- Current
- Browse
- Collections
-
For contributors
- For Authors
- Instructions to authors
- Article processing charge
- e-submission
- For Reviewers
- Instructions for reviewers
- How to become a reviewer
- Best reviewers
- For Readers
- Readership
- Subscription
- Permission guidelines
- About
- Editorial policy
Articles
- Page Path
- HOME > Diabetes Metab J > Volume 47(1); 2023 > Article
-
ReviewGuideline/Fact Sheet Lipid Management in Korean People with Type 2 Diabetes Mellitus: Korean Diabetes Association and Korean Society of Lipid and Atherosclerosis Consensus Statement
-
Ye Seul Yang1
 , Hack-Lyoung Kim2,3, Sang-Hyun Kim2,3
, Hack-Lyoung Kim2,3, Sang-Hyun Kim2,3 , Min Kyong Moon2,3
, Min Kyong Moon2,3 , on Behalf of Committee of Clinical Practice Guideline, Korean Diabetes Association and Clinical Practice Guideline Committee, Korean Society of Lipid and Atherosclerosis
, on Behalf of Committee of Clinical Practice Guideline, Korean Diabetes Association and Clinical Practice Guideline Committee, Korean Society of Lipid and Atherosclerosis -
Diabetes & Metabolism Journal 2023;47(1):1-9.
DOI: https://doi.org/10.4093/dmj.2022.0448
Published online: January 20, 2023
1Department of Medicine, Seoul National University College of Medicine, Seoul, Korea
2Department of Internal Medicine, Seoul Metropolitan Government Seoul National University Boramae Medical Center, Seoul, Korea
3Department of Internal Medicine, Seoul National University College of Medicine, Seoul, Korea
-
Corresponding authors: Min Kyong Moon
 Division of Endocrinology and Metabolism, Department of Internal Medicine, Seoul Metropolitan Government Seoul National University Boramae Medical Center, Seoul National University College of Medicine, 20 Boramae-ro 5-gil, Dongjak-gu, Seoul 07061, Korea E-mail: mkmoon@snu.ac.kr
Division of Endocrinology and Metabolism, Department of Internal Medicine, Seoul Metropolitan Government Seoul National University Boramae Medical Center, Seoul National University College of Medicine, 20 Boramae-ro 5-gil, Dongjak-gu, Seoul 07061, Korea E-mail: mkmoon@snu.ac.kr -
Sang-Hyun Kim
 Division of Cardiology, Department of Internal Medicine, Seoul Metropolitan Government Seoul National University Boramae Medical Center, Seoul National University College of Medicine, 20 Boramae-ro 5-gil, Dongjak-gu, Seoul 07061, Korea E-mail: shkimmd@snu.ac.kr
Division of Cardiology, Department of Internal Medicine, Seoul Metropolitan Government Seoul National University Boramae Medical Center, Seoul National University College of Medicine, 20 Boramae-ro 5-gil, Dongjak-gu, Seoul 07061, Korea E-mail: shkimmd@snu.ac.kr - This manuscript is simultaneously published in the Diabetes & Metabolism Journal and the Journal of Lipid and Atherosclerosis by the Korean Diabetes Association and the Korean Society of Lipid and Atherosclerosis.
Copyright © 2023 Korean Diabetes Association
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
ABSTRACT
- Dyslipidemia in patients with diabetes is an important treatment target as a modifiable risk factor for cardiovascular disease (CVD). Although the primary treatment goal for dyslipidemia is to control low-density lipoprotein cholesterol (LDL-C), achieving this goal remains suboptimal according to recent studies. It is important to set the target goal for LDL-C control based on an accurate risk assessment for CVD. Here, we summarize the latest evidence on lipid management in patients with diabetes and present a consensus of the Korean Diabetes Association and Korean Society of Lipid and Atherosclerosis on the treatment goals of LDL-C according to the duration of diabetes, presence of CVD, target organ damage, or major cardiovascular risk factors. In patients with type 2 diabetes mellitus (T2DM) and CVD, an LDL-C goal of <55 mg/dL and a reduction in LDL-C level by 50% or more from the baseline is recommended. For the primary prevention of CVD in patients with T2DM with a duration of diabetes ≥10 years, major cardiovascular risk factors, or target organ damage, an LDL-C goal of <70 mg/dL is recommended. In patients with T2DM with a duration of diabetes <10 years and no major cardiovascular risk factors, an LDL-C goal of <100 mg/dL is recommended.
- Cardiovascular disease (CVD) is the leading cause of death in patients with diabetes mellitus, although cardiovascular complications and death from CVD have recently been decreasing [1]. Dyslipidemia in patients with diabetes is an important treatment target because mortality from CVD is two to four times higher in patients with diabetes than in those without [2,3]. In the UK Prospective Diabetes Study (UKPDS), low-density lipoprotein cholesterol (LDL-C) was the strongest predictor of coronary heart disease in patients with type 2 diabetes mellitus (T2DM) among several risk factors for CVD, and each 39 mg/dL increase in LDL-C increased the coronary heart disease risk by about 60% [4]. Lowering the LDL-C level is the primary target for CVD prevention, but the actual goals differ among various guidelines. In this report, we present the experts’ opinions on lipid management in Koreans with T2DM from a thorough review of previous randomized controlled trials, worldwide guidelines, and Korean data. The Korean Diabetes Association (KDA) and Korean Society of Lipid and Atherosclerosis (KSoLA) have reached a consensus for lipid management in patients with T2DM.
INTRODUCTION
- The treatment goal of LDL-C in patients with diabetes was derived from randomized controlled trials on primary and secondary prevention of CVD using drug interventions, meta-analyses, and systematic reviews of those studies [5-10]. The benefits of statin treatment for CVD have been consistently demonstrated in studies of patients with T2DM and subgroup analyses of patients with diabetes in several clinical studies of statins. The Collaborative Atorvastatin Diabetes Study (CARDS) is a representative primary prevention study of statins in patients with T2DM [11]. Atorvastatin (10 mg) was administered to patients with T2DM aged 40 to 75 years with one or more cardiovascular risk factors; the mean LDL-C concentration was 72 mg/dL, which was reduced by 39% compared to baseline, and the risk of major cardiovascular events was reduced by 37% [11]. Representative studies that demonstrated the secondary prevention effect of statin therapy in patients with T2DM with prior CVD are the Treating to New Targets (TNT) [6] and Pravastatin or Atorvastatin Evaluation and Infection Trial (PROVE-IT) [12]. In these studies, when LDL-C concentration was maintained at 57 to 77 mg/dL by administering 80 mg of atorvastatin, the incidence of CVD was significantly reduced compared to the group for which LDL-C concentration was maintained at 81 to 99 mg/dL with atorvastatin 10 mg or pravastatin 40 mg [6,12]. In a meta-analysis of 14 randomized clinical trials, when LDL-C was reduced by 1 mmol/L with statin therapy, there was a 23% reduction in major cardiovascular events over 5 years, regardless of baseline LDL-C concentration or other underlying characteristics, and the benefits of statin treatment were similar between type 1 diabetes mellitus (T1DM) and T2DM [7]. Because patients with T2DM benefited from a relative risk reduction comparable to that of non-diabetic patients in this meta-analysis by the Cholesterol Treatment Trialists’ Collaboration [7], the benefit of absolute reduction in LDL-C by statin therapy can be greater in patients with diabetes, considering the higher absolute risk, than in patients without diabetes. Recent trials evaluating the effects of the combination of statins and ezetimibe or proprotein convertase subtilisin/kexin type 9 (PCSK9) inhibitors in patients with atherosclerotic CVD, such as the IMProved Reduction of Outcomes: Vytorin Efficacy International Trial (IMPROVE-IT) [13], Further Cardiovascular Outcomes Research with PCSK9 Inhibition in Subjects With Elevated Risk (FOURIER) [14], and the Evaluation of Cardiovascular Outcomes After an Acute Coronary Syndrome During Treatment With Alirocumab (ODYSSEY OUTCOMES) trial [15], showed that even when LDL-C was lowered to less than 70 mg/dL, further reduction of LDL-C lowered the risk of major cardiovascular events.
- The IMPROVE-IT study included 18,144 patients who were hospitalized for acute coronary syndrome within 10 days of the study. In the statin and ezetimibe combination treatment group, LDL-C was 15.8 mg/dL lower than that in the statin monotherapy group (53.7 mg/dL vs. 69.5 mg/dL as the median time-weighted average LDL-C level), and the relative risk of CVD significantly decreased by 6.4% at 7 years of follow-up [13]. In the subgroup analysis, the relative risk of CVD was reduced by 14% in patients with diabetes, indicating that the preventive effect of CVD was greater among such patients [16].
- In the FOURIER study including 27,564 patients with CVD, the LDL-C levels reduced by 59% (from 92 to 30 mg/dL) in the group in which evolocumab was added to statin. The relative risk of CVD was reduced by 15% over a median of 2.2 years [14]. A subgroup analysis of 11,031 patients with diabetes in this study showed similar results [17]. In the ODYSSEY OUTCOMES trial including 18,924 patients with recent acute coronary syndrome, the risk of CVD was significantly reduced by 15% over a median of 2.8 years in the group in which alirocumab was added to statins, with an LDL-C level of 53.3 mg/dL at 48 months [15]. A subgroup analysis of patients with diabetes showed similar results [18].
EVIDENCE FOR DYSLIPIDEMIA TREATMENT GOALS
- Not all patients with diabetes have the same CVD risk. Long duration of diabetes (for T2DM ≥10 years and for T1DM ≥20 years), albuminuria (≥30 mg/g of urine albumin/creatinine ratio), estimated glomerular filtration rate (eGFR) <60 mL/min/1.73 m2, retinopathy, neuropathy, and ankle-brachial index <0.9 are well-known risk factors that increase cardiovascular risk in patients with diabetes [19]. In the 2019 European Society of Cardiology (ESC) and European Atherosclerosis Society (EAS) guidelines [20], diabetic patients with (1) target organ damage defined as albuminuria, chronic kidney disease (CKD) with an eGFR of <30 mL/min/1.73 m2, retinopathy, or neuropathy; (2) three or more major risk factors including age, hypertension, dyslipidemia, smoking, and obesity; and (3) early onset T1DM with a long duration of >20 years were classified as a very high-risk group with a 10-year cardiovascular mortality risk exceeding 10%. In these patient groups, the LDL-C target is recommended to be a reduction of 50% or more from the baseline and <1.4 mmol/L (<55 mg/dL) [20].
- In a 9.3-year follow-up study of 248,000 Korean patients with T2DM aged 30 to 90 years using the Korean National Health Insurance Service (NHIS) database, among diabetic patients without prior CVD, the incidence of myocardial infarction and stroke was increased when accompanied by CKD (eGFR <60 mL/min/1.73 m2), hypertension, long duration of diabetes, and three or more cardiovascular risk factors [21]. In particular, the incidence rate of CVD was similar to or higher in patients with three or more major risk factors (14.1/1,000-person years) or CKD (18.3/1,000-person years) than in patients with prior CVD (14.1/1,000-person years) [21].
RISK STRATIFICATION AMONG PEOPLE WITH DIABETES
- According to the Diabetes Fact Sheet 2021 of the KDA, 76.5% of Korean adults with diabetes had hyper-LDL-cholesterolemia, and only 38.3% of adults achieved the target level of LDL-C (<100 mg/dL) [22]. In a recent retrospective observational study using electronic medical record data of 2,000 T2DM patients at 15 hospitals, LDL-C goal achievement remained suboptimal according to several current guidelines for dyslipidemia management [23]: 34.9% to 55.2% in very high-risk patients according to the KDA guidelines [24], 15.7% to 26.6% according to the ESC and EAS guidelines [20], and only 15.5% according to the American Diabetes Association guidelines [25]. In a study using the Korean NHIS database including approximately 153,000 patients with diabetes, LDL-C goal attainment rates were 32.6% in patients without a high risk of CVD (<100 mg/dL) and 12.2% in patients with a high risk of CVD (<70 mg/dL) [26]. When assessing the gap between real-world practice and clinical guidelines, investigators’ assessment of risk was underestimated by 71.6% compared to that by clinical guidelines [27]. Physicians’ perceptions of the target achievement rate of LDL-C were higher than the actual achievement rate (70.6% vs. 47.4%) [28], and physician satisfaction with patients’ LDL-C levels was the primary reason for the non-intensification of statin therapy [27].
CURRENT STATUS OF LIPID MANAGEMENT IN KOREAN PATIENTS WITH T2DM
- The primary treatment goal for dyslipidemia in diabetic patients is the control of LDL-C. Non-high-density lipoprotein cholesterol (HDL-C) or apolipoprotein B can be used as a target when LDL-C has reached the target level but hypertriglyceridemia persists, or when the blood sample is drawn in a non-fasting state [29]. The target goal of non-HDL-C is to add 30 mg/dL to the existing target LDL-C level (Table 1).
- Low-density lipoprotein cholesterol
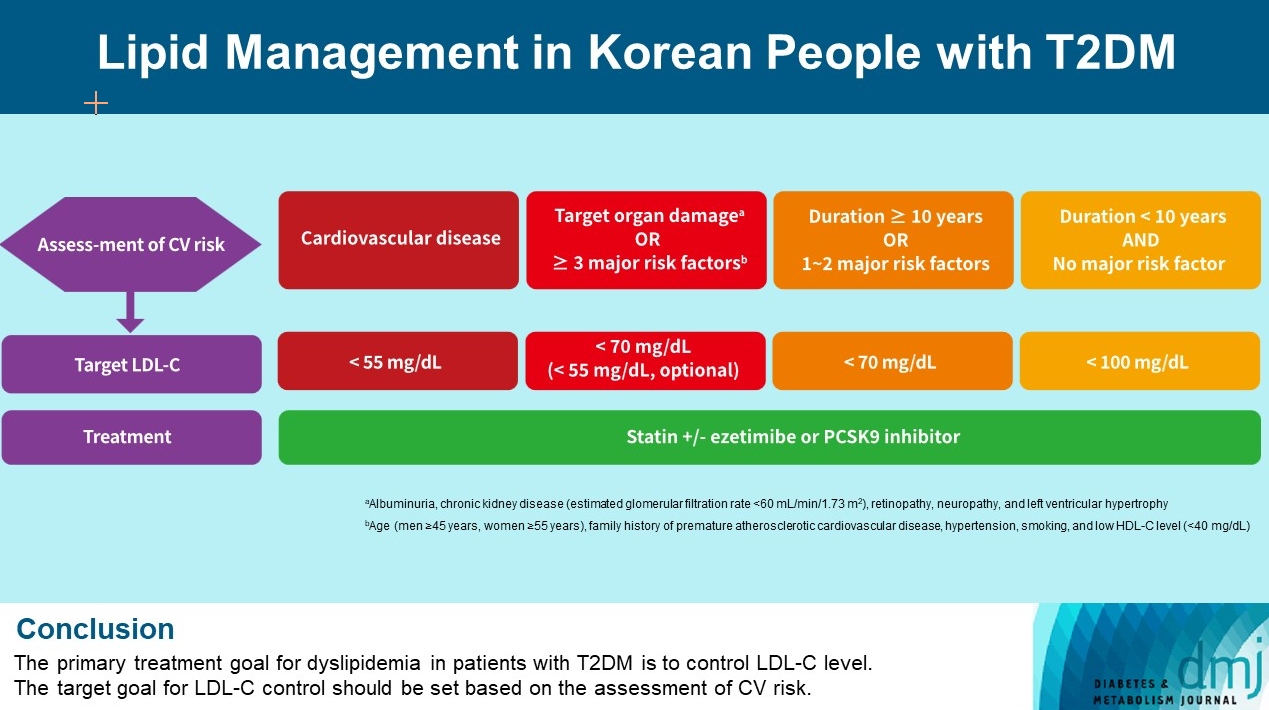
- Among people with diabetes, cardiovascular risk varies according to comorbidities and accompanying cardiovascular risk factors. Therefore, it is important to identify the patient’s comorbidities, including CVD and target organ damage (albuminuria, CKD [eGFR <60 mL/min/1.73 m2], retinopathy, neuropathy, and left ventricular hypertrophy), major cardiovascular risk factors (age, family history of premature atherosclerotic CVD, hypertension, smoking, and low HDL-C), and duration of diabetes to determine the LDL-C treatment goal for each patient with T2DM.
- Table 1 shows the LDL-C treatment goals according to cardiovascular risk. In patients with T2DM and CVD, an LDL-C goal of <55 mg/dL and a reduction in LDL-C level by 50% or more from the baseline is recommended. For the primary prevention of CVD in patients with T2DM who have a diabetes duration ≥10 years or who have major cardiovascular risk factors or target organ damage, an LDL-C goal of <70 mg/dL is recommended. In patients with T2DM who have any target organ damage or more than three major cardiovascular risk factors, an LDL-C goal of <55 mg/dL is considered an option. In patients with T2DM who have a diabetes duration <10 years and no major cardiovascular risk factors, an LDL-C target of <100 mg/dL is recommended.
- Triglyceride
- The risk of acute pancreatitis increases when the triglyceride concentration is elevated to 500 mg/dL or higher; therefore, control is required. Whether hypertriglyceridemia is a risk factor for CVD remains controversial. Triglyceride elevation reflects the number of residual lipoprotein particles, which are factors other than LDL-C that promote atherosclerosis and are associated with an increase in small dense LDL particles. Therefore, the opinion that it is one of the risk factors for CVD prevails [30]. Triglycerides are particularly increased in patients with overweight, obesity, metabolic syndrome, and diabetes. In the 2001 National Cholesterol Education Program-Adult Treatment Panel (NECP-ATP) III report [31,32], 150 mg/dL or more of triglycerides was suggested as a diagnostic criterion for metabolic syndrome and the normal range of triglycerides is <150 mg/dL. Therefore, this criterion is recommended as a control mark for triglycerides and substituted by non-HDL-C level as a target.
- High-density lipoprotein cholesterol
- Based on the study that an increase in HDL-C concentration decreased mortality by CVD [33], low HDL-C (less than 40 mg/dL) was defined as a risk factor for CVD and a diagnostic element of metabolic syndrome in the 2001 NECP-ATP III guidelines [31]. Although the upper limit of the treatment target for HDL-C is not specified, it is recommended to pay attention to low HDL-C as a cardiovascular risk factor and maintain a concentration of >40 mg/dL in men and >50 mg/dL in women.
TREATMENT GOAL
- Lifestyle intervention
- In a randomized controlled trial of the effects of a Mediterranean-style diet on cardiovascular risk in people with T2DM or cardiovascular risk factors, the risk of CVD was reduced by 31% compared to the control group [34]. Medical nutrition therapy and lifestyle modifications, including increased physical activity and weight loss in patients with obesity, can improve lipid concentrations [35]. Medical nutrition therapy should be individualized in consideration of the patient’s age, type of diabetes, medications, lipid profile, and comorbidities. Patients should be encouraged to reduce their intake of saturated fat, cholesterol, and trans-fat and increase their intake of omega-3 fatty acids and dietary fiber. Optimizing glycemic control can improve lipid profiles, especially in patients with diabetes who have poor glycemic control and high triglyceride levels. In addition, abstinence from alcohol and weight loss are effective in treating hypertriglyceridemia.
- Pharmacological treatments
- Statins are the first-line treatment for patients with diabetes and dyslipidemia. If the LDL-C target goal is not achieved with the usual statin dose, the dose should be increased to the maximum tolerated dose or replaced with high-intensity statins [36,37]. In a study of patients with diabetes, statin treatment showed significant efficacy in both primary and secondary prevention of CVD in previously described studies, such as the CADS, TNT, and PROVE-IT studies.
- Compared to statin monotherapy, ezetimibe combined with statins can lower LDL-C concentrations by an additional 15% to 20% [38,39]. IMPROVE-IT is a representative study that showed the effect of statin and ezetimibe combination treatment in reducing the incidence of CVD. The PCSK9 inhibitors evolocumab and alirocumab were added for patients with a high risk of CVD or T2DM who were using statins at the maximum tolerated dose; LDL-C concentration was further reduced by 36% to 59% [40-42]. In a systematic review and meta-analysis of 39 randomized controlled trials, including a total of 66,478 patients, the PCSK9 inhibitor group showed no difference in overall mortality compared to the control group, but the risk of myocardial infarction, stroke, and coronary revascularization was significantly low [43]. Therefore, the addition of ezetimibe or PCSK9 inhibitors should be considered in patients with diabetes and CVD if the target LDL-C goal is not met by the maximum tolerable dose of statins.
- There have been studies on statin and omega-3 fatty acid combination therapy, but this combination therapy has not shown any clear benefit. The results of studies on the prevention of CVD by omega-3 fatty acids are inconsistent. In the Reduction of Cardiovascular Events with Icosapent Ethyl-Intervention Trial (REDUCE-IT) study, a combination treatment with statins and 4 g icosapent ethyl, which is a highly purified and stable eicosapentaenoic acid (EPA), showed a preventive effect against CVD [44]. The same effect was found in a subgroup analysis of patients with diabetes. However, in the Outcomes Study to Assess Statin Residual Risk Reduction with Epanova in High Cardiovascular Risk Patients with Hypertriglyceridemia (STRENGTH) study, which included 70% diabetic patients, the combination treatment of statins and 4 g omega-3 acids EPA and docosahexaenoic acid (DHA) per day did not show any significant difference in the composite outcome of major CVD compared to that with corn oil [45].
- Whether the combination of statins and fibrates helps lower CVD events in patients with T2DM is controversial. In the Action to Control Cardiovascular Risk in Diabetes (ACCORD) lipid study, the combination of statins and fibrates failed to lower the risk of CVD when compared to statin monotherapy [46]. However, in the subgroup analysis, a possible CVD preventive benefit was observed in patients with both a high baseline triglyceride and a low baseline HDL-C level, which is typical of diabetic dyslipidemia [46]. A similar result was shown in the Fenofibrate Intervention and Event Lowering in Diabetes (FIELD) study [47,48]; therefore, there was an effort to estimate the expected treatment effect of fenofibrate in patients with T2DM and dyslipidemia [49]. In a recent propensity-matched cohort study in Korea, the risk of major cardiovascular events was reduced in adults with metabolic syndrome using fenofibrate as an add-on to statin treatment and also in diabetic patients in a subgroup analysis [50]. However, in the most recently published the Pemafibrate to Reduce Cardiovascular Outcomes by Reducing Triglycerides in Patients with Diabetes (PROMINENT) trial, pemafibrate treatment did not reduce the risk of CVD in patients with T2DM and dyslipidemia, in whom 95.7% of the study population were already receiving statins, even though it significantly reduced triglyceride, very-low-density lipoprotein cholesterol, measured remnant cholesterol, and apolipoprotein C-III levels [51]. This suggests that triglyceride-lowering treatment using fibrates has limitations in reducing the risk of residual CVD.
- In the case of hypertriglyceridemia, it is necessary to determine if there are secondary causes that may increase triglyceride levels (weight gain, drinking, excessive carbohydrate intake, CKD, diabetes, hypothyroidism, pregnancy, and use of estrogen, tamoxifen, and glucocorticoids) and any genetic factors that may cause abnormalities in lipid metabolism [52]. Lifestyle modifications such as weight loss, increased physical activity, and medical nutrition therapy, including abstinence from alcohol, are effective in the treatment of hypertriglyceridemia in diabetic patients and may reduce the risk factors for atherosclerotic CVD in some patients [53]. If hyperglycemia is not controlled, hypertriglyceridemia is exacerbated, and strict glycemic control can lower triglyceride levels. If there is a secondary cause, treatment for it is prioritized.
- In cases of severe hypertriglyceridemia with a triglyceride concentration ≥500 mg/dL, a low-fat diet, abstinence from alcohol, and immediate drug treatment such as omega-3 fatty acids or fibrate to prevent acute pancreatitis is considered [54]. If the triglyceride concentration is 200 to 499 mg/dL, the primary treatment goal is to lower LDL-C to less than the targeted level, according to the cardiovascular risk. If triglycerides persist at >200 mg/dL even after achieving the LDL-C target goal through therapeutic lifestyle adjustment and statin treatment, drug treatments such as fibrate and omega-3 fatty acids can be considered to lower the triglycerides. Combination therapy can be considered when triglyceride levels do not reach the target even after administration of a single drug for triglyceride control.
TREATMENTS
LDL-C lowering therapy
1) Statins
2) Combination of statins and ezetimibe/PCSK9 inhibitor
3) Combination of statins and omega-3 fatty acid
4) Combination of statins and fibrates
Treatment for hypertriglyceridemia
- Efforts have been made to suggest appropriate lipid management targets for Koreans using retrospective data [21,55-58]. However, there is a lack of independent studies to establish lipid management goals in Korean with diabetes or to evaluate whether achieving the treatment goals based on evidence from other ethnic groups is effective in preventing CVD in Korean patients with diabetes. Therefore, well-designed randomized clinical trials targeting Koreans are needed in the future to strengthen the evidence of this statement.
CURRENT LIMITATIONS AND RESEARCH NEEDS
- 1. The primary treatment goal for dyslipidemia in patients with diabetes is to control their LDL-C levels.
- 2. To determine the LDL-C treatment goal for each patient with T2DM, the patient’s comorbidities, including CVD and target organ damage (albuminuria, CKD, retinopathy, neuropathy, and left ventricular hypertrophy), major cardiovascular risk factors (age, family history of premature atherosclerotic CVD, hypertension, smoking, and low HDL-C), and duration of diabetes must be identified first.
- 3. In patients with T2DM and CVD, an LDL-C goal of <55 mg/dL and a reduction in LDL-C level by 50% or more from the baseline is recommended.
- 4. For the primary prevention of CVD in patients with T2DM who have a duration of diabetes ≥10 years or who have major cardiovascular risk factors or target organ damage, an LDL-C goal of <70 mg/dL is recommended.
- 5. For the primary prevention of CVD in patients with T2DM who have any target organ damage or more than three major cardiovascular risk factors, an LDL-C goal of <55 mg/dL is considered an option.
- 6. For the primary prevention of CVD in patients with T2DM who have a duration of diabetes <10 years and no major cardiovascular risk factors, an LDL-C goal of <100 mg/dL is recommended.
- 7. Statin is the first-line treatment for patients with diabetes and dyslipidemia.
- 8. The addition of ezetimibe or PCSK9 inhibitors should be considered for patients with diabetes and CVD if the target LDL-C goal is not met by a maximum tolerable dose of statin.
CONSENSUS STATEMENT
-
CONFLICTS OF INTEREST
No potential conflict of interest relevant to this article was reported.
-
FUNDING
None
NOTES
-
Acknowledgements
- This work was performed with the cooperation of the Korean Diabetes Association and Korean Society of Lipid and Atherosclerosis.
| Risk category | LDL-C, mg/dL | Non-HDL-C, mg/dL |
|---|---|---|
| Cardiovascular diseasea | <55 | <85 |
| Target organ damageb or major risk factorc or duration of diabetes ≥10 years | <70d | <100 |
| Duration of diabetes <10 years and no major risk factor | <100 | <130 |
LDL-C, low-density lipoprotein cholesterol; HDL-C, high-density lipoprotein cholesterol.
a Reducing LDL-C by ≥50% from the baseline level is also recommended,
b Albuminuria, chronic kidney disease (estimated glomerular filtration rate <60 mL/min/1.73 m2), retinopathy, neuropathy, and left ventricular hypertrophy,
c Age (men ≥45 years, women ≥55 years), family history of premature atherosclerotic cardiovascular disease, hypertension, smoking, and low HDL-C level (<40 mg/dL),
d In patients with any target organ damage or more than three major cardiovascular risk factors, an LDL-C goal of <55 mg/dL is considered an option.
- 1. Park JH, Ha KH, Kim BY, Lee JH, Kim DJ. Trends in cardiovascular complications and mortality among patients with diabetes in South Korea. Diabetes Metab J 2021;45:120-4.ArticlePubMedPDF
- 2. Haffner SM, Lehto S, Ronnemaa T, Pyorala K, Laakso M. Mortality from coronary heart disease in subjects with type 2 diabetes and in nondiabetic subjects with and without prior myocardial infarction. N Engl J Med 1998;339:229-34.ArticlePubMed
- 3. Kim KJ, Kwon TY, Yu S, Seo JA, Kim NH, Choi KM, et al. Ten-year mortality trends for adults with and without diabetes mellitus in South Korea, 2003 to 2013. Diabetes Metab J 2018;42:394-401.ArticlePubMedPMCPDF
- 4. Stevens RJ, Kothari V, Adler AI, Stratton IM; United Kingdom Prospective Diabetes Study (UKPDS) Group. The UKPDS risk engine: a model for the risk of coronary heart disease in type II diabetes (UKPDS 56). Clin Sci (Lond) 2001;101:671-9.ArticlePubMed
- 5. Nissen SE, Tuzcu EM, Schoenhagen P, Brown BG, Ganz P, Vogel RA, et al. Effect of intensive compared with moderate lipid-lowering therapy on progression of coronary atherosclerosis: a randomized controlled trial. JAMA 2004;291:1071-80.ArticlePubMed
- 6. Shepherd J, Barter P, Carmena R, Deedwania P, Fruchart JC, Haffner S, et al. Effect of lowering LDL cholesterol substantially below currently recommended levels in patients with coronary heart disease and diabetes: the Treating to New Targets (TNT) study. Diabetes Care 2006;29:1220-6.PubMed
- 7. Cholesterol Treatment Trialists’ (CTT) Collaborators. Efficacy of cholesterol-lowering therapy in 18,686 people with diabetes in 14 randomised trials of statins: a meta-analysis. Lancet 2008;371:117-25.ArticlePubMed
- 8. Brugts JJ, Yetgin T, Hoeks SE, Gotto AM, Shepherd J, Westendorp RG, et al. The benefits of statins in people without established cardiovascular disease but with cardiovascular risk factors: meta-analysis of randomised controlled trials. BMJ 2009;338:b2376.ArticlePubMedPMC
- 9. Cholesterol Treatment Trialists’ (CTT) Collaboration. Efficacy and safety of more intensive lowering of LDL cholesterol: a meta-analysis of data from 170,000 participants in 26 randomised trials. Lancet 2010;376:1670-81.ArticlePubMedPMC
- 10. Heart Protection Study Collaborative Group. MRC/BHF heart protection study of cholesterol lowering with simvastatin in 20,536 high-risk individuals: a randomised placebo-controlled trial. Lancet 2002;360:7-22.ArticlePubMed
- 11. Colhoun HM, Betteridge DJ, Durrington PN, Hitman GA, Neil HA, Livingstone SJ, et al. Primary prevention of cardiovascular disease with atorvastatin in type 2 diabetes in the Collaborative Atorvastatin Diabetes Study (CARDS): multicentre randomised placebo-controlled trial. Lancet 2004;364:685-96.ArticlePubMed
- 12. Ahmed S, Cannon CP, Murphy SA, Braunwald E. Acute coronary syndromes and diabetes: is intensive lipid lowering beneficial? Results of the PROVE IT-TIMI 22 trial. Eur Heart J 2006;27:2323-9.ArticlePubMed
- 13. Cannon CP, Blazing MA, Giugliano RP, McCagg A, White JA, Theroux P, et al. Ezetimibe added to statin therapy after acute coronary syndromes. N Engl J Med 2015;372:2387-97.ArticlePubMed
- 14. Sabatine MS, Giugliano RP, Keech AC, Honarpour N, Wiviott SD, Murphy SA, et al. Evolocumab and clinical outcomes in patients with cardiovascular disease. N Engl J Med 2017;376:1713-22.ArticlePubMed
- 15. Schwartz GG, Steg PG, Szarek M, Bhatt DL, Bittner VA, Diaz R, et al. Alirocumab and cardiovascular outcomes after acute coronary syndrome. N Engl J Med 2018;379:2097-107.ArticlePubMed
- 16. Giugliano RP, Cannon CP, Blazing MA, Nicolau JC, Corbalan R, Spinar J, et al. Benefit of adding ezetimibe to statin therapy on cardiovascular outcomes and safety in patients with versus without diabetes mellitus: results from IMPROVE-IT (Improved Reduction of Outcomes: Vytorin Efficacy International Trial). Circulation 2018;137:1571-82.ArticlePubMed
- 17. Sabatine MS, Leiter LA, Wiviott SD, Giugliano RP, Deedwania P, De Ferrari GM, et al. Cardiovascular safety and efficacy of the PCSK9 inhibitor evolocumab in patients with and without diabetes and the effect of evolocumab on glycaemia and risk of new-onset diabetes: a prespecified analysis of the FOURIER randomised controlled trial. Lancet Diabetes Endocrinol 2017;5:941-50.ArticlePubMed
- 18. Ray KK, Colhoun HM, Szarek M, Baccara-Dinet M, Bhatt DL, Bittner VA, et al. Effects of alirocumab on cardiovascular and metabolic outcomes after acute coronary syndrome in patients with or without diabetes: a prespecified analysis of the ODYSSEY OUTCOMES randomised controlled trial. Lancet Diabetes Endocrinol 2019;7:618-28.PubMed
- 19. Grundy SM, Stone NJ, Bailey AL, Beam C, Birtcher KK, Blumenthal RS, et al. 2018 AHA/ACC/AACVPR/AAPA/ABC/ACPM/ADA/AGS/APhA/ASPC/NLA/PCNA guideline on the management of blood cholesterol: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Circulation 2019;139:e1082-143.PubMed
- 20. Mach F, Baigent C, Catapano AL, Koskinas KC, Casula M, Badimon L, et al. 2019 ESC/EAS guidelines for the management of dyslipidaemias: lipid modification to reduce cardiovascular risk. Eur Heart J 2020;41:111-88.ArticlePubMedPDF
- 21. Moon MK, Noh J, Rhee EJ, Park SH, Kim HC, Kim BJ, et al. Cardiovascular outcomes according to comorbidities and low-density lipoprotein cholesterol in Korean people with type 2 diabetes mellitus. Diabetes Metab J 2023;47:45-58.ArticlePubMedPMCPDF
- 22. Bae JH, Han KD, Ko SH, Yang YS, Choi JH, Choi KM, et al. Diabetes fact sheet in Korea 2021. Diabetes Metab J 2022;46:417-26.ArticlePubMedPMCPDF
- 23. Yun SJ, Jeong IK, Cha JH, Lee J, Cho HC, Choi SH, et al. Current status of low-density lipoprotein cholesterol target achievement in patients with type 2 diabetes mellitus in Korea compared with recent guidelines. Diabetes Metab J 2021;46:464-75.ArticlePubMedPDF
- 24. Kim MK, Ko SH, Kim BY, Kang ES, Noh J, Kim SK, et al. 2019 Clinical practice guidelines for type 2 diabetes mellitus in Korea. Diabetes Metab J 2019;43:398-406.ArticlePubMedPMCPDF
- 25. American Diabetes Association. 10. Cardiovascular disease and risk management: standards of medical care in diabetes-2019. Diabetes Care 2019;42(Suppl 1):S103-23.
- 26. Yang YS, Yang BR, Kim MS, Hwang Y, Choi SH. Low-density lipoprotein cholesterol goal attainment rates in high-risk patients with cardiovascular diseases and diabetes mellitus in Korea: a retrospective cohort study. Lipids Health Dis 2020;19:5.ArticlePubMedPMCPDF
- 27. Yang YS, Lee SY, Kim JS, Choi KM, Lee KW, Lee SC, et al. Achievement of LDL-C targets defined by ESC/EAS (2011) guidelines in risk-stratified Korean patients with dyslipidemia receiving lipid-modifying treatments. Endocrinol Metab (Seoul) 2020;35:367-76.ArticlePubMedPMCPDF
- 28. Hwang JY, Jung CH, Lee WJ, Park CY, Kim SR, Yoon KH, et al. Low density lipoprotein cholesterol target goal attainment rate and physician perceptions about target goal achievement in Korean patients with diabetes. Diabetes Metab J 2011;35:628-36.ArticlePubMedPMC
- 29. Charlton-Menys V, Betteridge DJ, Colhoun H, Fuller J, France M, Hitman GA, et al. Targets of statin therapy: LDL cholesterol, non-HDL cholesterol, and apolipoprotein B in type 2 diabetes in the Collaborative Atorvastatin Diabetes Study (CARDS). Clin Chem 2009;55:473-80.ArticlePubMedPDF
- 30. Triglyceride Coronary Disease Genetics Consortium and Emerging Risk Factors Collaboration. Triglyceride-mediated pathways and coronary disease: collaborative analysis of 101 studies. Lancet 2010;375:1634-9.ArticlePubMedPMC
- 31. Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults. Executive summary of the third report of the National Cholesterol Education Program (NCEP) expert panel on detection, evaluation, and treatment of high blood cholesterol in adults (Adult Treatment Panel III). JAMA 2001;285:2486-97.ArticlePubMed
- 32. Grundy SM, Cleeman JI, Merz CN, Brewer HB, Clark LT, Hunninghake DB, et al. Implications of recent clinical trials for the National Cholesterol Education Program Adult Treatment Panel III guidelines. Circulation 2004;110:227-39.ArticlePubMed
- 33. Gordon DJ, Probstfield JL, Garrison RJ, Neaton JD, Castelli WP, Knoke JD, et al. High-density lipoprotein cholesterol and cardiovascular disease: four prospective American studies. Circulation 1989;79:8-15.ArticlePubMed
- 34. Estruch R, Ros E, Salas-Salvado J, Covas MI, Corella D, Aros F, et al. Primary prevention of cardiovascular disease with a Mediterranean diet supplemented with extra-virgin olive oil or nuts. N Engl J Med 2018;378:e34.ArticlePubMed
- 35. Franz MJ, Boucher JL, Rutten-Ramos S, VanWormer JJ. Lifestyle weight-loss intervention outcomes in overweight and obese adults with type 2 diabetes: a systematic review and meta-analysis of randomized clinical trials. J Acad Nutr Diet 2015;115:1447-63.ArticlePubMed
- 36. Hur KY, Moon MK, Park JS, Kim SK, Lee SH, Yun JS, et al. 2021 Clinical practice guidelines for diabetes mellitus of the Korean Diabetes Association. Diabetes Metab J 2021;45:461-81.ArticlePubMedPMCPDF
- 37. Rhee EJ, Kim HC, Kim JH, Lee EY, Kim BJ, Kim EM, et al. 2018 Guidelines for the management of dyslipidemia in Korea. J Lipid Atheroscler 2019;8:78-131.ArticlePubMedPMCPDF
- 38. Ben-Yehuda O, Wenger NK, Constance C, Zieve F, Hanson ME, Lin JX, et al. The comparative efficacy of ezetimibe added to atorvastatin 10 mg versus uptitration to atorvastatin 40 mg in subgroups of patients aged 65 to 74 years or greater than or equal to 75 years. J Geriatr Cardiol 2011;8:1-11.ArticlePubMedPMC
- 39. Bays HE, Conard SE, Leiter LA, Bird SR, Lowe RS, Tershakovec AM. Influence of age, gender, and race on the efficacy of adding ezetimibe to atorvastatin vs. atorvastatin up-titration in patients at moderately high or high risk for coronary heart disease. Int J Cardiol 2011;153:141-7.ArticlePubMed
- 40. Zhang XL, Zhu QQ, Zhu L, Chen JZ, Chen QH, Li GN, et al. Safety and efficacy of anti-PCSK9 antibodies: a meta-analysis of 25 randomized, controlled trials. BMC Med 2015;13:123.ArticlePubMedPMCPDF
- 41. Rosenson RS, Daviglus ML, Handelsman Y, Pozzilli P, Bays H, Monsalvo ML, et al. Efficacy and safety of evolocumab in individuals with type 2 diabetes mellitus: primary results of the randomized controlled BANTING study. Diabetologia 2019;62:948-58.ArticlePubMedPMCPDF
- 42. Moriarty PM, Jacobson TA, Bruckert E, Thompson PD, Guyton JR, Baccara-Dinet MT, et al. Efficacy and safety of alirocumab, a monoclonal antibody to PCSK9, in statin-intolerant patients: design and rationale of ODYSSEY ALTERNATIVE, a randomized phase 3 trial. J Clin Lipidol 2014;8:554-61.ArticlePubMed
- 43. Guedeney P, Giustino G, Sorrentino S, Claessen BE, Camaj A, Kalkman DN, et al. Efficacy and safety of alirocumab and evolocumab: a systematic review and meta-analysis of randomized controlled trials. Eur Heart J 2022;43:e17-25.ArticlePubMedPDF
- 44. Bhatt DL, Steg PG, Miller M, Brinton EA, Jacobson TA, Ketchum SB, et al. Cardiovascular risk reduction with icosapent ethyl for hypertriglyceridemia. N Engl J Med 2019;380:11-22.ArticlePubMed
- 45. Nicholls SJ, Lincoff AM, Garcia M, Bash D, Ballantyne CM, Barter PJ, et al. Effect of high-dose omega-3 fatty acids vs corn oil on major adverse cardiovascular events in patients at high cardiovascular risk: the STRENGTH randomized clinical trial. JAMA 2020;324:2268-80.ArticlePubMedPMC
- 46. ACCORD Study Group. Effects of combination lipid therapy in type 2 diabetes mellitus. N Engl J Med 2010;362:1563-74.ArticlePubMedPMC
- 47. Scott R, O’Brien R, Fulcher G, Pardy C, D’Emden M, Tse D, et al. Effects of fenofibrate treatment on cardiovascular disease risk in 9,795 individuals with type 2 diabetes and various components of the metabolic syndrome: the Fenofibrate Intervention and Event Lowering in Diabetes (FIELD) study. Diabetes Care 2009;32:493-8.PubMedPMC
- 48. Hermans MP. Impact of fenofibrate on type 2 diabetes patients with features of the metabolic syndrome: subgroup analysis from FIELD. Curr Cardiol Rev 2010;6:112-8.ArticlePubMedPMC
- 49. Koopal C, Visseren FL, Westerink J, van der Graaf Y, Ginsberg HN, Keech AC. Predicting the effect of fenofibrate on cardiovascular risk for individual patients with type 2 diabetes. Diabetes Care 2018;41:1244-50.ArticlePubMedPDF
- 50. Kim NH, Han KH, Choi J, Lee J, Kim SG. Use of fenofibrate on cardiovascular outcomes in statin users with metabolic syndrome: propensity matched cohort study. BMJ 2019;366:l5125.ArticlePubMedPMC
- 51. Das Pradhan A, Glynn RJ, Fruchart JC, MacFadyen JG, Zaharris ES, Everett BM, et al. Triglyceride lowering with pemafibrate to reduce cardiovascular risk. N Engl J Med 2022;387:1923-34.ArticlePubMed
- 52. Stone NJ, Robinson JG, Lichtenstein AH, Bairey Merz CN, Blum CB, Eckel RH, et al. 2013 ACC/AHA guideline on the treatment of blood cholesterol to reduce atherosclerotic cardiovascular risk in adults: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol 2014;63(25 Pt B):2889-934.PubMed
- 53. Berglund L, Brunzell JD, Goldberg AC, Goldberg IJ, Sacks F, Murad MH, et al. Evaluation and treatment of hypertriglyceridemia: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab 2012;97:2969-89.ArticlePubMedPMC
- 54. American Diabetes Association Professional Practice Committee. 10. Cardiovascular disease and risk management: standards of medical care in diabetes-2022. Diabetes Care 2022;45(Suppl 1):S144-74.ArticlePubMedPDF
- 55. Lee KH, Jeong MH, Kim HM, Ahn Y, Kim JH, Chae SC, et al. Benefit of early statin therapy in patients with acute myocardial infarction who have extremely low low-density lipoprotein cholesterol. J Am Coll Cardiol 2011;58:1664-71.ArticlePubMed
- 56. Kim MK, Han K, Joung HN, Baek KH, Song KH, Kwon HS. Cholesterol levels and development of cardiovascular disease in Koreans with type 2 diabetes mellitus and without pre-existing cardiovascular disease. Cardiovasc Diabetol 2019;18:139.ArticlePubMedPMCPDF
- 57. Huh JH, Park SW, Go TH, Kang DR, Lee SH, Kim JY. Optimal low-density lipoprotein cholesterol levels in adults without diabetes mellitus: a nationwide population-based study including more than 4 million individuals from South Korea. Front Cardiovasc Med 2022;8:812416.ArticlePubMedPMC
- 58. Ahn JH, Ahn Y, Jeong MH, Kim JH, Hong YJ, Sim DS, et al. Optimal low-density lipoprotein cholesterol target level in Korean acute myocardial infarction patients (<70 mg/dL vs. <55 mg/dL): based on Korea acute myocardial infarction registry-National Institute of Health. Int J Cardiol 2022;351:15-22.ArticlePubMed
REFERENCES
Figure & Data
References
Citations

- Associations of omega-3 fatty acids vs. fenofibrate with adverse cardiovascular outcomes in people with metabolic syndrome: propensity matched cohort study
Nam Hoon Kim, Ji Yoon Kim, Jimi Choi, Sin Gon Kim
European Heart Journal - Cardiovascular Pharmacotherapy.2024; 10(2): 118. CrossRef - Clinical Characteristics of Patients With Statin Discontinuation in Korea: A Nationwide Population-Based Study
Kyung-Soo Kim, Sangmo Hong, Kyungdo Han, Cheol-Young Park
Journal of Lipid and Atherosclerosis.2024; 13(1): 41. CrossRef - Role of Fenofibrate Use in Dyslipidemia and Related Comorbidities in the Asian Population: A Narrative Review
Chaicharn Deerochanawong, Sin Gon Kim, Yu-Cheng Chang
Diabetes & Metabolism Journal.2024; 48(2): 184. CrossRef - Dyslipidemia Fact Sheet in South Korea, 2022
Eun-Sun Jin, Jee-Seon Shim, Sung Eun Kim, Jae Hyun Bae, Shinae Kang, Jong Chul Won, Min-Jeong Shin, Heung Yong Jin, Jenny Moon, Hokyou Lee, Hyeon Chang Kim, In-Kyung Jeong
Diabetes & Metabolism Journal.2023; 47(5): 632. CrossRef - 2023 Clinical Practice Guidelines for Diabetes
Min Kyong Moon
The Journal of Korean Diabetes.2023; 24(3): 120. CrossRef - 2023 Clinical Practice Guidelines for Diabetes Mellitus of the Korean Diabetes Association
Jong Han Choi, Kyung Ae Lee, Joon Ho Moon, Suk Chon, Dae Jung Kim, Hyun Jin Kim, Nan Hee Kim, Ji A Seo, Mee Kyoung Kim, Jeong Hyun Lim, YoonJu Song, Ye Seul Yang, Jae Hyeon Kim, You-Bin Lee, Junghyun Noh, Kyu Yeon Hur, Jong Suk Park, Sang Youl Rhee, Hae J
Diabetes & Metabolism Journal.2023; 47(5): 575. CrossRef - Management of Dyslipidemia in Patients with Diabetes Mellitus
Kyung Ae Lee
The Journal of Korean Diabetes.2023; 24(3): 111. CrossRef - 2023 Clinical Practice Guidelines for Diabetes: Management of Cardiovascular Risk Factors
Ye Seul Yang
The Journal of Korean Diabetes.2023; 24(3): 135. CrossRef - Dyslipidemia Fact Sheet in South Korea, 2022
Eun-Sun Jin, Jee-Seon Shim, Sung Eun Kim, Jae Hyun Bae, Shinae Kang, Jong Chul Won, Min-Jeong Shin, Heung Yong Jin, Jenny Moon, Hokyou Lee, Hyeon Chang Kim, In-Kyung Jeong
Journal of Lipid and Atherosclerosis.2023; 12(3): 237. CrossRef
- Figure
- Related articles
-
- Evaluation and Management of Patients with Diabetes and Heart Failure: A Korean Diabetes Association and Korean Society of Heart Failure Consensus Statement
- Comprehensive Understanding for Application in Korean Patients with Type 2 Diabetes Mellitus of the Consensus Statement on Carbohydrate-Restricted Diets by Korean Diabetes Association, Korean Society for the Study of Obesity, and Korean Society of Hypertension

 KDA
KDA
 PubReader
PubReader ePub Link
ePub Link Cite
Cite