analysis showed agreement between the blood glucose levels of LMT-1000 and lancet samples independent of baseline glucose level (Fig. 1B-D). In error grid analysis, 97.96% of values fell within zone A, 2.04% in zone B, and 0% in zones C, D, and E (Fig. 1E). The areas of zones A and B indicated that there was no effect on clinical action or altered clinical action had little or no effect on clinical outcomes, suggesting excellent consistency of blood glucose measurements between the two devices.
- Comparison of pain and satisfaction between sampling with the LMT-1000 and a lancet
- Among the 150 patients with diabetes, the success rates for the lancet and LMT-1000 devices were 100% (n=150) and 99.3% (n=149), respectively (Table 1). The median pain scores were 4.0 (IQR, 3.0 to 6.0) and 1.0 (IQR, 0.0 to 2.0) for the lancet and LMT-1000 devices, respectively (P<0.001), and the median satisfaction scores were 5.0 (IQR, 3.0 to 7.0) and 9.0 (IQR, 7.0 to 10.0) (P<0.001). Notably, even in the second attempt, the pain and satisfaction scores were significantly better than those of the lancet device. The only adverse event caused by the LMT-1000 device was a tingling sensation in one patient, but the patient recovered and the symptom disappeared within 4 days.
RESULTS
- In this study, we demonstrated the clinical benefits of a laser lancing device, LMT-1000, in patients with diabetes. The capillary blood glucose concentration of LMT-1000 samples correlated with the findings obtained using lancet samples and remained consistent independent of baseline glucose level. In addition, the LMT-1000 device exhibited a significant reduction in pain and improvement of satisfaction with capillary blood glucose sampling. No significant adverse events or complications were observed.
- SMBG plays a key role in management of diabetes [11-13]. However, numerous barriers exist to routine use of SMBG. One of the main obstacles is needle phobia and lancing pain [5,14]. In our study, the LMT-1000 device exhibited statistically significant improvement in lancing pain (NRS score 4 to 1) and satisfaction (VAS score 5 to 9) compared to the lancet device. Importantly, even during a second attempt at blood sampling using a higher energy level for patients who failed the first attempt of sampling with the LMT-1000 device, pain scores did not differ from those of the first attempt and were still lower than the scores with the lancet device. A possible mechanism underlying this low pain sensation is shallow penetration depth of the LMT-1000. By not contacting the reticular dermis, which has abundant free nerve endings, patients only experience touch sensations when using the LMT-1000 [15]. In addition, since the LMT-1000 does not utilize a needle, it avoids needle phobia. Based on these results, a laser device could reduce anxiety and fear before puncture, which can further increase compliance and help achieve adequate glucose control to prevent or delay diabetic complications.
- To increase SMBG compliance, the following components should meet patient expectations. First, there should be a high correlation in biochemical value measurements between the LMT-1000 and conventional methods. Our study demonstrated conformance between the two lancing devices regardless of the baseline glucose level. Second, the device should be safe for use. The LMT-1000 does not require a needle for perforating the skin, it can prevent needle stick injury and does not increase the risk of infection. In addition, the LMT-1000 method has several steps to prevent accidental exposure of eyes to lasers [16]. Our study had several limitations. First, we analyzed with relatively small size of Korean diabetic patients. Second, although the official intra-observer coefficient of variation (CV) of LMT-1000 is between 1.7% and 2.0%, meaning strong stability in its energy output, LMT-1000 performed only one comparison per person in this study. Therefore, a prospective randomized controlled study evaluating the efficacy of LMT-1000 in self-glucose control and long-term safety is on-going (CRIS number: KCT0006555). Third, Lanzo may not be a perfect control device that represents a general lancet, thus comparisons between LMT-1000 and several types of conventional lancets are necessary. The strength of this study is the efficacy representation of a novel laser lancing device, LMT-1000, for blood sampling in patients with diabetes for the first time.
- In our study, capillary glucose level of LMT-1000 samples correlated with that of lancet samples regardless of baseline glucose levels In addition, the LMT-1000 significantly reduced pain and improved satisfaction with capillary glucose sampling. Therefore, this novel lancing device, LMT-1000, might improve patient compliance with blood glucose monitoring to allow reliable measurement.
DISCUSSION
-
CONFLICTS OF INTEREST
- Ji A Seo has been associate editors of the Diabetes & Metabolism Journal since 2021. Hye Jin Yoo was been associate editors of the Diabetes & Metabolism Journal from 2020 to 2021. They were not involved in the review process of this article. Otherwise, there was no conflict of interest.
-
AUTHOR CONTRIBUTIONS
Conception or Design: J.A.K., H.J.Y., N.H.K.
Acquisition, analysis, or interpretation of data: J.A.K., M.J.P., E.S., E.R., S.Y.P., D.Y.L., J.K., H.J.Y., N.H.K.
Drafting the work or revising: J.A.K., H.J.Y.
Final approval of the manuscript: J.H.Y., J.A.S., K.M.C., S.H.B., H.J.Y., N.H.K.
-
FUNDING
This work was supported by the Korea Medical Device Development Fund grant funded by the Korea government (the Ministry of Science and ICT, the Ministry of Trade, Industry and Energy, the Ministry of Health & Welfare, the Ministry of Food and Drug Safety) (Project Number: 9991007469, KMDF_PR_20200901_0233).
NOTES
-
Acknowledgements
- None

| Variable | Lancet (n=150) |
LMT-1000 (n=150) |
P valuea,b | ||
|---|---|---|---|---|---|
| Total | 1st attempt | 2nd attempt | |||
| Success rate of puncture | 150 (100) | 149 (99.3) | 118 (78.7) | 31 (20.6) | |
| Total pain score, NRS | 4.0 (3.0–6.0) | 1.0 (0–2.0)a | 1.0 (0–2.0) | 1.0 (0–1.0)b | <0.001 |
| Total satisfaction score, VAS | 5.0 (3.0–7.0) | 9.0 (7.0–10.0)a | 9.0 (7.0–10.0) | 8.0 (5.5–10.0)b | <0.001 |
- 1. American Diabetes Association. 6. Glycemic targets: standards of medical care in diabetes-2021. Diabetes Care 2021;44(Suppl 1):S73-84.ArticlePubMedPDF
- 2. Gao L, Ji L, Su Q, Feng B, Shan Z, Hu R, et al. Impact of structured self-monitoring of blood glucose on the quality of life of insulin-treated Chinese patients with type 2 diabetes mellitus: results from the COMPASS study. Diabetes Res Clin Pract 2016;112:88-93.ArticlePubMed
- 3. Polonsky WH, Fisher L, Schikman CH, Hinnen DA, Parkin CG, Jelsovsky Z, et al. Structured self-monitoring of blood glucose significantly reduces A1C levels in poorly controlled, noninsulin-treated type 2 diabetes: results from the Structured Testing Program study. Diabetes Care 2011;34:262-7.PubMedPMC
- 4. Mannucci E, Antenore A, Giorgino F, Scavini M. Effects of structured versus unstructured self-monitoring of blood glucose on glucose control in patients with non-insulin-treated type 2 diabetes: a meta-analysis of randomized controlled trials. J Diabetes Sci Technol 2018;12:183-9.ArticlePubMedPMCPDF
- 5. Burge MR. Lack of compliance with home blood glucose monitoring predicts hospitalization in diabetes. Diabetes Care 2001;24:1502-3.ArticlePubMedPDF
- 6. Ong WM, Chua SS, Ng CJ. Barriers and facilitators to selfmonitoring of blood glucose in people with type 2 diabetes using insulin: a qualitative study. Patient Prefer Adherence 2014;8:237-46.PubMedPMC
- 7. Yoo WS, Min J, Chung PS, Woo SH. Biochemical and pain comparisons between the laser lancing device and needle lancets for capillary blood sampling: a randomized control trial. Lasers Surg Med 2021;53:316-23.ArticlePubMedPDF
- 8. Haefeli M, Elfering A. Pain assessment. Eur Spine J 2006;15 Suppl 1:S17-24.ArticlePubMedPMCPDF
- 9. Voutilainen A, Pitkaaho T, Kvist T, Vehvilainen-Julkunen K. How to ask about patient satisfaction?: the visual analogue scale is less vulnerable to confounding factors and ceiling effect than a symmetric Likert scale. J Adv Nurs 2016;72:946-57.ArticlePubMedPDF
- 10. Parkes JL, Slatin SL, Pardo S, Ginsberg BH. A new consensus error grid to evaluate the clinical significance of inaccuracies in the measurement of blood glucose. Diabetes Care 2000;23:1143-8.ArticlePubMedPDF
- 11. Stratton IM, Adler AI, Neil HA, Matthews DR, Manley SE, Cull CA, et al. Association of glycaemia with macrovascular and microvascular complications of type 2 diabetes (UKPDS 35): prospective observational study. BMJ 2000;321:405-12.ArticlePubMedPMC
- 12. Ziegler R, Heidtmann B, Hilgard D, Hofer S, Rosenbauer J, Holl R, et al. Frequency of SMBG correlates with HbA1c and acute complications in children and adolescents with type 1 diabetes. Pediatr Diabetes 2011;12:11-7.ArticlePubMed
- 13. Diabetes Control and Complications Trial Research Group, Nathan DM, Genuth S, Lachin J, Cleary P, Crofford O, et al. The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulindependent diabetes mellitus. N Engl J Med 1993;329:977-86.ArticlePubMed
- 14. Fu AZ, Qiu Y, Radican L. Impact of fear of insulin or fear of injection on treatment outcomes of patients with diabetes. Curr Med Res Opin 2009;25:1413-20.ArticlePubMed
- 15. Fonseca V, Hinson J, Pappas A, Waner M, Flock S. An erbium:YAG laser to obtain capillary blood samples without a needle for point-of-care laboratory testing. Arch Pathol Lab Med 1997;121:685-8.PubMed
- 16. Barkana Y, Belkin M. Laser eye injuries. Surv Ophthalmol 2000;44:459-78.ArticlePubMed
REFERENCES
Figure & Data
References
Citations

- Comparison between a laser-lancing device and automatic incision lancet for capillary blood sampling from the heel of newborn infants: a randomized feasibility trial
Chul Kyu Yun, Eui Kyung Choi, Hyung Jin Kim, Jaeyoung Kim, Byung Cheol Park, Kyuhee Park, Byung Min Choi
Journal of Perinatology.2024;[Epub] CrossRef

 KDA
KDA PubReader
PubReader ePub Link
ePub Link Cite
Cite