
- Current
- Browse
- Collections
-
For contributors
- For Authors
- Instructions to authors
- Article processing charge
- e-submission
- For Reviewers
- Instructions for reviewers
- How to become a reviewer
- Best reviewers
- For Readers
- Readership
- Subscription
- Permission guidelines
- About
- Editorial policy
Articles
- Page Path
- HOME > Diabetes Metab J > Volume 35(3); 2011 > Article
-
ReviewDiabetes and Cancer: Is Diabetes Causally Related to Cancer?
- Sunghwan Suh, Kwang-Won Kim
-
Diabetes & Metabolism Journal 2011;35(3):193-198.
DOI: https://doi.org/10.4093/dmj.2011.35.3.193
Published online: June 30, 2011
Division of Endocrinology and Metabolism, Department of Medicine, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Korea.
- Corresponding author: Kwang-Won Kim. Division of Endocrinology and Metabolism, Department of Medicine, Samsung Medical Center, Sungkyunkwan University School of Medicine, 50 Irwon-dong, Gangnam-gu, Seoul 135-710, Korea. kw1234@skku.edu
Copyright © 2011 Korean Diabetes Association
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/3.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
ABSTRACT
- Diabetes mellitus is a serious and growing health problem worldwide and is associated with severe acute and chronic complications. Moreover, epidemiologic evidence suggests that people with diabetes are at significantly higher risk for many forms of cancer. Several studies indicate an association between diabetes and the risk of liver, pancreas, endometrium, colon/rectum, breast, and bladder cancer. Mortality is also moderately increased in subjects with diabetes. Common risk factors such as age, obesity, physical inactivity and smoking may contribute to increased cancer risk in diabetic patients. Hyperinsulinemia most likely favors cancer in diabetic patients as insulin is a growth factor with pre-eminent metabolic as well as mitogenic effects, and its action in malignant cells is favored by mechanisms acting at both the receptor and post-receptor level. The effect of diabetes treatment drugs, aside from metformin, on cancer is not conclusive. In order to fight the perfect storm of diabetes and cancer, strategies to promote primary prevention and early detection of these conditions are urgently needed.
- Diabetes mellitus (DM) is a serious and growing health problem worldwide and is associated with severe acute and chronic complications. Today, 250 million people live with diabetes globally, and this figure is expected to reach 366 million in 2030 [1]. Therefore, if diabetes is associated with an increase in the risk of cancer, this may have a tremendous impact on health worldwide. The industrialization and economic growth accompanied by the so-called 'westernization' of lifestyle, characterized by a high-calorie diet, obesity, and physical inactivity may explain this diabetes epidemic. As a result of this change, the mortality of lifestyle-related diseases such as cancer, diabetes, and cardiovascular disease has increased in many countries including South Korea. Worldwide, cancer is the 2nd and diabetes is the 12th leading cause of death [2]. According to the recent Statistics Korea report for 2009 [3], cancer is the leading cause of death and DM is the 5th most common cause of death.
- Epidemiologic evidence suggests that people with diabetes are at significantly higher risk for many forms of cancer [4-7]. Park et al. [8] found that death by malignancy was markedly increased (from 4.7% to 21.9%) in Korean type 2 diabetes patients during the past 10 years. Type 2 diabetes and cancer share many risk factors, but potential biologic links between the two diseases are not completely understood.
- In this review, we will discuss Korean and foreign evidences of an association between diabetes and cancer, and the possible mechanisms involved. The link between diabetes treatment and cancer risk will also be reviewed.
INTRODUCTION
- Many longitudinal and case-control studies, often pooled in meta-analyses, have explored the association between diabetes and a large array of different neoplasms. Recently, the results of several studies have been combined for a meta-analytic study [4,9] and the results are shown in Table 1. The relative risks imparted by diabetes are greatest (about twofold or higher) for cancers of the liver, pancreas, and endometrium, and lesser (about 1.2 to 1.5 fold) for cancers of the colon and rectum, breast, and bladder. Other cancers (such as lung) do not appear to be associated with diabetes, and the evidence for some (e.g., kidney, non-Hodgkin's lymphoma) is inconclusive. Diabetes is associated with a lower risk of prostate cancer only.
- Previous meta-analyses are mainly derived from Western populations. However, a 10-year prospective cohort study of 1.3 million Koreans aged 30 to 95 years [10] found that cancer incidence is generally elevated for persons with diabetes or an elevated fasting serum glucose level greater than 125 mg/dL (6.9 mmol/L) compared with those without hyperglycemia. The association was strongest for pancreatic cancer, comparing the highest and lowest strata in men (hazard ratio [HR], 1.91; 95% confidence interval [CI], 1.52 to 2.41) and in women (HR, 2.05; 95% CI, 1.43 to 2.93). Significant associations were also found for cancers of the esophagus, liver, and colon/rectum in men and of the liver and cervix in women. There were also significant trends with glucose level and cancers of the esophagus, colon/rectum, liver, pancreas, and bile duct in men and of the liver and pancreas in women. We also have reported that 30% of pancreatic cancer patients have diabetes [11]. Findings similar to those of the Korean cohort study were seen in the Japan Pubic Health Center-based Prospective (JPHC) study of 110,000 Japanese aged 40 to 60 years [12].
- The large majority of the epidemiologic data on cancer incidence and mortality has been obtained from type 2 diabetic patients. Because of the different physiology between the two subtypes of diabetes, these findings cannot be extended to type 1 diabetic patients. However, the risk of cancer among patients with type 1 diabetes (T1DM) has been investigated in two cohort studies. A Swedish study of over 29,000 T1DM patients revealed an overall 20% increase in the risk of cancer [13]. In particular, the risks of stomach, uterine cervix, and endometrium neoplasm were almost doubled. A UK study involving 28,900 individuals showed that the risk of ovarian cancer and the mortality associated with this neoplasm was more than two-fold higher in subjects with T1DM than in controls [14]. No other significant associations were found.
INCREASED CANCER INCIDENCE IN DIABETIC PATIENTS
- Besides its role as an independent risk factor for the development of several tumors, diabetes can also have impact on cancer prognosis. Several studies have documented increased cancer mortality in subjects with diabetes. A recent meta-analysis of 23 studies comparing overall survival in cancer patients with and without preexisting diabetes showed that diabetes was associated with an increased mortality HR of 1.41 (95% CI, 1.28 to 1.55) compared with normoglycemic individuals across all cancer types [15]. Subgroup analyses by cancer type showed an increased risk for cancers of the endometrium (HR, 1.76; 95% CI, 1.34 to 2.31), breast (HR, 1.61; 95% CI, 1.46 to 1.78), and colorectum (HR, 1.32; 95% CI, 1.24 to 1.41). A cohort study including Korean individuals [10] of both genders revealed a linear trend of increasing mortality with increasing fasting serum glucose levels, even in the non-diabetic range. The linear association between fasting serum glucose levels and cancer mortality was particularly evident for malignancies of the pancreas, colon/rectum, liver, esophagus, and biliary tract among men and the pancreas, liver, and uterine cervix in women.
INCREASED CANCER MORTALITY IN DIABETIC PATIENTS
- Diabetes and cancer represent common health concerns, and they often coexist in the same individuals. Overall, 8% to 18% of individuals suffering from cancer also have diabetes, and prevalence rates vary according to tumor sites [16].
- Age
- Over 60% of cancer diagnoses are made in individuals aged 65 years or more [17]; since the prevalence of diabetes reaches 17% in this age class, the coexistence of diabetes and cancer is destined to raise as life expectancy increases.
- Obesity
- Type 2 diabetes is strongly related to overweight and obesity, two conditions associated with an increased risk of several cancers [18]. Cancers most consistently associated with overweight and obesity are breast (in postmenopausal women), colon/rectum, endometrium, pancreas, adenocarcinoma of the esophagus, kidney, gallbladder, and liver. Moreover, obesity is associated with higher cancer incidence and mortality [19,20].
- Physical inactivity
- Evidence from observational epidemiologic studies consistently shows that higher levels of physical activity are associated with a lower risk of the colon, postmenopausal breast, and endometrial cancer [21,22]. Prevention of diabetes with increased physical activity has been proven by numerous trials [23-26].
- Smoking
- It is estimated that worldwide, cigarette smoking accounts for 71% of all trachea, bronchus, and lung cancer deaths [27]. Other cancers strongly associated with smoking are cancers of the larynx, upper digestive tract, bladder, kidney, pancreas, liver, stomach, uterine cervix, and leukemia. Studies suggest that smoking is also an independent risk factor for the development of diabetes [28,29].
COMMON RISK FACTORS FOR BOTH CANCER AND DIABETES
- The role of insulin in promoting cancer growth was first recognized by studies in experimental animals as early as 1972 [30,31]. Diabetes is generally characterized by hyperglycemia and hyperinsulinemia, which are often coupled with a reduced metabolic effect of insulin (insulin resistance) in peripheral tissues. Chronic hyperinsulinemia, however, is a possible factor favoring cancer initiation and progression in diabetic patients due to the mitogenic effect of insulin, which has been reviewed in detail [32]. In brief, an increase in insulin levels leads to a decrease in the liver synthesis and blood levels of insulin-like growth factor binding protein 1 (IGFBP1), and is associated with a decrease in IGFBP2 in the blood. These effects in turn result in an increase in bioavailable IGF1. Insulin and IGF1 signal through insulin receptors and IGF1 receptors, respectively, to promote cellular proliferation and inhibit apoptosis in many tissue types. These effects might contribute to cancerogenesis.
- Many cancer cells have increased insulin receptor (IR) content [33]. In malignant cells, the expression of the isoform (IR-A) is predominant, and its activation elicits more mitogenetic than metabolic effects [34]. By binding to the overexpressed IR-A, insulin may favor cancer progression and facilitate the growth of tumors that would otherwise have likely remained clinically irrelevant.
- Insulin mitogenic activity might be enhanced at the cellular level by post-receptor molecular mechanisms, including insulin (or its synthetic analogs) residence time on the receptor [35] and the intracellular up-regulation of the insulin mitogenic pathway.
POSSIBLE MECHANISMS UNDERLYING DIABETES AND CANCER
- Most diabetic patients are treated for years or decades with a variety of drugs. The potential role of these drugs in favoring cancer is unclear, but is most likely minor, if any. The data are not conclusive because the large majority of diabetic patients change the drug dosage and/or type many times during the course of the disease. Moreover, many are treated with more than one drug simultaneously. As a result, this issue is not well-studied epidemiologically, and evidence is weak, inconclusive and controversial. The debate about the potential risk of developing cancer associated with insulin use has been ignited by the publication of four observational studies [36-39] in 2009. However, randomized clinical trial data from an open-label 5-year trial of insulin glargine versus NPH insulin did not find any evidence of excess cancer risk with insulin glargine [40]. Due to the methodological limitations of previous studies, which have been broadly debated [41-43], a clear relationship between use of insulin glargine and increased risk of cancer cannot be established.
- On the contrary, a mounting body of evidence suggests that metformin may reduce cancer risk [36,44-47] or mortality [48] in diabetic patients. There is probably a dual mechanism for the anticancer effect of metformin. In addition to the lowering of circulating levels of insulin, metformin stimulates expression of AMPK, leading to the rapid inhibition of cellular protein synthesis and growth [49,50].
DIABETES TREATMENT AND CANCER
- Descriptive and analytical evidence obtained to date suggest that cancer risk and cancer mortality are increased in diabetic patients, providing more evidence for some site-specific cancers. The increase in the risk of cancer is likely related to the interplay between obesity, hyperinsulinemia and hyperglycemia. Improved glycemic control guidelines with a wide prescription of statin and aspirin have reduced death from vascular complications and diabetes itself. As a result, death by cancer is rising steeply although cardiovascular disease and infection are still the leading cause of the death. The impressive rate of increase in the incidence of both diabetes and obesity will pose serious problems to many countries including South Korea. In order to fight the perfect storm of diabetes and cancer, preventive strategies to promote primary prevention and early detection of these conditions are urgently needed.
CONCLUSION
- 1. Wild S, Roglic G, Green A, Sicree R, King H. Global prevalence of diabetes: estimates for the year 2000 and projections for 2030. Diabetes Care 2004;27:1047-1053. ArticlePubMedPDF
- 2. Lopez AD, Mathers CD, Ezzati M, Jamison DT, Murray CJ. Global and regional burden of disease and risk factors, 2001: systematic analysis of population health data. Lancet 2006;367:1747-1757. ArticlePubMed
- 3. Statistics Korea: Statistics of Cause of Death Available from: http://www.kostat.go.kr. (updated 2010 Sep 9).
- 4. Vigneri P, Frasca F, Sciacca L, Pandini G, Vigneri R. Diabetes and cancer. Endocr Relat Cancer 2009;16:1103-1123. ArticlePubMed
- 5. Nicolucci A. Epidemiological aspects of neoplasms in diabetes. Acta Diabetol 2010;47:87-95. ArticlePubMedPDF
- 6. Tsugane S, Inoue M. Insulin resistance and cancer: epidemiological evidence. Cancer Sci 2010;101:1073-1079. ArticlePubMed
- 7. Giovannucci E, Harlan DM, Archer MC, Bergenstal RM, Gapstur SM, Habel LA, Pollak M, Regensteiner JG, Yee D. Diabetes and cancer: a consensus report. Diabetes Care 2010;33:1674-1685. ArticlePubMedPMC
- 8. Park SK, Park MK, Suk JH, Kim MK, Kim YK, Kim IJ, Kang YH, Lee KJ, Lee HS, Lee CW, Kim BH, Lee KI, Kim MK, Kim DK. Cause-of-death trends for diabetes mellitus over 10 years. Korean Diabetes J 2009;33:65-72.Article
- 9. Nicolucci A. Epidemiological aspects of neoplasms in diabetes. Acta Diabetol 2010;47:87-95. ArticlePubMedPDF
- 10. Jee SH, Ohrr H, Sull JW, Yun JE, Ji M, Samet JM. Fasting serum glucose level and cancer risk in Korean men and women. JAMA 2005;293:194-202. ArticlePubMed
- 11. Park YJ, Kim KW, Oh EY, Min YK, Lee MS, Lee MK, Lee JK, Lee KT, Kim YI, Choi YH. Prevalence of diabetes mellitus in pancreatic cancer patients. J Korean Diabetes Assoc 2001;25:316-322.
- 12. Inoue M, Iwasaki M, Otani T, Sasazuki S, Noda M, Tsugane S. Diabetes mellitus and the risk of cancer: results from a large-scale population-based cohort study in Japan. Arch Intern Med 2006;166:1871-1877. ArticlePubMed
- 13. Zendehdel K, Nyren O, Ostenson CG, Adami HO, Ekbom A, Ye W. Cancer incidence in patients with type 1 diabetes mellitus: a population-based cohort study in Sweden. J Natl Cancer Inst 2003;95:1797-1800. ArticlePubMed
- 14. Swerdlow AJ, Laing SP, Qiao Z, Slater SD, Burden AC, Botha JL, Waugh NR, Morris AD, Gatling W, Gale EA, Patterson CC, Keen H. Cancer incidence and mortality in patients with insulin-treated diabetes: a UK cohort study. Br J Cancer 2005;92:2070-2075. ArticlePubMedPMCPDF
- 15. Barone BB, Yeh HC, Snyder CF, Peairs KS, Stein KB, Derr RL, Wolff AC, Brancati FL. Long-term all-cause mortality in cancer patients with preexisting diabetes mellitus: a systematic review and meta-analysis. JAMA 2008;300:2754-2764. ArticlePubMedPMC
- 16. Ko C, Chaudhry S. The need for a multidisciplinary approach to cancer care. J Surg Res 2002;105:53-57. ArticlePubMed
- 17. Centers for Disease Control and Prevention (CDC). Cancer survivorship--United States, 1971-2001. MMWR Morb Mortal Wkly Rep 2004;53:526-529. PubMed
- 18. Calle EE, Rodriguez C, Walker-Thurmond K, Thun MJ. Overweight, obesity, and mortality from cancer in a prospectively studied cohort of U.S. adults. N Engl J Med 2003;348:1625-1638. ArticlePubMed
- 19. Adami HO, Trichopoulos D. Obesity and mortality from cancer. N Engl J Med 2003;348:1623-1624. ArticlePubMed
- 20. Vigneri P, Frasca F, Sciacca L, Frittitta L, Vigneri R. Obesity and cancer. Nutr Metab Cardiovasc Dis 2006;16:1-7. ArticlePubMed
- 21. Friedenreich CM, Orenstein MR. Physical activity and cancer prevention: etiologic evidence and biological mechanisms. J Nutr 2002;132(11 Suppl):3456S-3464S. ArticlePubMed
- 22. Lee IM. Physical activity and cancer prevention: data from epidemiologic studies. Med Sci Sports Exerc 2003;35:1823-1827. ArticlePubMed
- 23. Knowler WC, Barrett-Connor E, Fowler SE, Hamman RF, Lachin JM, Walker EA, Nathan DM. Diabetes Prevention Program Research Group. Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. N Engl J Med 2002;346:393-403. ArticlePubMedPMC
- 24. Pan XR, Li GW, Hu YH, Wang JX, Yang WY, An ZX, Hu ZX, Lin J, Xiao JZ, Cao HB, Liu PA, Jiang XG, Jiang YY, Wang JP, Zheng H, Zhang H, Bennett PH, Howard BV. Effects of diet and exercise in preventing NIDDM in people with impaired glucose tolerance. The Da Qing IGT and Diabetes Study. Diabetes Care 1997;20:537-544. ArticlePubMedPDF
- 25. Tuomilehto J, Lindstrom J, Eriksson JG, Valle TT, Hamalainen H, Ilanne-Parikka P, Keinanen-Kiukaanniemi S, Laakso M, Louheranta A, Rastas M, Salminen V, Uusitupa M. Finnish Diabetes Prevention Study Group. Prevention of type 2 diabetes mellitus by changes in lifestyle among subjects with impaired glucose tolerance. N Engl J Med 2001;344:1343-1350. ArticlePubMed
- 26. Kosaka K, Noda M, Kuzuya T. Prevention of type 2 diabetes by lifestyle intervention: a Japanese trial in IGT males. Diabetes Res Clin Pract 2005;67:152-162. ArticlePubMed
- 27. Mackay J, Ericksen M, Shafey O. The cancer atlas. 2006. Atlanta: American Cancer Society.
- 28. Foy CG, Bell RA, Farmer DF, Goff DC Jr, Wagenknecht LE. Smoking and incidence of diabetes among U.S. adults: findings from the Insulin Resistance Atherosclerosis Study. Diabetes Care 2005;28:2501-2507. PubMed
- 29. Willi C, Bodenmann P, Ghali WA, Faris PD, Cornuz J. Active smoking and the risk of type 2 diabetes: a systematic review and meta-analysis. JAMA 2007;298:2654-2664. ArticlePubMed
- 30. Heuson JC, Legros N. Influence of insulin deprivation on growth of the 7,12-dimethylbenz(a)anthracene-induced mammary carcinoma in rats subjected to alloxan diabetes and food restriction. Cancer Res 1972;32:226-232. PubMed
- 31. Heuson JC, Legros N, Heimann R. Influence of insulin administration on growth of the 7,12-dimethylbenz(a)anthracene-induced mammary carcinoma in intact, oophorectomized, and hypophysectomized rats. Cancer Res 1972;32:233-238. PubMed
- 32. Calle EE, Kaaks R. Overweight, obesity and cancer: epidemiological evidence and proposed mechanisms. Nat Rev Cancer 2004;4:579-591. ArticlePubMedPDF
- 33. Papa V, Pezzino V, Costantino A, Belfiore A, Giuffrida D, Frittitta L, Vannelli GB, Brand R, Goldfine ID, Vigneri R. Elevated insulin receptor content in human breast cancer. J Clin Invest 1990;86:1503-1510. ArticlePubMedPMC
- 34. Frasca F, Pandini G, Scalia P, Sciacca L, Mineo R, Costantino A, Goldfine ID, Belfiore A, Vigneri R. Insulin receptor isoform A, a newly recognized, high-affinity insulin-like growth factor II receptor in fetal and cancer cells. Mol Cell Biol 1999;19:3278-3288. ArticlePubMedPMCPDF
- 35. De Meyts P, Christoffersen CT, Urso B, Wallach B, Gronskov K, Yakushiji F, Shymko RM. Role of the time factor in signaling specificity: application to mitogenic and metabolic signaling by the insulin and insulin-like growth factor-I receptor tyrosine kinases. Metabolism 1995;44(10 Suppl 4):2-11. ArticlePubMed
- 36. Currie CJ, Poole CD, Gale EA. The influence of glucose-lowering therapies on cancer risk in type 2 diabetes. Diabetologia 2009;52:1766-1777. ArticlePubMedPDF
- 37. Jonasson JM, Ljung R, Talback M, Haglund B, Gudbjornsdottir S, Steineck G. Insulin glargine use and short-term incidence of malignancies-a population-based follow-up study in Sweden. Diabetologia 2009;52:1745-1754. ArticlePubMedPDF
- 38. Colhoun HM. SDRN Epidemiology Group. Use of insulin glargine and cancer incidence in Scotland: a study from the Scottish Diabetes Research Network Epidemiology Group. Diabetologia 2009;52:1755-1765. ArticlePubMedPMC
- 39. Hemkens LG, Grouven U, Bender R, Gunster C, Gutschmidt S, Selke GW, Sawicki PT. Risk of malignancies in patients with diabetes treated with human insulin or insulin analogues: a cohort study. Diabetologia 2009;52:1732-1744. ArticlePubMedPMC
- 40. Rosenstock J, Fonseca V, McGill JB, Riddle M, Halle JP, Hramiak I, Johnston P, Davis M. Similar risk of malignancy with insulin glargine and neutral protamine Hagedorn (NPH) insulin in patients with type 2 diabetes: findings from a 5 year randomised, open-label study. Diabetologia 2009;52:1971-1973. ArticlePubMedPMC
- 41. Pollak M, Russell-Jones D. Insulin analogues and cancer risk: cause for concern or cause célèbre? Int J Clin Pract 2010;64:628-636. ArticlePubMed
- 42. Gerstein HC. Does insulin therapy promote, reduce, or have a neutral effect on cancers? JAMA 2010;303:446-447. ArticlePubMed
- 43. Smith U, Gale EA. Does diabetes therapy influence the risk of cancer? Diabetologia 2009;52:1699-1708. ArticlePubMedPDF
- 44. Monami M, Lamanna C, Balzi D, Marchionni N, Mannucci E. Sulphonylureas and cancer: a case-control study. Acta Diabetol 2009;46:279-284. ArticlePubMedPDF
- 45. Evans JM, Donnelly LA, Emslie-Smith AM, Alessi DR, Morris AD. Metformin and reduced risk of cancer in diabetic patients. BMJ 2005;330:1304-1305. ArticlePubMedPMC
- 46. Bowker SL, Majumdar SR, Veugelers P, Johnson JA. Increased cancer-related mortality for patients with type 2 diabetes who use sulfonylureas or insulin. Diabetes Care 2006;29:254-258. ArticlePubMedPDF
- 47. Wright JL, Stanford JL. Metformin use and prostate cancer in Caucasian men: results from a population-based case-control study. Cancer Causes Control 2009;20:1617-1622. ArticlePubMedPMC
- 48. Landman GW, Kleefstra N, van Hateren KJ, Groenier KH, Gans RO, Bilo HJ. Metformin associated with lower cancer mortality in type 2 diabetes: ZODIAC-16. Diabetes Care 2010;33:322-326. PubMed
- 49. Cazzaniga M, Bonanni B, Guerrieri-Gonzaga A, Decensi A. Is it time to test metformin in breast cancer clinical trials? Cancer Epidemiol Biomarkers Prev 2009;18:701-705. ArticlePubMedPDF
- 50. Goodwin PJ, Ligibel JA, Stambolic V. Metformin in breast cancer: time for action. J Clin Oncol 2009;27:3271-3273. ArticlePubMed
REFERENCES
Table 1Meta-analysis on the relative risk (RR) for cancer in different origins of diabetic patients (Modified from Vigneri P, et al. Endocr Relat Cancer 2009;16:1103-23, with permission from Society for Endocrinology) [4]
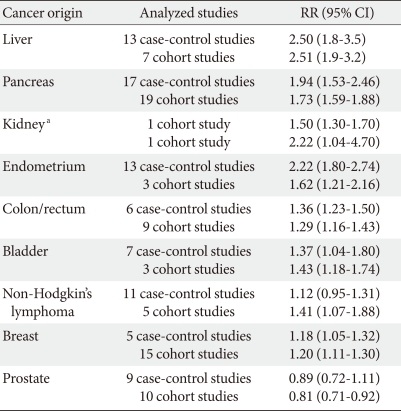

Figure & Data
References
Citations
Citations to this article as recorded by 

- Proinsulin C-peptide inhibits high glucose-induced migration and invasion of ovarian cancer cells
Eun-Bin Kim, Hye-Yoon Jeon, Yung-Taek Ouh, Ah-Jun Lee, Chan-Hee Moon, Sung Hun Na, Kwon-Soo Ha
Biomedicine & Pharmacotherapy.2024; 172: 116232. CrossRef - Glycemic traits and colorectal cancer survival in a cohort of South Korean patients: A Mendelian randomization analysis
So Yon Jun, Sooyoung Cho, Min Jung Kim, Ji Won Park, Seung‐Bum Ryoo, Seung Yong Jeong, Kyu Joo Park, Aesun Shin
Cancer Medicine.2024;[Epub] CrossRef - The Association of Glycemic Index, Glycemic Load, and Daily Carbohydrates Intake with the Risk of Hepatocellular Carcinoma: A Systematic Review and Meta-Analysis
Long-Shan Yang, Lun-Jie Yan, Guang-Xiao Meng, Zi-Niu Ding, Sheng-Yu Yao, Hai-Chao Li, Zhao-Ru Dong, Zhi-Qiang Chen, Jian-Guo Hong, Tao Li
Nutrition and Cancer.2023; 75(2): 461. CrossRef - 4. Comprehensive Medical Evaluation and Assessment of Comorbidities:Standards of Care in Diabetes—2023
Nuha A. ElSayed, Grazia Aleppo, Vanita R. Aroda, Raveendhara R. Bannuru, Florence M. Brown, Dennis Bruemmer, Billy S. Collins, Kenneth Cusi, Marisa E. Hilliard, Diana Isaacs, Eric L. Johnson, Scott Kahan, Kamlesh Khunti, Jose Leon, Sarah K. Lyons, Mary Lo
Diabetes Care.2023; 46(Supplement): s49. CrossRef - TCF7L2, CASC8, and GREM1 polymorphism and colorectal cancer in south-eastern Romanian population
Anca Florentina Mitroi, Nicoleta Leopa, Eugen Dumitru, Andrei Dumitru, Cristina Tocia, Ioana Popescu, Adrian Mitroi, Răzvan Cătălin Popescu
Medicine.2023; 102(7): e33056. CrossRef - New benzimidazole‐oxadiazole derivatives: Synthesis, α‐glucosidase, α‐amylase activity, and molecular modeling studies as potential antidiabetic agents
Ulviye Acar Çevik, Ismail Celik, Leyla Paşayeva, Hanifa Fatullayev, Hayrani E. Bostancı, Yusuf Özkay, Zafer A. Kaplancıklı
Archiv der Pharmazie.2023;[Epub] CrossRef - Synthesis, α-amylase and α-glucosidase inhibition and molecular docking studies of indazole derivatives
Muhammad Nawaz, Muhammad Taha, Faiza Qureshi, Nisar Ullah, Manikandan Selvaraj, Sumaira Shahzad, Sridevi Chigurupati, Samar A. Abubshait, Tauqir Ahmad, Sampath Chinnam, Soleiman Hisaindee
Journal of Biomolecular Structure and Dynamics.2022; 40(21): 10730. CrossRef - Association between Alzheimer's disease and risk of cancer: A retrospective cohort study in Shanghai, China
Ru‐Jing Ren, Qiang Huang, Gang Xu, Kai Gu, Eric B. Dammer, Chun‐Fang Wang, Xin‐Yi Xie, Wen Chen, Zhen‐Yi Shao, Sheng‐Di Chen, Gang Wang
Alzheimer's & Dementia.2022; 18(5): 924. CrossRef - 4. Comprehensive Medical Evaluation and Assessment of Comorbidities: Standards of Medical Care in Diabetes—2022
Diabetes Care.2022; 45(Supplement): S46. CrossRef - A Novel Metabolic Reprogramming Strategy for the Treatment of Diabetes‐Associated Breast Cancer
Qiongyu Hao, Zhimin Huang, Qun Li, Dingxie Liu, Piwen Wang, Kun Wang, Jieqing Li, Wei Cao, Wenhong Deng, Ke Wu, Rui Su, Zhongmin Liu, Jay Vadgama, Yong Wu
Advanced Science.2022;[Epub] CrossRef - Seroreactivity Against Tyrosine Phosphatase PTPRN Links Type 2 Diabetes and Colorectal Cancer and Identifies a Potential Diagnostic and Therapeutic Target
María Garranzo-Asensio, Guillermo Solís-Fernández, Ana Montero-Calle, José Manuel García-Martínez, Maria Carmen Fiuza, Pilar Pallares, Nuria Palacios-Garcia, Custodia García-Jiménez, Ana Guzman-Aranguez, Rodrigo Barderas
Diabetes.2022; 71(3): 497. CrossRef - Doxorubicin-induced apoptosis enhances monocyte infiltration and adverse cardiac remodeling in diabetic animals
Chandrakala Aluganti Narasimhulu, Dinender K. Singla
Canadian Journal of Physiology and Pharmacology.2022; 100(5): 441. CrossRef - Sleep Disruption and Cancer: Chicken or the Egg?
Adrian Berisha, Kyle Shutkind, Jeremy C. Borniger
Frontiers in Neuroscience.2022;[Epub] CrossRef - A comparative study of phytochemical, antioxidant, anticarcinogenic, and antidiabetic potential of coriander (Coriandrum sativum L.): Microgreen and mature plant
G. M. Dhakshayani, S. Janaki Alias Priya
Foods and Raw Materials.2022; : 283. CrossRef - Influence of type II diabetes mellitus on postoperative complications following colorectal cancer surgery
Răzvan Cătălin Popescu, Nicoleta Leopa, Eugen Dumitru, Anca Mitroi, Cristina Tocia, Andrei Dumitru, Costel Brînzan, Florin Botea
Experimental and Therapeutic Medicine.2022;[Epub] CrossRef - Diabetes Mellitus as a Risk Factor for Different Types of Cancers: A Systematic Review
Saud S Alharbi
Clinical Cancer Investigation Journal.2022; 11(4): 19. CrossRef - Survival of Colorectal Cancer Patients With Diabetes Mellitus: A Meta-Analysis
Fausto Petrelli, Michele Ghidini, Emanuele Rausa, Antonio Ghidini, Mary Cabiddu, Karen Borgonovo, Mara Ghilardi, Maria Chiara Parati, Filippo Pietrantonio, Paolo Sganzerla, Antonio Carlo Bossi
Canadian Journal of Diabetes.2021; 45(2): 186. CrossRef - 4. Comprehensive Medical Evaluation and Assessment of Comorbidities: Standards of Medical Care in Diabetes—2021
Diabetes Care.2021; 44(Supplement): S40. CrossRef - High glucose‐ROS conditions enhance the progression in cholangiocarcinoma via upregulation of MAN2A2 and CHD8
Unchalee Thonsri, Sopit Wongkham, Chaisiri Wongkham, Shinjiro Hino, Mitsuyoshi Nakao, Sittiruk Roytrakul, Tomoaki Koga, Wunchana Seubwai
Cancer Science.2021; 112(1): 254. CrossRef - On the meaning of and relationship between dragon-kings, black swans and related concepts
Ingrid Glette-Iversen, Terje Aven
Reliability Engineering & System Safety.2021; 211: 107625. CrossRef - Colonoscopy and Risk of Colorectal Cancer in Patients With Nonalcoholic Fatty Liver Disease: A Retrospective Territory‐Wide Cohort Study
Xinrong Zhang, Vincent Wai‐Sun Wong, Terry Cheuk‐Fung Yip, Yee‐Kit Tse, Lilian Yan Liang, Vicki Wing‐Ki Hui, Guan‐Lin Li, Henry Lik‐Yuen Chan, Grace Lai‐Hung Wong
Hepatology Communications.2021; 5(7): 1212. CrossRef - Metabolic profiling analysis for clinical urine of colorectal cancer
Wu Ning, Nan Qiao, Xiyin Zhang, Dongpo Pei, Wenyue Wang
Asia-Pacific Journal of Clinical Oncology.2021; 17(4): 403. CrossRef - Metformin suppresses breast cancer growth via inhibition of cyclooxygenase‑2
Bin Shi, Xinyu Hu, Huimin He, Wenzheng Fang
Oncology Letters.2021;[Epub] CrossRef - Characteristics that influence the diagnosis and treatment of diabetes in geriatric patients over 75
Angelo Scuteri
Journal of Gerontology and Geriatrics.2021; 69(4): 238. CrossRef - Need of integrated management of type ii diabetes mellitus as a serious risk factor in modifying outcomes in cancer management: A literature review
YogeshNarayan Bendale, Vineeta Bendale, Pravin Gund, Avinash Kadam
Indian Journal of Ayurveda and Integrative Medicine KLEU.2021; 2(2): 50. CrossRef - Metformin use reduced the overall risk of cancer in diabetic patients: A study based on the Korean NHIS-HEALS cohort
Ye-Seul Kim, Eun-A. Choi, Jae-woo Lee, Yonghwan Kim, Hyo-Sun You, Ye-Eun Han, Hyeong-Seop Kim, Yoon-Jong Bae, Hee-Taik Kang, Joungyoun Kim
Nutrition, Metabolism and Cardiovascular Diseases.2020; 30(10): 1714. CrossRef - No clear associations of adult BMI and diabetes mellitus with non-muscle invasive bladder cancer recurrence and progression
Jelle Evers, Anne J. Grotenhuis, Katja K. H. Aben, Lambertus A. L. M. Kiemeney, Alina Vrieling, Ernest K. Amankwah
PLOS ONE.2020; 15(3): e0229384. CrossRef - Prevalence of diabetes mellitus as well as cardiac and other main comorbidities in a representative sample of the adult Greek population in comparison with the general population
Anastasios Tentolouris, Ioanna Eleftheriadou, Kostas Athanasakis, John Kyriopoulos, Diamantis I. Tsilimigras, Pinelopi Grigoropoulou, John Doupis, Nikolaos Tentolouris
Hellenic Journal of Cardiology.2020; 61(1): 15. CrossRef - A clinical prediction nomogram to assess risk of colorectal cancer among patients with type 2 diabetes
Lu-Huai Feng, Tingting Su, Kun-Peng Bu, Shuang Ren, Zhenhua Yang, Cheng-En Deng, Bi-Xun Li, Wei-Yuan Wei
Scientific Reports.2020;[Epub] CrossRef - Cohort Profile: The Maule Cohort (MAUCO)
Catterina Ferreccio, Andrea Huidobro, Sandra Cortés, Claudia Bambs, Pablo Toro, Vanessa Van De Wyngard, Johanna Acevedo, Fabio Paredes, Pía Venegas, Hugo Verdejo, Ximena Oyarzún-González, Paz Cook, Pablo F Castro, Claudia Foerster, Claudio Vargas, Jill Ko
International Journal of Epidemiology.2020; 49(3): 760. CrossRef - Gastric Cancer Heterogeneity and Clinical Outcomes
Rachel E. Sexton, Mohammed Najeeb Al Hallak, Md. Hafiz Uddin, Maria Diab, Asfar S. Azmi
Technology in Cancer Research & Treatment.2020; 19: 153303382093547. CrossRef - Temporal trajectories of accompanying comorbidities in patients with type 2 diabetes: a Korean nationwide observational study
Eugene Jeong, Namgi Park, Yujeong Kim, Ja Young Jeon, Wou Young Chung, Dukyong Yoon
Scientific Reports.2020;[Epub] CrossRef - Utility of KRAS Gene and Clinicopathological Features in the Assessment of the Risk of Type 2 Diabetes in the Etiology of Colon Cancer
Wedad Saeed Al-Qahtani, Ebtesam Al-Olayan, Fatimah Gh. Albani, Rania Saad Suliman, Nada Hamad Aljarba, E.M. Al-Humaidhi, Alanood S. Almurshedi, Dalia Mostafa Domiaty, Manal Abdullah Alduwish, Aljohara M. Al-Otaibi, Abdelbaset Mohamed Elasbali, Hussain Gad
Global Medical Genetics.2020; 07(02): 035. CrossRef - Glycation Leads to Increased Polysialylation and Promotes the Metastatic Potential of Neuroblastoma Cells
Maximilian Scheer, Kaya Bork, Frieder Simon, Manimozhi Nagasundaram, Rüdiger Horstkorte, Vinayaga Srinivasan Gnanapragassam
Cells.2020; 9(4): 868. CrossRef - Site-specific cancer risk in patients with type 2 diabetes: a nationwide population-based cohort study in Korea
Suk Kyeong Kim, Ju-Young Jang, Dong-Lim Kim, Young A Rhyu, Suh Eun Lee, Seung-Hyun Ko, Kyungdo Han, Kee-Ho Song
The Korean Journal of Internal Medicine.2020; 35(3): 641. CrossRef - Synthesis, α-glucosidase inhibition and antioxidant activity of the 7-carbo–substituted 5-bromo-3-methylindazoles
Malose J. Mphahlele, Nontokozo M. Magwaza, Samantha Gildenhuys, Itumeleng B. Setshedi
Bioorganic Chemistry.2020; 97: 103702. CrossRef - 4. Comprehensive Medical Evaluation and Assessment of Comorbidities: Standards of Medical Care in Diabetes—2020
Diabetes Care.2020; 43(Supplement): S37. CrossRef - 4. Comprehensive Medical Evaluation and Assessment of Comorbidities:Standards of Medical Care in Diabetes—2019
Diabetes Care.2019; 42(Supplement): S34. CrossRef - Diabetes‐mediated promotion of colon mucosa carcinogenesis is associated with mitochondrial dysfunction
Laura Del Puerto‐Nevado, Aranzazu Santiago‐Hernandez, Sonia Solanes‐Casado, Nieves Gonzalez, Marta Ricote, Marta Corton, Isabel Prieto, Sebastian Mas, Ana Belen Sanz, Oscar Aguilera, Carmen Gomez‐Guerrero, Carmen Ayuso, Alberto Ortiz, Federico Rojo, Jesus
Molecular Oncology.2019; 13(9): 1887. CrossRef - Diabetes and Cancer: Cancer Should Be Screened in Routine Diabetes Assessment
Sunghwan Suh, Kwang-Won Kim
Diabetes & Metabolism Journal.2019; 43(6): 733. CrossRef - Lorcaserin for prevention and remission of type 2 diabetes mellitus in people with overweight or obesity: protocol for a systematic review and meta-analysis
Hai Zeng, Meng Luo, Zunjiang Li, Junru Wen, Guoxin He, Yuelin Jin, Wenbin Fu, Peng Zhou
BMJ Open.2019; 9(7): e029426. CrossRef - Disseminated Well-Differentiated Gastro-Entero-Pancreatic Tumors Are Associated with Metabolic Syndrome
Santos, Castro, Antunes, Henrique, Cardoso, Monteiro
Journal of Clinical Medicine.2019; 8(9): 1479. CrossRef - Effects of Aspirin or Clopidogrel on Colorectal Cancer Chemoprevention in Patients with Type 2 Diabetes Mellitus
Yi-Chun Kuan, Kuang-Wei Huang, Cheng-Li Lin, Jiing-Chyuan Luo, Chia-Hung Kao
Cancers.2019; 11(10): 1468. CrossRef - Retrospective database analysis of cancer risk in patients with type 2 diabetes mellitus in China
Xiaoning He, Lizheng Shi, Jing Wu
Current Medical Research and Opinion.2018; 34(6): 1089. CrossRef - Association of genetic variants in ATR-CHEK1 and ATM-CHEK2 pathway genes with risk of colorectal cancer in a Chinese population
Shijia Wang, Yue Zhang, Min Chen, Yong Wang, Yifei Feng, Ziwei Xu, Dongsheng Zhang, Yueming Sun, Zan Fu
Oncotarget.2018; 9(42): 26616. CrossRef - Metformin inhibits human breast cancer cell growth by promoting apoptosis via a ROS-independent pathway involving mitochondrial dysfunction: pivotal role of superoxide dismutase (SOD)
Prateek Sharma, Sanjeev Kumar
Cellular Oncology.2018; 41(6): 637. CrossRef - 3. Comprehensive Medical Evaluation and Assessment of Comorbidities:Standards of Medical Care in Diabetes—2018
Diabetes Care.2018; 41(Supplement): S28. CrossRef - 2017 update on the relationship between diabetes and colorectal cancer: epidemiology, potential molecular mechanisms and therapeutic implications
Nieves González, Isabel Prieto, Laura del Puerto-Nevado, Sergio Portal-Nuñez, Juan Antonio Ardura, Marta Corton, Beatriz Fernández-Fernández, Oscar Aguilera, Carmen Gomez-Guerrero, Sebastián Mas, Juan Antonio Moreno, Marta Ruiz-Ortega, Ana Belen Sanz, Mar
Oncotarget.2017; 8(11): 18456. CrossRef - Systems and precision medicine approaches to diabetes heterogeneity: a Big Data perspective
Enrico Capobianco
Clinical and Translational Medicine.2017;[Epub] CrossRef - Hyperglycemia exacerbates colon cancer malignancy through hexosamine biosynthetic pathway
A Vasconcelos-dos-Santos, H F B R Loponte, N R Mantuano, I A Oliveira, I F de Paula, L K Teixeira, J C M de-Freitas-Junior, K C Gondim, N Heise, R Mohana-Borges, J A Morgado-Díaz, W B Dias, A R Todeschini
Oncogenesis.2017; 6(3): e306. CrossRef - A Comprehensive Survey of the Roles of Highly Disordered Proteins in Type 2 Diabetes
Zhihua Du, Vladimir Uversky
International Journal of Molecular Sciences.2017; 18(10): 2010. CrossRef - Colon cancer modulation by a diabetic environment: A single institutional experience
Isabel Prieto, Laura del Puerto-Nevado, Nieves Gonzalez, Sergio Portal-Nuñez, Sandra Zazo, Marta Corton, Pablo Minguez, Carmen Gomez-Guerrero, Jose Miguel Arce, Ana Belen Sanz, Sebastian Mas, Oscar Aguilera, Gloria Alvarez-Llamas, Pedro Esbrit, Alberto Or
PLOS ONE.2017; 12(3): e0172300. CrossRef - Prevalence of elevated liver enzymes in adults with type 1 diabetes: A multicentre analysis of the German/Austrian DPV database
Marietta Stadler, Esther Bollow, Maria Fritsch, Wolfgang Kerner, Ingrid Schuetz‐Fuhrmann, Dietmar Krakow, Sigrun Merger, Michaela Riedl, Peter Jehle, Reinhard W. Holl
Diabetes, Obesity and Metabolism.2017; 19(8): 1171. CrossRef - Review of 2017 Diabetes Standards of Care
Kate Crawford
Nursing Clinics of North America.2017; 52(4): 621. CrossRef - Glycans as Regulatory Elements of the Insulin/IGF System: Impact in Cancer Progression
Julio de-Freitas-Junior, Jéssica Andrade-da-Costa, Mariana Silva, Salomé Pinho
International Journal of Molecular Sciences.2017; 18(9): 1921. CrossRef - 3. Comprehensive Medical Evaluation and Assessment of Comorbidities
Diabetes Care.2017; 40(Supplement): S25. CrossRef - Cation-selective transporters are critical to the AMPK-mediated antiproliferative effects of metformin in human breast cancer cells
Hao Cai, Yunhui Zhang, Tianxiang Kevin Han, Ruth S. Everett, Dhiren R. Thakker
International Journal of Cancer.2016; 138(9): 2281. CrossRef - Looking at the carcinogenicity of human insulin analogues via the intrinsic disorder prism
Elrashdy M. Redwan, Moustafa H. Linjawi, Vladimir N. Uversky
Scientific Reports.2016;[Epub] CrossRef - Two variants on T2DM susceptible gene HHEX are associated with CRC risk in a Chinese population
Rui Sun, Jian-Ping Liu, Chang Gao, Ying-Ying Xiong, Min Li, Ya-Ping Wang, Yan-Wei Su, Mei Lin, An-Li Jiang, Ling-Fan Xiong, Yan Xie, Jue-Ping Feng
Oncotarget.2016; 7(20): 29770. CrossRef - 3. Foundations of Care and Comprehensive Medical Evaluation
Diabetes Care.2016; 39(Supplement): S23. CrossRef - Mortality and causes of death in a national sample of type 2 diabetic patients in Korea from 2002 to 2013
Yu Mi Kang, Ye-Jee Kim, Joong-Yeol Park, Woo Je Lee, Chang Hee Jung
Cardiovascular Diabetology.2016;[Epub] CrossRef - Association Between Chronic Conditions and Physical Function Among Veteran and Non-Veteran Women With Diabetes
Kristen E. Gray, Jodie G. Katon, Eileen Rillamas-Sun, Lori A. Bastian, Karin M. Nelson, Andrea Z. LaCroix, Gayle E. Reiber
The Gerontologist.2016; 56(Suppl 1): S112. CrossRef - 3. Initial Evaluation and Diabetes Management Planning
Diabetes Care.2015; 38(Supplement): S17. CrossRef - Lack of metformin effect on mouse embryo AMPK activity: implications for metformin treatment during pregnancy
Hyung‐yul Lee, Dan Wei, Mary R. Loeken
Diabetes/Metabolism Research and Reviews.2014; 30(1): 23. CrossRef - Standards of Medical Care in Diabetes—2014
Diabetes Care.2014; 37(Supplement): S14. CrossRef - Detection bias may be the main cause of increased cancer incidence among diabetics: Results from the Rotterdam Study
Kirstin M.J. De Bruijn, Rikje Ruiter, Catherine E. de Keyser, Albert Hofman, Bruno H. Stricker, Casper H.J. van Eijck
European Journal of Cancer.2014; 50(14): 2449. CrossRef - Effects of Metformin Dose on Cancer Risk Reduction in Patients with Type 2 Diabetes Mellitus: A 6-Year Follow-up Study
Hsiu-Chen Lin, Baxter H. Kachingwe, Hsiu-Li Lin, Hui Wen Cheng, Yow-Shieng Uang, Li-Hsuan Wang
Pharmacotherapy: The Journal of Human Pharmacology and Drug Therapy.2014; 34(1): 36. CrossRef - Hyperglycemia as a Risk Factor for Cancer Progression
Tae Young Ryu, Jiyoung Park, Philipp E. Scherer
Diabetes & Metabolism Journal.2014; 38(5): 330. CrossRef - High glucose and insulin differentially modulates proliferation in MCF-7 and MDA-MB-231 cells
Chanchal Gupta, Kulbhushan Tikoo
Journal of Molecular Endocrinology.2013; 51(1): 119. CrossRef - Systematic review and meta-analysis of the association between diabetes mellitus and incidence and mortality in breast and colorectal cancer
K M J De Bruijn, L R Arends, B E Hansen, S Leeflang, R Ruiter, C H J van Eijck
British Journal of Surgery.2013; 100(11): 1421. CrossRef - Obesity, diabetes mellitus, and the risk of female breast cancer in Eastern China
Xiao-Lei Wang, Cun-Xian Jia, Li-Yuan Liu, Qiang Zhang, Yu-Yang Li, Liang Li
World Journal of Surgical Oncology.2013;[Epub] CrossRef - Effect of Type 2 Diabetes Mellitus on Prognosis of Nonmetastatic Renal Cell Cancer
Evren Süer, Erdem Öztürk, Ömer Gülpınar, Aytaç Kayış, Sümer Baltacı
Korean Journal of Urology.2013; 54(8): 499. CrossRef - Glycemic index, glycemic load and cancer risk
J. Hu, C. La Vecchia, L.S. Augustin, E. Negri, M. de Groh, H. Morrison, L. Mery
Annals of Oncology.2013; 24(1): 245. CrossRef - The Relationship between Type 2 Diabetes and Cancer: An Integrative Review
Mutaz Arafat Altamimi
SSRN Electronic Journal.2013;[Epub] CrossRef - Diabetes Mellitus and the Risk for Developing Cancer
Shane Malachy Markey, Marie A Congiusta
International Journal of Experimental Dental Science.2013; 2(1): 41. CrossRef - Standards of Medical Care in Diabetes—2013
Diabetes Care.2013; 36(Supplement): S11. CrossRef - Targeted therapy in rare cancers—adopting the orphans
Javier Munoz, Razelle Kurzrock
Nature Reviews Clinical Oncology.2012; 9(11): 631. CrossRef - Obesity and Pancreatic Diseases
Ho Gak Kim, Jimin Han
The Korean Journal of Gastroenterology.2012; 59(1): 35. CrossRef - CYP2W1, CYP4F11 and CYP8A1 Polymorphisms and Interaction of CYP2W1 Genotypes with Risk Factors in Mexican Women with Breast Cancer
N. Cardenas-Rodriguez, E. Lara-Padilla, C. Bandala, J. Lopez-Cruz, C. Uscanga-Carmona, P.F. Lucio-Monter, E. Floriano-Sanchez
Asian Pacific Journal of Cancer Prevention.2012; 13(3): 837. CrossRef - Standards of Medical Care in Diabetes—2012
Diabetes Care.2012; 35(Supplement): S11. CrossRef - The Risk of Bladder Cancer in Korean Diabetic Subjects Treated with Pioglitazone
Sun Ok Song, Kwang Joon Kim, Byung-Wan Lee, Eun Seok Kang, Bong Soo Cha, Hyun Chul Lee
Diabetes & Metabolism Journal.2012; 36(5): 371. CrossRef - L’uso prolungato di metformina è associato con la riduzione del rischio di carcinoma mammario
M. Bodmer, C. Meier, S. Krähenbühl, S. S. Jick, C. R. Meier, Francesca Marciello, Antongiulio Faggiano, Annamaria Colao
L'Endocrinologo.2011; 12(6): 310. CrossRef

 KDA
KDA PubReader
PubReader Cite
Cite



