- Current
- Browse
- Collections
-
For contributors
- For Authors
- Instructions to authors
- Article processing charge
- e-submission
- For Reviewers
- Instructions for reviewers
- How to become a reviewer
- Best reviewers
- For Readers
- Readership
- Subscription
- Permission guidelines
- About
- Editorial policy
Articles
- Page Path
- HOME > Diabetes Metab J > Volume 35(2); 2011 > Article
-
Original ArticleChanges in Adenosine Deaminase Activity in Patients with Type 2 Diabetes Mellitus and Effect of DPP-4 Inhibitor Treatment on ADA Activity
- Jae-Geun Lee1, Dong Gu Kang1, Jung Re Yu1, Youngree Kim2, Jinsoek Kim1, Gwanpyo Koh1, Daeho Lee1
-
Diabetes & Metabolism Journal 2011;35(2):149-158.
DOI: https://doi.org/10.4093/dmj.2011.35.2.149
Published online: April 30, 2011
1Department of Internal Medicine, Jeju National University Hospital, Jeju National University School of Medicine, Jeju, Korea.
2Department of Laboratory Medicine, Jeju National University Hospital, Jeju National University School of Medicine, Jeju, Korea.
- Corresponding author: Daeho Lee. Department of Internal Medicine, Jeju National University School of Medicine, 66 Jejudaehak-ro, Jeju 690-756, Korea. Ldhkso@jejunu.ac.kr
Copyright © 2011 Korean Diabetes Association
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/3.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
ABSTRACT
-
Background
- Dipeptidyl peptidase 4 (DPP-4, also known as CD26) binds with adenosine deaminase (ADA) to activate T lymphocytes. Here, we investigated whether ADA activity is specifically affected by treatment with DPP-4 inhibitor (DPP4I) compared with other anti-diabetic agents.
-
Methods
- Fasting ADA activity, in addition to various metabolic and biochemical parameters, were measured in 262 type 2 diabetes mellitus (T2DM) patients taking various anti-diabetic agents and in 46 non-diabetic control subjects.
-
Results
- ADA activity was increased in T2DM patients compared with that in non-diabetic control subjects (mean±standard error, 23.1±0.6 U/L vs. 18.6±0.8 U/L; P<0.05). ADA activity was correlated with fasting plasma glucose (r=0.258, P<0.05), HbA1c (r=0.208, P<0.05), aspartate aminotransferase (r=0.325, P<0.05), and alanine aminotransferase (r=0.248, P<0.05). Compared with the well-controlled T2DM patients (HbA1c<7%), the poorly controlled group (HbA1c>9%) showed significantly increased ADA activity (21.1±0.8 U/L vs. 25.4±1.6 U/L; P<0.05). The effect of DPP4I on ADA activity in T2DM patients did not differ from those of other oral anti-diabetic agents or insulin. T2DM patients on metformin monotherapy showed a lower ADA activity (20.9±1.0 U/L vs. 28.1±2.8 U/L; P<0.05) compared with that of those on sulfonylurea monotherapy.
-
Conclusion
- Our results show that ADA activity is increased in T2DM patients compared to that in non-diabetic patients, is positively correlated with blood glucose level, and that DPP4I has no additional specific effect on ADA activity, except for a glycemic control- or HbA1c-dependent effect.
- Glucagon-like peptide-1 (GLP-1) [1,2], an incretin, promotes insulin secretion in a glucose concentration-dependent manner in pancreatic beta cells [3], inhibits glucagon secretion in alpha cells [4], decreases the gastric discharge rate [5], and mediates appetite suppression [6]. However, because GLP-1 is rapidly degraded by dipeptidyl peptidase-4 (DPP-4), oral DPP-4 inhibitor (DPP4I) drugs and GLP-1 analogues have been developed to overcome the GLP-1 degradation effect in the treatment of diabetes [7].
- DPP-4, also known as CD26 or adenosine deaminase (ADA) binding protein, is a cellular membrane ectopeptidase in the prolyl oligopeptidase family [8,9]. Mammalian endothelial and epithelial cells generally express DPP-4; it is particularly abundantly expressed in the intestines, bone marrow, kidney, and liver. The enzymatic function of this molecule is not limited to direct action upon various substrates; it is also involved in the regulation of cellular functions through interactions with various extracellular substrates [8,10]. DPP-4 is also expressed in the cells of the immune system, especially in T cells, in which it interacts with other signal transduction pathways (CD3) and acts as a co-stimulator of T cell (particularly CD4+ T cell); the promotion of T-cell responses to foreign antigens, initial signal transduction, increased cytokine secretion, promotion of cell proliferation, increased expression of active T-cell markers (CD25, CD71, and CD69), promotion of effector cell differentiation, increased cellular mobility, and many other actions [8-10]. After new anti-diabetic drugs that selectively inhibit DPP-4 were introduced and administered to diabetic patients, there were several reports that DPP4I might increase the incidences of some infectious diseases (e.g., nasopharyngitis and urinary tract infection), so further experimental and clinical studies are needed to determine the effects of DPP-4 on immune cell function [11-13]. One alleged side effect of DPP-4 inhibition is the nonspecific inhibition of DPP-8 and DPP-9. However, according to a recent study, high doses of vildagliptin, producing nearly complete inhibition of DPP-8 and DPP-9 in vivo, yielded no toxicities in rodents [14]. Therefore, further studies are required regarding the side effects of DPP4Is.
- DPP-4 can also bind with ADA. Since ADA degrades adenosine, which inhibits the proliferation of T cells, this interaction of DPP-4 with ADA and the rearrangement of ADA on cell membrane can lead to the increase in T-cell proliferation and cytokine synthesis due to ADA activity on the cell membrane [15-17].
- ADA is an enzyme that converts adenosine into inosine through an irreversible deamination reaction [18]. Previous studies have reported that the highest ADA activity was ob-served in the lymphoid and fatty tissues, liver, skeletal muscle, and heart, although the activity was widely distributed in most organs [19,20]. An increase in ADA activity in type 2 diabetic (T2DM) patients has been reported [21-23]. While the mechanism that increases serum and tissue ADA activity is not well known, with higher ADA activity in insulin-sensitive tissues, the level of adenosine, which increases glucose uptake into cells, will be reduced [24]. Thus, if ADA activity is suppressed, insulin sensitivity may be improved, and cellular proliferation, inflammation, and T-cell activity, all of which are associated with the pathophysiology of insulin resistance, can also be affected. Therefore, insulin resistance may have an important relationship with ADA activity. However, it is difficult to conclude whether changes in ADA activity are the cause or result of ac-tual insulin resistance [25,26]. In addition to its association with diabetes, serum ADA activity is also increased in patients with liver cirrhosis as well as in patient with infectious diseases such as hepatitis, tuberculosis, brucellosis, and typhoid fever [27,28].
- Studies of the many functions of DPP-4, particularly those related to T-cell function, were performed prior to the development of the DPP-4 selective inhibitor. As such, some of those studies used non-selective DPP inhibitors with low specificity and could have non-specific study results due to inhibition of other isoforms of DPPs in addition to DPP-4 [14,29].
- Since ADA activity is associated with T-cell activity and insulin resistance and can bind with DPP-4, in the present study, we measured serum ADA activity in T2DM patients to evaluate the relationship between serum ADA activity and various clinical and metabolic parameters including inflammatory markers and to check if selective DPP4I affect ADA activity in T2DM patients.
INTRODUCTION
- Subjects
- The measurement of ADA activity was performed in patients with type 2 diabetes (T2DM, n=262) who were outpatients or who were hospitalized to control their blood glucose levels. All of the patients were on their oral anti-diabetic medications or insulin injection for more than one month. Standard biochemical, metabolic, and anthropometric measurements were also performed in the subjects. Non-diabetic healthy subjects who visited our hospital for health screenings or standard medical examinations were selected as the control group (Non-DM, n=46). Patients with type 1 diabetes, systemic infectious diseases, systemic inflammatory diseases, viral or alcoholic liver disease, advanced cardiovascular disease or other acute diseases, pregnant women, and patients with a glomerular filtration rate less than 60 mL/min/1.73 m2 were excluded from this study.
- After receiving a summary of the purpose of this study, the participants provided consent, and this study was conducted after approval from the Jeju National University Hospital Institutional Review Board (IRB No. #2009-11).
- Methods
- Blood and urine tests were performed after at least eight hours of fasting, and microalbumin tests were calibrated to be measured with urinary creatinine concentration (urine albumin to creatinine ratio [UACR], mg/g of creatinine). For blood cell calculation tests, total lymphocytes were calculated using complete blood cell count. High sensitivity C-reactive protein (hsCRP) and erythrocyte sedimentation rates (ESR) were measured as inflammation markers. Serum ADA activity was measured using UV spectrophotometry (Asan Pharmaceutical Co., Seoul, Korea). C-peptides were measured using a radioimmunoassay. Glycated hemoglobin (hemoglobin A1c, HbA1c) was measured using ion exchange HPLC (Tosoh Co., Tokyo, Japan).
- All technical data were expressed as means±standard errors, and statistical analysis was performed using the SPSS statistical program version 15.0 for Windows (SPSS Inc., Chicago, IL, USA). Clinical features in the control group and in T2DM patients were analyzed using independent sample t-tests, and Pearson's bivariate correlation analysis was used to correlate each variable with ADA activity. We performed multivariate regression analysis using log-substituted ADA activity as the dependent variable. Additionally, T2DM patients were classi-fied into smaller groups based on their glycemic control level, diabetes treatment medications, and liver function, and the differences in ADA activity among these smaller groups were also analyzed. Fasting plasma glucose (FPG) and HbA1c data was used to classify patients into three groups. The difference in ADA activities among the three groups was analyzed by using a one-way ANOVA test. The comparison of ADA activities according to diabetes treatment medication was performed using a one-way ANOVA test. The diabetic patients were divided into three groups as follows: the DPP4I group who were taking DPP4I and metformin combination therapy, the other oral hypoglycemic agent group who were taking metformin and other oral anti-diabetic agent(s) except for DPP4I, and the insulin treatment group (insulin combination therapy or insulin monotherapy groups). To clearly evaluate the efficacy of the DPP4Is, the differences in ADA activity and levels of inflammatory markers between the metformin only group and the metformin and DPP4I combination therapy group (DPP4I merged group) were also analyzed using independent sample t-tests. Additionally, in T2DM patients who were taking DPP4I, ADA activity and inflammatory markers were measured prior to administration of DPP4I and 8 to 12 weeks after and were compared using a paired t-test. The comparison of ADA activities according to statin therapy was also performed and independent sample t-tests were used to compare the groups; any statin therapy group vs. no statin therapy group.
- When analyzing the effects of drug treatment, ADA activity may be affected secondary to the degree of glycemic control. Therefore, when needed, ADA activity was adjusted using HbA1c value and the ANOVA test was performed.
- In patients with T2DM, even mild changes in liver function are considered to have any effect on ADA activity. Prati et al. [30] proposed upper normal limit values in men and women according to alanine aminotransferase (ALT) value. Here, among the T2DM patients, women with ALT values less than 19 IU/L and men with ALT values less than 30 IU/L were placed in the normal liver function group (Normal ALT), those who were not in that group were classified into the dysfunctional liver group (High ALT). The differences in ADA activity between two groups were analyzed using independent sample t-tests. P values less than 0.05 were considered statistically significant.
METHODS
Examinations
Statistical analysis
- Clinical characteristics of study subjects
- The clinical characteristics of the study subjects are shown in Table 1. The FPG values of the T2DM group (n=262) and the control group (n=46) were 154.8±3.4 mg/dL and 104.5±2.6 mg/dL (P<0.05), and the HbA1c of the T2DM group was significantly higher than that of the control group (7.7±0.1% vs. 6.2±0.1%, P<0.05). However, because some patients with impaired fasting glucose were included in the control group, FPG and HbA1c levels were slightly increased when compared to the values that would be expected for a group with completely normal glucose metabolism.
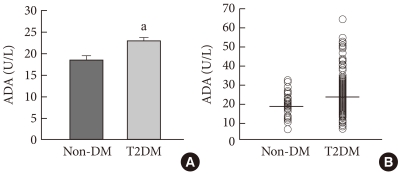
- Compared to the control group, ADA activity in T2DM patients was significantly higher (23.1±0.6 U/L vs. 18.6±0.8 U/L, P<0.05); the ADA activity range in the control group was 5.4 to 30.8 U/L compared to an ADA activity range of 5.8 to 64.6 U/L in the T2DM group. The ADA activity distributions in normal healthy subjects and T2DM patients showed considerable overlap (Table 1, Fig. 1).
- ADA activity and the correlations among various variables
- Regarding the correlations between ADA activity and other variables in all included experimental subjects, age, FPG, HbA1c, aspartate aminotransferase (AST), ALT, ESR, and serum creatinine levels of both the control group and the T2DM patient group were highly correlated with ADA activity (Table 2). In a multivariate regression analysis that included age, FPG, HbA1c, AST, ALT, ESR, and serum creatinine as input variables and log-substituted ADA activity as a dependent variable, age (β=0.164, P=0.028), FPG (β=0.259, P=0.004), HbA1c (β=0.168, P=0.012), and AST (β=0.264, P=0.014) remained significant.
- Degree of glycemic control in patients with T2DM according to the ADA activity comparison
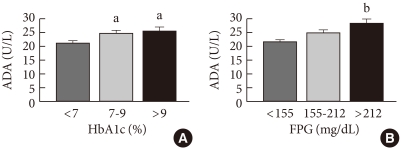
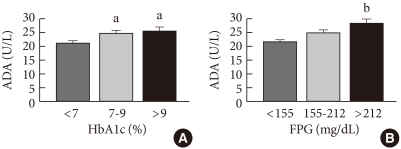
- Patients with T2DM were classified into three groups, those with HbA1c levels less than 7% (n=108), those with levels ranging from 7 to 9% (n=100), and those with levels greater than 9% (n=52). When the ADA activity levels of these groups were compared, the group with HbA1c level less than 7% had a significantly lower ADA activity compared to that of the groups with HbA1C levels between 7-9% and greater than 9% (21.1±0.8 U/L, 24.5±1.0 U/L, and 25.4±1.6 U/L for the less than 7%, 7-9%, and greater than 9% groups, respectively; P<0.05). However, the ADA activities in the 7-9% and greater than 9% HbA1c groups were not significantly different (P=0.849, Fig. 2A).
- T2DM patients were classified into three groups according to FPG level: less than 155 mg/dL (n=157), 155-212 mg/dL (n=66), and greater than 212 mg/dL (n=37). These groups were then analyzed for their ADA activity. The respective ADA activities were 21.5±0.7 U/L, 24.6±1.2 U/L, and 28.2±1.8 U/L. The group with FPG less than 155 mg/dL and that with FPG greater than 212 mg/dL had significant differences between their ADA activity levels. There were no significant differences between the less than 155 mg/dL FPG group and the 155-212 mg/dL FPG group (P=0.075) or between the 155-212 mg/dL FPG group and the greater than 212 mg/dL FPG group (P=0.171, Fig. 2B).
- Comparative ADA activity levels between the DPP4I treatment group and other treatment groups of T2DM patients
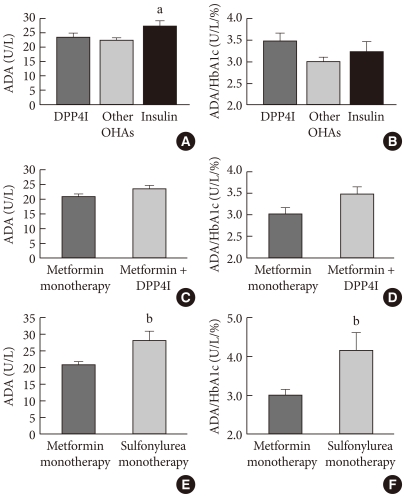
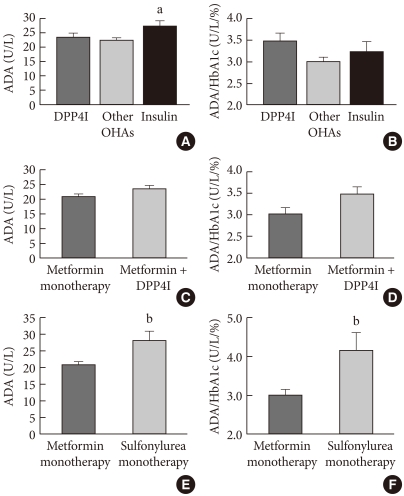
- T2DM patients were classified into three separate groups according to treatment type. Thirty-four patients were placed in the DPP4I treatment group, 195 patients were in the other oral anti-diabetic agent group, and 33 patients were in the insulin combination therapy group. The ADA activity values for the three groups were 23.6±1.3 U/L, 22.5±0.7 U/L, and 27.3±1.8 U/L, respectively. There was a significant difference between the other oral hypoglycemic agent group and the insulin combination therapy group (P<0.05). There were no significant differences in ADA activity level between the DPP4I treatment group and the other oral hypoglycemic agent group (P=0.834) or between the DPP4I treatment group and the insulin combination therapy group (P=0.278, Fig. 3A). When HbA1c level of these groups were compared, the insulin combination therapy group had a significantly higher HbA1c level compared to those of two other groups (6.8±0.1%, 7.6±0.1%, and 8.9±0.3% for DPP4I treatment group, the other oral hypoglycemic agent group, and the insulin combination therapy group, respectively; P<0.05). However, there was no significant difference in the ADA activity values that were adjusted for HbA1c among the three groups (Fig. 3B).
- The ADA activity results between the metformin monotherapy group (n=51) and the DPP4I combination therapy group (n=34) did not differ significantly (20.9±1.0 U/L vs. 23.6±1.3 U/L, P=0.09, Fig. 3C). In addition, there was no sig-nificant difference in HbA1c level between the two groups (7.1±0.2% vs. 6.8±0.1%, P=0.285), and there was very little difference in the ADA activity values that were adjusted for HbA1c (Fig. 3D).
- In order to better understand the effects of metformin monotreatment on ADA activity, we made independent comparisons of the metformin monotreatment group (n=50) and the sulfonylurea monotreatment group (n=9). These results showed that, despite the small difference in HbA1c value between them (7.1±0.2% vs. 6.9±0.4%, P=0.624), the ADA activity in the metformin monotreatment group was significantly lower than that of the sulfonylurea monotreatment group (20.9±1.0 U/L vs. 28.1±2.8 U/L, P<0.05, Fig. 3E). This suggests the possibility that metformin can directly influence ADA activity. Additionally, the ADA activity levels adjusted for HbA1c maintained a significant statistical difference (Fig. 3F).
- ADA activity comparison before and after DPP4I treatment in T2DM patients
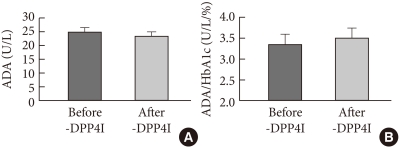
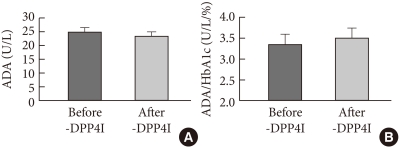
- We measured HbA1c and ADA activity levels before DPP4I treatment and 8 to 12 weeks after treatment in a small subgroup of the DPP4I treatment group (n=24). Despite the reductions in the comparatively analyzed results of HbA1c (7.4±0.2% vs. 6.6±0.1%, P<0.05), ADA activity (24.7±1.7 U/L vs. 23.0±1.6 U/L, P=0.154) showed no change (Fig. 4A). Additionally, ADA activity levels before and after DPP4I adminis-tration were adjusted for HbA1c, but the comparatively analyzed results did not show a significant difference (3.4±0.2 U/L/% vs. 3.5±0.2 U/L/%, P=0.347, Fig. 4B).
- These results suggest that ADA activity is unaffected by DPP4I administration regardless of glycemic control. Also, leukocytes, lymphocyte count, lymphocyte percentage, ESR, and hsCRP before and after the administration of DPP4I were not significantly statistically different.
- Comparison of ADA activity according to statin therapy in T2DM patients
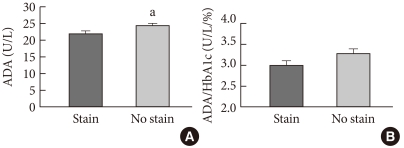
- T2DM patients were classified into two groups according to statin treatment or not. Between the statin-treated (n=114) and non-treated (n=146) groups, the comparatively analyzed results showed little difference with regard to HbA1c level (7.7±0.1% vs. 7.7±0.1%, P=0.851) or FPG level (154.0±5.7 mg/dL vs. 155.6±4.2 mg/dL, P=0.833). However, ADA activity was significantly lower in the statin-treated group than in the group not treated with statins (22.0±0.8 U/L vs. 24.2±0.9 U/L, P<0.05, Fig. 5A). Even after ADA activity was adjusted for HbA1c, there was a strong tendency toward a lower ADA activity in the statin-treated group compared to the non-treated group (P=0.086, Fig. 5B). Additionally, the comparable levels of AST, ALT, and hsCRP between the two groups suggest that ADA activity could be directly inhibited by statin.
- Comparison of ADA activity according to liver function in T2DM patients
- We applied the upper limit of the normal values of liver function tests in healthy male and female subjects proposed by Prati et al. [30] to patients with T2DM, divided them according to ALT value into normal ALT and high ALT groups, and their ADA activities were compared. In female patients, ADA activity in the normal ALT group (n=37) was significantly lower than that in the high ALT group (n=75) (21.8±1.2 U/L vs. 26.0±1.1 U/L, P<0.05). The same was true in male patients (20.9±1.0 U/L vs. 24.2±1.3 U/L, P<0.05). All T2DM patients were classified as normal ALT (n=125) or high ALT (n=128), and a comparison of ADA activity showed that the normal ALT group had significantly lower ADA activity than did the high ALT group (21.2±0.8 U/L vs. 25.9±0.8 U/L, P<0.05).
- T2DM patients with normal liver function were classified into the following groups according to FPG level: less than 155 mg/dL (n=74), 155-212 mg/dL (n=34), and greater than 212 mg/dL (n=17). The ADA activities of the groups were 19.7±1.0 U/L, 22.5±1.4 U/L, and 25.3±2.5 U/L, respectively, and there was a considerable difference in the ADA activity between the group with FPG less than 155 mg/dL and the group with FPG greater than 212 mg/dL.
- The comparisons of ADA activity and other factors in T2DM patients
- T2DM patients were separated into subgroups based on several variables, including hsCRP level (hsCRP<3 mg/L and ≥3 mg/L), white blood cell count (<10.0×103/µL group and ≥10.0×103/µL), and lymphocyte percentage (<44% and ≥44%), and comparisons of ADA activity were made for each pair of subgroups. ADA activity did not show a significant difference between the groups with high and low levels of each variable.
RESULTS
- Because DPP-4 is an ADA-binding partner and ADA is closely related to T lymphocyte function [9] and insulin resistance, in the present study, we measured ADA activity in T2DM patients to evaluate whether there is an effect from selective DPP4I treatment and whether ADA activity is affected by other therapeutic drugs. According to our results, ADA activity in T2DM patients was significantly higher than that in the control group, and had positive correlations with both FPG and HbA1c.
- T2DM patients were also classified according to drug treatment type, and the ADA activity analysis results showed that the DPP4I treatment group did not have a significant difference in ADA activity from that of the other oral agent group or from that of the insulin treatment group. Also, the comparison of ADA activity between the metformin monotherapy group and the DPP4I combination therapy group showed no significant difference. Even when ADA activity was compared before and after DPP4I treatment, and regardless of glycemic control status, DPP4I treatments were confirmed not to have any specific effect on ADA activity. Conversely, when HbA1c had a tendency to be lower, ADA activity remained proportional, which suggests that ADA activity can increase as a result of selective DPP4I treatment. At least, in the present study, it was confirmed that DPP4I did not reduce ADA activity. One of the possible reasons that ADA activity was not affected by selective DPP4Is is evident through a recent analysis of the DPP-4 protein structures which revealed the active sites of DPP-4, active binding site of DPP4Is, and ADA binding site. Since the actions of these small molecules with selective DPP-4 inhibitory actions are limited to the DPP-4 catalytic pocket, the selective DPP4Is are unlikely to affect conformational structure of the DPP-4 protein, its dimerization, ant its interactions with other binding partners [31]. However, recent cellular and animal experimental results have shown that the mobility of CD4+ T lymphocytes derived from the spleens of non-obese diabetic (NOD) mice is increased by soluble DPP-4 (sDPP-4) [32]. Also, sitagliptin suppressed sDPP-4-induced CD4+ T cell infiltration in the islets. So, the diabetes reduction by sitagliptin treatment in NOD mice seems to involve a re-duction in T-cell mobility, and then the reduction of insulitis [32]. Thus, although selective DPP4Is did not have an effect on ADA activity, more studies of the effects of DPP4Is on T-cell functions are needed.
- ADA activity comparisons of oral hypoglycemic monotreatment groups showed that ADA activity was significantly lower in the metformin monotreatment group than it was in the sulfonylurea monotreatment group. Metformin decreases insulin resistance, so ADA activity is expected to decrease in conjunction with metformin therapy. Reports from one study conducted on red blood cell lysates showed that metformin did not directly inhibit ADA activity [33]. The ADA activity in the statin-treated group was significantly lower when compared to the activity in the non-treated group; this difference was not related to glycemic control, but statin itself may potentially affect ADA activity. In previous studies, it was reported that simvastatin-treated groups have significantly reduced ADA activity [34]; however, the exact mechanism still remains unclear. Statin's lipid-lowering effects and various other effects such as an anti-inflammatory actions, T-cell differentiation inhibition, TNF-α inhibition, and other immune regulatory effects [35-37] may be considered to have an effect on ADA activity.
- In line with previous reports done by other researchers, ADA activity in T2DM patients in the present study was significantly higher than that in the control group [21-23]. Moreover, compared to that of T2DM patients with relatively good glycemic control, the ADA activity in T2DM patients with poor glycemic control was significantly lower. These results are consistent with those reported by Hoshino et al. [38].
- Although subjects with active liver diseases were excluded from this study, the patients with even mild liver dysfunction which seemed to be related to metabolic syndrome, had significantly higher ADA activity regardless of glycemic control. The differences in ADA activity corresponding to differences in the AST and ALT levels that reflect liver dysfunction are consistent with the reports from other studies [21,30]. A correlation between γ-GTP and ADA activity had also been reported [21], but was not shown to be statistically significant in the present study. When the ADA activity in diabetic patients with normal liver function was analyzed, the results showed that patients with poor glycemic control had significantly higher ADA activity. In the analysis of all patients and several subgroups, ADA activity did not have a significant correlation with hsCRP, white blood cell count, or lymphocyte count.
- The limitations of this study were as follows: 1) ADA activity differences based on glycemic control level, treatment medications and liver functions were compared in T2DM patients through a simple cross-sectional study, 2) comparisons before and after medical treatments were not performed, 3) because national health insurance does not cover DPP4I monotreatment, patients undergoing metformin baseline maintenance treatment who were treated with an additional DPP4I were classified into the DPP4I treatment group and analyzed as such. Additionally, the control group was composed of non-diabetic adults, and patients with diabetes were excluded in the group; however, adults with impaired fasting glucose may have been included in the control group.
- In conclusion, compared to the control group, ADA activity in T2DM patients was higher. When glycemic control was relatively good, ADA activity was low. However, although neither ADA activity nor inflammatory-response-related variables changed with DPP4I treatment regardless of changes in glycemic control.
- Thus, the results of this study suggest that the selective DPP4Is currently used by diabetic patients do not have any effect on the non-enzymatic action of DPP-4. In addition to this study focused on ADA activity, additional studies are needed to evaluate the effects of selective DPP4Is on other physiologic functions related to the non-enzymatic action of DPP-4.
DISCUSSION
-
Acknowledgements
- This work was supported by a research grant in 2009 from Jeju National University Hospital.
ACKNOWLEDGMENT
- 1. Drucker DJ. Enhancing incretin action for the treatment of type 2 diabetes. Diabetes Care 2003;26:2929-2940. ArticlePubMedPDF
- 2. Ahren B. Gut peptides and type 2 diabetes mellitus treatment. Curr Diab Rep 2003;3:365-372. ArticlePubMedPDF
- 3. Zander M, Madsbad S, Madsen JL, Holst JJ. Effect of 6-week course of glucagon-like peptide 1 on glycaemic control, insulin sensitivity, and beta-cell function in type 2 diabetes: a parallel-group study. Lancet 2002;359:824-830. PubMed
- 4. Drucker DJ. Biological actions and therapeutic potential of the glucagon-like peptides. Gastroenterology 2002;122:531-544. ArticlePubMed
- 5. Nauck MA, Niedereichholz U, Ettler R, Holst JJ, Orskov C, Ritzel R, Schmiegel WH. Glucagon-like peptide 1 inhibition of gastric emptying outweighs its insulinotropic effects in healthy humans. Am J Physiol 1997;273(5 Pt 1):E981-E988. ArticlePubMed
- 6. Turton MD, O'Shea D, Gunn I, Beak SA, Edwards CM, Meeran K, Choi SJ, Taylor GM, Heath MM, Lambert PD, Wilding JP, Smith DM, Ghatei MA, Herbert J, Bloom SR. A role for glucagon-like peptide-1 in the central regulation of feeding. Nature 1996;379:69-72. ArticlePubMedPDF
- 7. Deacon CF, Nauck MA, Toft-Nielsen M, Pridal L, Willms B, Holst JJ. Both subcutaneously and intravenously administered glucagon-like peptide I are rapidly degraded from the NH2-terminus in type II diabetic patients and in healthy subjects. Diabetes 1995;44:1126-1131. ArticlePubMed
- 8. Lambeir AM, Durinx C, Scharpe S, De Meester I. Dipeptidyl-peptidase IV from bench to bedside: an update on structural properties, functions, and clinical aspects of the enzyme DPP IV. Crit Rev Clin Lab Sci 2003;40:209-294. ArticlePubMed
- 9. Gorrell MD, Gysbers V, McCaughan GW. CD26: a multifunctional integral membrane and secreted protein of activated lymphocytes. Scand J Immunol 2001;54:249-264. ArticlePubMedPDF
- 10. De Meester I, Korom S, Van Damme J, Scharpe S. CD26, let it cut or cut it down. Immunol Today 1999;20:367-375. ArticlePubMed
- 11. Amori RE, Lau J, Pittas AG. Efficacy and safety of incretin therapy in type 2 diabetes: systematic review and meta-analysis. JAMA 2007;298:194-206. ArticlePubMed
- 12. Richter B, Bandeira-Echtler E, Bergerhoff K, Lerch CL. Dipeptidyl peptidase-4 (DPP-4) inhibitors for type 2 diabetes mellitus. Cochrane Database Syst Rev 2008;(2):CD006739ArticlePubMedPMC
- 13. Raz I, Hanefeld M, Xu L, Caria C, Williams-Herman D, Khatami H. Sitagliptin Study 023 Group. Efficacy and safety of the dipeptidyl peptidase-4 inhibitor sitagliptin as monotherapy in patients with type 2 diabetes mellitus. Diabetologia 2006;49:2564-2571. ArticlePubMedPDF
- 14. Kirby M, Yu DM, O'Connor S, Gorrell MD. Inhibitor selectivity in the clinical application of dipeptidyl peptidase-4 inhibition. Clin Sci (Lond) 2009;118:31-41. ArticlePubMedPDF
- 15. Martin DW Jr, Gelfand EW. Biochemistry of diseases of immunodevelopment. Annu Rev Biochem 1981;50:845-877. ArticlePubMed
- 16. Ocana I, Martinez-Vazquez JM, Segura RM, Fernandez-De-Sevilla T, Capdevila JA. Adenosine deaminase in pleural fluids. Test for diagnosis of tuberculous pleural effusion. Chest 1983;84:51-53. ArticlePubMed
- 17. Barnes PF, Mistry SD, Cooper CL, Pirmez C, Rea TH, Modlin RL. Compartmentalization of a CD4+ T lymphocyte subpopulation in tuberculous pleuritis. J Immunol 1989;142:1114-1119. ArticlePubMedPDF
- 18. Brady T. Adenosine deaminase. Biochem J 1942;36:478-484. ArticlePubMedPMCPDF
- 19. Ratech H, Hirschhorn R. Serum adenosine deaminase in normals and in a patient with adenosine deaminase deficient-severe combined immunodeficiency. Clin Chim Acta 1981;115:341-347. ArticlePubMed
- 20. Niedzwicki JG, Abernethy DR. Structure-activity relationship of ligands of human plasma adenosine deaminase2. Biochem Pharmacol 1991;41:1615-1624. ArticlePubMed
- 21. Prakash MS, Chennaiah S, Murthy YS, Anjaiah E, Rao SA, Suresh C. Altered adenosine deaminase activity in type 2 diabetes mellitus. JIACM 2006;7:114-117.
- 22. Mokhtari M, Hashemi M, Yaghmaei M, Molashahi F, Shikhzadeh A, Niazi A, Ghavami S. Serum adenosine deaminase activity in gestational diabetes mellitus and normal pregnancy. Arch Gynecol Obstet 2010;281:623-626. ArticlePubMedPDF
- 23. Kurtul N, Pence S, Akarsu E, Kocoglu H, Aksoy Y, Aksoy H. Adenosine deaminase activity in the serum of type 2 diabetic patients. Acta Medica (Hradec Kralove) 2004;47:33-35. ArticlePubMed
- 24. Kather H. Pathways of purine metabolism in human adipocytes. Further evidence against a role of adenosine as an endogenous regulator of human fat cell function. J Biol Chem 1990;265:96-102. ArticlePubMed
- 25. Koopmans SJ, Sips HC, Bosman J, Radder JK, Krans HM. Antilipolytic action of insulin in adipocytes from starved and diabetic rats during adenosine-controlled incubations. Endocrinology 1989;125:3044-3050. ArticlePubMed
- 26. Green A, Newsholme EA. Sensitivity of glucose uptake and lipolysis of white adipocytes of the rat to insulin and effects of some metabolites. Biochem J 1979;180:365-370. ArticlePubMedPMCPDF
- 27. Kobayashi F, Ikeda T, Marumo F, Sato C. Adenosine deaminase isoenzymes in liver disease. Am J Gastroenterol 1993;88:266-271. PubMed
- 28. Kalkan A, Bulut V, Erel O, Avci S, Bingol NK. Adenosine deaminase and guanosine deaminase activities in sera of patients with viral hepatitis. Mem Inst Oswaldo Cruz 1999;94:383-386. ArticlePubMed
- 29. Lankas GR, Leiting B, Roy RS, Eiermann GJ, Beconi MG, Biftu T, Chan CC, Edmondson S, Feeney WP, He H, Ippolito DE, Kim D, Lyons KA, Ok HO, Patel RA, Petrov AN, Pryor KA, Qian X, Reigle L, Woods A, Wu JK, Zaller D, Zhang X, Zhu L, Weber AE, Thornberry NA. Dipeptidyl peptidase IV inhibition for the treatment of type 2 diabetes: potential importance of selectivity over dipeptidyl peptidases 8 and 9. Diabetes 2005;54:2988-2994. PubMed
- 30. Prati D, Taioli E, Zanella A, Della Torre E, Butelli S, Del Vecchio E, Vianello L, Zanuso F, Mozzi F, Milani S, Conte D, Colombo M, Sirchia G. Updated definitions of healthy ranges for serum alanine aminotransferase levels. Ann Intern Med 2002;137:1-10. ArticlePubMed
- 31. Biftu T, Scapin G, Singh S, Feng D, Becker JW, Eiermann G, He H, Lyons K, Patel S, Petrov A, Sinha-Roy R, Zhang B, Wu J, Zhang X, Doss GA, Thornberry NA, Weber AE. Rational design of a novel, potent, and orally bioavailable cyclohexylamine DPP-4 inhibitor by application of molecular modeling and X-ray crystallography of sitagliptin. Bioorg Med Chem Lett 2007;17:3384-3387. ArticlePubMed
- 32. Kim SJ, Nian C, McIntosh CH. Sitagliptin (MK0431) inhibition of dipeptidyl peptidase IV decreases nonobese diabetic mouse CD4+ T-cell migration through incretin-dependent and -independent pathways. Diabetes 2010;59:1739-1750. ArticlePubMedPMCPDF
- 33. Paiva M, Riksen NP, Davidson SM, Hausenloy DJ, Monteiro P, Goncalves L, Providencia L, Rongen GA, Smits P, Mocanu MM, Yellon DM. Metformin prevents myocardial reperfusion injury by activating the adenosine receptor. J Cardiovasc Pharmacol 2009;53:373-378. ArticlePubMed
- 34. Kowalczyk E, Kopff M, Kowalski J, Kopff A, Mikhailidis DP, Barylski M, Banach M. Effect of cardiovascular drugs on adenosine deaminase activity. Angiology 2008-2009;59:740-744. ArticlePDF
- 35. Albert MA, Danielson E, Rifai N, Ridker PM. PRINCE Investigators. Effect of statin therapy on C-reactive protein levels: the pravastatin inflammation/CRP evaluation (PRINCE): a randomized trial and cohort study. JAMA 2001;286:64-70. ArticlePubMed
- 36. Palinski W. Immunomodulation: a new role for statins? Nat Med 2000;6:1311-1312. ArticlePubMedPDF
- 37. Kwak B, Mulhaupt F, Myit S, Mach F. Statins as a newly recognized type of immunomodulator. Nat Med 2000;6:1399-1402. ArticlePubMedPDF
- 38. Hoshino T, Yamada K, Masuoka K, Tsuboi I, Itoh K, Nonaka K, Oizumi K. Elevated adenosine deaminase activity in the serum of patients with diabetes mellitus. Diabetes Res Clin Pract 1994;25:97-102. ArticlePubMed
REFERENCES

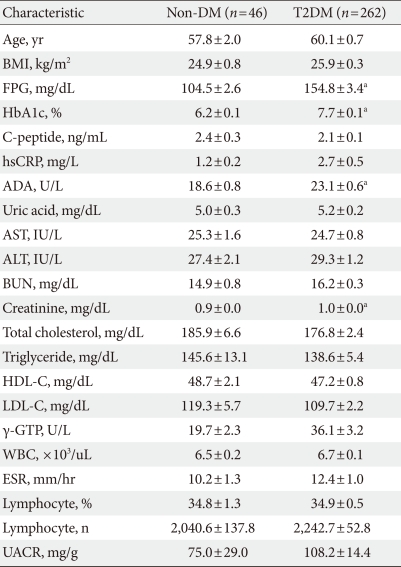
Data are presented as means±standard error.
T2DM, type 2 diabetes mellitus; BMI, body mass index; FPG, fasting plasma glucose; ADA, adenosine deaminase; hsCRP, high sensitivity C-reactive protein; HDL-C, high density lipoprotein cholesterol; LDL-C, low density lipoprotein cholesterol; γ-GTP, gamma GTP; WBC, white blood cell; ESR, erythrocyte sedimentation rate; UACR, urine albumin to creatinine ratio.
aP<0.05 vs. Non-DM group.
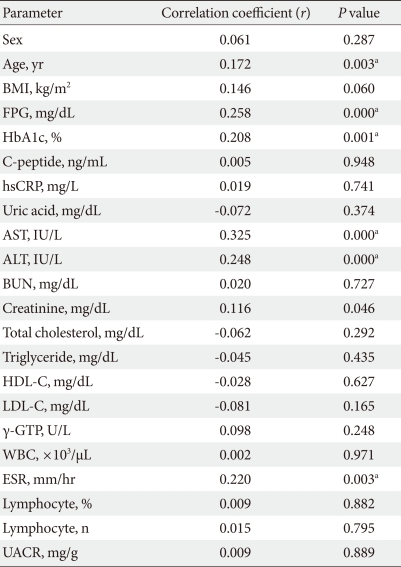
ADA, adenosine deaminase; BMI, body mass index; FPG, fasting plasma glucose; hsCRP, high sensitivity C-reactive protein; HDL-C, high density lipoprotein cholesterol; LDL-C, low density lipoprotein cholesterol; γ-GTP, gamma GTP; WBC, white blood cell; ESR, erythrocyte sedimentation rate; UACR, urine albumin to creatinine ratio.
aP<0.05.
Figure & Data
References
Citations

- Influence of BMI on adenosine deaminase and stroke outcomes in mechanical thrombectomy subjects
Benton Maglinger, Christopher J. McLouth, Jacqueline A. Frank, Chintan Rupareliya, Madison Sands, Lila Sheikhi, Shivani Pahwa, David Dornbos, Jordan P. Harp, Amanda L. Trout, Jadwiga Turchan-Cholewo, Ann M. Stowe, Justin F. Fraser, Keith R. Pennypacker
Brain, Behavior, & Immunity - Health.2022; 20: 100422. CrossRef - Glutamine restores testicular glutathione-dependent antioxidant defense and upregulates NO/cGMP signaling in sleep deprivation-induced reproductive dysfunction in rats
M.A. Hamed, T.M. Akhigbe, R.E. Akhigbe, A.O. Aremu, P.A. Oyedokun, J.A. Gbadamosi, P.E. Anifowose, M.A. Adewole, O.O. Aboyeji, H.O. Yisau, G.O. Tajudeen, M.M. Titiloye, N.F. Ayinla, A.F. Ajayi
Biomedicine & Pharmacotherapy.2022; 148: 112765. CrossRef - Effects of quercetin and metabolites on uric acid biosynthesis and consequences for gene expression in the endothelium
Sarka Tumova, Yuanlu Shi, Ian M. Carr, Gary Williamson
Free Radical Biology and Medicine.2021; 162: 191. CrossRef - The value of adenosine deaminase activity in latent autoimmune diabetes in adults and type 2 diabetes patients
Yu Zhou, Wei-Dong Jin, Zhen-Zhen Pang, Jun Xia, Su-Feng Chen
International Journal of Diabetes in Developing Countries.2021; 41(1): 48. CrossRef - Purinergic signaling in diabetes and metabolism
Shanu Jain, Kenneth A. Jacobson
Biochemical Pharmacology.2021; 187: 114393. CrossRef - Berberine modulates crucial erectogenic biomolecules and alters histological architecture in penile tissues of diabetic rats
Stephen Adeniyi Adefegha, Ganiyu Oboh, Felix Abayomi Dada, Sunday Idowu Oyeleye, Bathlomew Maduka Okeke
Andrologia.2021;[Epub] CrossRef - Suppression of uric acid and lactate production by sodium acetate ameliorates hepatic triglyceride accumulation in fructose-insulin resistant pregnant rats
Adewumi O. Oyabambi, Kehinde S. Olaniyi, Ayodele O. Soladoye, Lawrence A. Olatunji
Environmental Toxicology and Pharmacology.2020; 80: 103452. CrossRef - Therapeutic Perspectives of Adenosine Deaminase Inhibition in Cardiovascular Diseases
Barbara Kutryb-Zajac, Paulina Mierzejewska, Ewa M. Slominska, Ryszard T. Smolenski
Molecules.2020; 25(20): 4652. CrossRef - Adenosine as a Marker and Mediator of Cardiovascular Homeostasis: A Translational Perspective
Trevor Simard, Richard Jung, Alisha Labinaz, Mohammad Ali Faraz, F. Daniel Ramirez, Pietro Di Santo, Ian Pitcher, Pouya Motazedian, Chantal Gaudet, Rebecca Rochman, Jeffrey Marbach, Paul Boland, Kiran Sarathy, Saleh Alghofaili, Juan J. Russo, Etienne Cout
Cardiovascular & Hematological Disorders-Drug Targets.2019; 19(2): 109. CrossRef - Mineralocorticoid receptor blockade attenuates disrupted glutathione-dependent antioxidant defense and elevated endoglin in the hearts of pregnant rats exposed to testosterone
Taofeek O. Usman, Olufunto O. Badmus, InKyeom Kim, Lawrence A. Olatunji
Naunyn-Schmiedeberg's Archives of Pharmacology.2019; 392(7): 773. CrossRef - Serum activities of dipeptidyl peptidase-4 and adenosine deaminase in polycystic ovary syndrome: association with obesity
Seda Kahraman, Alev Eroglu Altinova, Serenay Elgun, Mehmet Muhittin Yalcin, Banu Aktas Yilmaz, Cigdem Ozkan, Mujde Akturk, Fusun Balos Toruner
Gynecological Endocrinology.2019; 35(8): 714. CrossRef - Serum adenosine deaminase activity and coronary artery disease: a retrospective case-control study based on 9929 participants
Chao Xuan, Qing-Wu Tian, Shao-Yan Zhang, Hui Li, Ting-Ting Tian, Peng Zhao, Kang Yue, Yan-Yan Ling, Guo-Wei He, Li-Min Lun
Therapeutic Advances in Chronic Disease.2019; 10: 204062231989153. CrossRef - Metabolites related to purine catabolism and risk of type 2 diabetes incidence; modifying effects of the TCF7L2-rs7903146 polymorphism
Christopher Papandreou, Jun Li, Liming Liang, Mònica Bulló, Yan Zheng, Miguel Ruiz-Canela, Edward Yu, Marta Guasch-Ferré, Cristina Razquin, Clary Clish, Dolores Corella, Ramon Estruch, Emilio Ros, Montserrat Fitó, Fernando Arós, Lluís Serra-Majem, Nuria R
Scientific Reports.2019;[Epub] CrossRef - Current status of G-protein coupled receptors as potential targets against type 2 diabetes mellitus
Mehboob Hoque, Safdar Ali, Muddasarul Hoda
International Journal of Biological Macromolecules.2018; 118: 2237. CrossRef - Endoglin inhibition by sodium acetate and flutamide ameliorates cardiac defective G6PD-dependent antioxidant defense in gestational testosterone-exposed rats
Lawrence A. Olatunji, Emmanuel D. Areola, Olufunto O. Badmus
Biomedicine & Pharmacotherapy.2018; 107: 1641. CrossRef - Sodium acetate and androgen receptor blockade improve gestational androgen excess-induced deteriorated glucose homeostasis and antioxidant defenses in rats: roles of adenosine deaminase and xanthine oxidase activities
Taofeek O. Usman, Emmanuel D. Areola, Olufunto O. Badmus, InKyeom Kim, Lawrence A. Olatunji
The Journal of Nutritional Biochemistry.2018; 62: 65. CrossRef - ADENOSINE DEAMINASE ACTIVITY IN TYPE 2 DIABETES MELLITUS
Farija Peruvankuzhiyil, Lavanya Madhavan, Manaloor George Joseraj
Journal of Evidence Based Medicine and Healthcare.2017; 4(5): 238. CrossRef - Adenosine signaling in diabetes mellitus and associated cardiovascular and renal complications
Maria Peleli, Mattias Carlstrom
Molecular Aspects of Medicine.2017; 55: 62. CrossRef - The Adenosinergic System in Diabetic Retinopathy
J. Vindeirinho, A. R. Santiago, C. Cavadas, A. F. Ambrósio, P. F. Santos
Journal of Diabetes Research.2016; 2016: 1. CrossRef - Upregulation of inducible NO synthase by exogenous adenosine in vascular smooth muscle cells activated by inflammatory stimuli in experimental diabetes
Alberto Nassi, Francesca Malorgio, Serena Tedesco, Andrea Cignarella, Rosa Maria Gaion
Cardiovascular Diabetology.2016;[Epub] CrossRef - Reduced adenosine A2a receptor–mediated efferent arteriolar vasodilation contributes to diabetes-induced glomerular hyperfiltration
Patrik Persson, Peter Hansell, Fredrik Palm
Kidney International.2015; 87(1): 109. CrossRef - CD26/DPP4 Levels in Peripheral Blood and T Cells in Patients With Type 2 Diabetes Mellitus
Sang Ah Lee, Young Ree Kim, Eun Jin Yang, Eun-Jeong Kwon, Sun Hyung Kim, Sung Ha Kang, Doek Bae Park, Byung-Chul Oh, Jinseok Kim, Sang Taek Heo, Gwanpyo Koh, Dae Ho Lee
The Journal of Clinical Endocrinology & Metabolism.2013; 98(6): 2553. CrossRef - Raised Serum Adenosine Deaminase Level in Nonobese Type 2 Diabetes Mellitus
Vineet Kumar Khemka, Debajit Bagchi, Arindam Ghosh, Oishimaya Sen, Aritri Bir, Sasanka Chakrabarti, Anindita Banerjee
The Scientific World Journal.2013; 2013: 1. CrossRef - Phosphodiesterase III Inhibition Increases cAMP Levels and Augments the Infarct Size Limiting Effect of a DPP-4 Inhibitor in Mice with Type-2 Diabetes Mellitus
Yochai Birnbaum, Alexander C. Castillo, Jinqiao Qian, Shukuan Ling, Hongmei Ye, Jose R. Perez-Polo, Mandeep Bajaj, Yumei Ye
Cardiovascular Drugs and Therapy.2012; 26(6): 445. CrossRef - Serum Adenosine deaminase activity in type 2 Diabetes Mellitus patients
M. N. Vanitha Gowda, K. C. Vasudha, S. Reshma, K. J. Sujatha
International Journal of Diabetes in Developing Countries.2012; 32(3): 176. CrossRef - Cyclic AMP and PKA: How can a Lot of Good Come from the Potentially Bad?
Barbara Huisamen
Cardiovascular Drugs and Therapy.2012; 26(6): 435. CrossRef - Gadd45α: A Novel Diabetes-Associated Gene Potentially Linking Diabetic Cardiomyopathy and Baroreflex Dysfunction
Ning Wang, Chao Yang, Fang Xie, Lihua Sun, Xiaolin Su, Ying Wang, Ran Wei, Rong Zhang, Xia Li, Baofeng Yang, Jing Ai, Rajesh Gopalrao Katare
PLoS ONE.2012; 7(12): e49077. CrossRef - The CD39-Adenosinergic Axis in the Pathogenesis of Immune and Nonimmune Diabetes
Joanne S. J. Chia, Jennifer L. McRae, Peter J. Cowan, Karen M. Dwyer
Journal of Biomedicine and Biotechnology.2012; 2012: 1. CrossRef

 KDA
KDA PubReader
PubReader Cite
Cite